Outcome of Patients Discharged after their First Detected Episode of Atrial Fibrillation
Sophie Gomes MD, Laure Champ-Rigot MD, Anthony Foucault MD, Pellissier MD Arnaud, Alain Lebon MD, Patrice Scanu MD, Paul Milliez MD, PhD
Cardiology Department, Caen University Hospital, Normandy, France
.
Atrial fibrillation (AF) is the most frequent supraventricular arrhythmia with an approximative prevalence of 1 % in the general population and above 6 % in the elderly. After a first AF diagnosis, the hospitalization rate is markedly increased. Management of a first AF episode is different depending on the clinical status of patients. Practical guidelines developed in collaboration with the European Heart Rhythm Association and the Heart Rhythm Society are available for the management of these patients. A four-step decisional scheme must be followed in the management of a first recent AF episode: need for a short- and long-term anticoagulation, define a rythmologic strategy (rhythm or rate control), select the weapon (drug, device or ablation) and reconsider the strategy if needed. After a first uncomplicated paroxysmal AF episode, guidelines recommend that prescription of antiarrhythmics must be avoided and anticoagulation is optional. After a first persistent AF episode, guidelines recommend to either respect or reduce the arrhythmia. Prescription of antiarrhythmics and anticoagulation is also optional depending on the patient?s condition. In case of the AF reduction decision, anticoagulation must be tailored preliminary to this reduction. AF recurrence rate varies depending on the patient?s condition, and the risk of stroke assessed by the CHA2DS2-VASc score might be similarly considered for both paroxysmal and persistent AF.
Correspondence to: Sophie Gomes, MD, Cardiology Department Caen University Hospital, Avenue de la Cote de Nacre, Normandy 14033 Caen, France.
Atrial fibrillation (AF) is the most common supraventricular arrhythmia. After the onset of AF, changes of atrial electrophysiological properties, mechanical function, and atrial structure occur with different time courses and with different pathophysiological consequences. Consequently, these modifications underlie the tolerance and the occurrence of potential complications, and must be the source of important therapeutic decisions. Among different clinical criteria, the nature of AF (paroxysmal, persistent or permanent), the existence of disable symptoms, of an underlying heart disease and/or embolic risk factors, play an important role in the management of the appropriate medications. Practical recommendations developed in collaboration with the European Heart Rhythm Association and the Heart Rhythm Society help us to manage the first episode of AF; however, there are still some obscurities in these recommendations that we will be discussed below based on the nature of paroxysmal or persistent AF.1,2
Epidemiology of First Episode of AF
AF affects approximately 1% of the general population and accounts for more than a third of hospitalizations in the United States for heart rhythm disorders.3 First detected episode of AF represents 11% of all types of AF.4 Because AF may be asymptomatic (silent AF) and as a result undiagnosed, the “true” prevalence of AF is probably closer to 2% of the population.5
New onset AF often spontaneously reverts to normal sinus rhythm, with the incidence of reversion related to the duration of the arrhythmia.Spontaneous conversion to sinus rhythm occurs in almost 70% of patients presenting with atrial fibrillation of less than 72 hours duration, and presentation with symptoms of less than 24 hours duration is the best predictor of spontaneous conversion in a large prospective observational study.6
After the initial diagnosis of AF, the likelihood of hospitalization increases during the first year of AF. Advancing age, greater body mass index, hypertension, paroxysmal AF (vs permanent/persistent AF) at initial diagnosis, history of myocardial infarction, valvular heart disease, peripheral or carotid artery disease, stroke, diabetes mellitus, chronic renal disease, and chronic obstructive pulmonary disease are significant independent predictors of hospitalisation after a first detected episode of AF. The main causes of hospital admission are AF related congestive heart failure, coronary or peripheral arterial causes, and thromboembolic events.7A first detected episode of AF appears a marker for underlying cardiac diseases.8 Moreover, new onset of AF is associated with an increased mortality.8,9
Patients with AF have an increased risk of stroke, often with more severe form, and with a higher rate of recurrence.10 Stroke in AF is often severe and can result in long-term disability or death.11 Undiagnosed silent AF is a likely cause of some “cryptogenic” strokes. Furthermore, it is important to know that regardless of the type of AF (paroxysmal or permanent), the embolic risk is comparable. Hence, patients with paroxysmal AF should be regarded as having a stroke risk similar to those with persistent or permanent AF, in the presence of risk factors detailed below. Moreover, cognitive impairment may be related to AF, through silent embolic events.12 Finally, if AF can affect patients without underlying heart disease (also called “idiopathic AF” or “lone AF”), it occurs mainly in patients with a structural cardiomyopathy secondary to hypertension, valvular or coronary artery disease.9 A small sample observational study, but with a 12 year follow-up, confirms the favourable prognosis of newly-diagnosed lone AF. However, develoment of an underlying heart disease and arrythmia progression are risks factors of cardiovascular events, including stroke.13
Types of Atrial Fibrillation
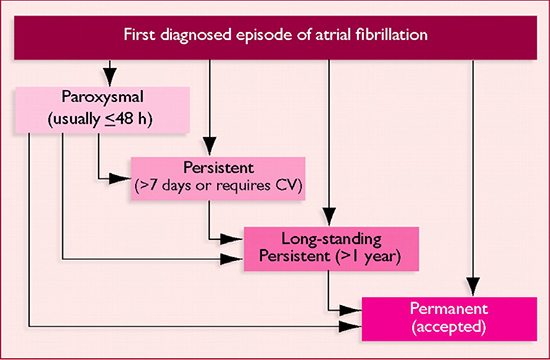
According to recent European Society of Cardiology (ESC) guidelines,2 five types of AF based on the clinical presentation and duration of the arrhythmia can be described: first diagnosed paroxysmal, persistent, long-standing persistent, and permanent AF (Figure 1).
1. First Diagnosed AF is every AF identified for the first time by an electrocardiogram (ECG) or other electrocardiographic rhythm recording device, irrespective of the duration of the arrhythmia or the presence and severity of AF-related symptoms.
2. Paroxysmal AF is self-terminating in less than 7 days, usually within 48 h.
3. Persistent AF is present when an AF episode either lasts longer than 7 days or requires termination by cardioversion (CV), either with drugs, or direct current cardioversion (DCC).
4. Long-Standing Persistent AF lasts for one year or more when it has been decided to adopt a rhythm control strategy.
5. Permanent AF is considered to be present if the arrhythmia lasts for more than one year and cardioversion either has not been attempted or has failed, or if the arrhythmia is accepted by the patient (and physician).
The pathogenesis of AF underlines the importance of slowly developing structural changes preceding a newly documented episode of AF episode. The idea that “AF begets AF” through complex electrophysiological and structural remodeling of the atria suggests that early treatment of AF should be considered associated with early, aggressive intervention on factors such as hypertension, obesity or sleep apnoea, in an attempt to prevent atrial remodeling, and so AF recurrences.14,15 A prospective study on 106 patients with first AF showed that half of the patients had no further recurrence after 5 years, but that patients with comorbidities are at higher risk for rapid progression to permanent AF.16
Paroxysmal AF recurrences vary markedly from one patient to another. Silent AF (asymptomatic) is common even in symptomatic patients.5 It may look like any of the temporal forms (paroxysmal, persistent or permanent) of AF. It may also manifest as an AF-related complication (ischaemic stroke or tachycardiomyopathy) or may be diagnosed by an opportunistic ECG. A recent meta-analysis showed that, in patients with an implanted device (pace-maker or internal defibrillator) asymptomatic atrial tachyarrhythmias, without clinical atrial fibrillation, were associated with a significantly increased risk of ischemic stroke or systemic embolism.17 This has important implications for management of therapies aimed at preventing AF-related complications.
Figure 1. Different types of AF. First-onset AF may be the first of recurrent attacks or already be deemed permanent. (from [2])
Several instruments are useful to assess AF episode recurrence, their duration or ventricular response rates. Continuous ambulatory ECG recording for 24 hours to 7 days or more, or event recorders are used to identify the arrhythmia if it is intermittent and not captured on routine electrocardiography.18 Finally, AF can occur under specific conditions such as acute coronary syndrome, hyperthyroidism, valve replacement, fever, etc. For instance, new onset of AF occuring during acute myocardial infarction is a risk factor of stroke and prescription of OAC dramatically decreases the rate of stroke.19 Among patients with severe sepsis, patients with new-onset AF were at increased risk of in-hospital stroke and death compared with patients with no AF and patients with preexisting AF.20 In hyperthyroid patients who presented with new-onset AF, there was an increased risk of ischemic stroke during the initial phase of presentation.21 So, AF in such conditions should not be regarded as a benign, transient complication of the acute event.
Management of a First Detected Episode of AF
A complete history and physical examination should be performed in all patients with new onset AF. There should be an assessment for an underlying cause, such as heart failure, pulmonary disease, alcohol, fever, or hyperthyroidism. Therapy for a precipitating cause should be initiated prior to cardioversion in stable patients and may result in reversion to sinus rhythm. Antithrombotic treatment will be discussed below.
Time to onset of the episode should be accurately established. It’s also important to weigh the risk/benefit ratio of these potential therapeutics in reducing morbidity and mortality of these patients with a first episode of AF to answer the following questions:
-Should I prevent complications related to the AF, including embolic?
-Does the patient have symptoms? If so, should I remove them?
-Should I prescribe an anti-arrhythmic (AA) treatment?
Thus, a 4-point strategy decision must be proposed in the context of this first episode:
-Discuss the need for a prescription of anticoagulant or anti-aggregation-Choose rate versus rhythm control strategy.
-Select a therapeutic weapon: AA, rate slowing drugs
Consider a new strategy in case of failure
By asking these four questions, we barely just have to follow the ACC/AHA/HRS and ESC 2011 guidelines on management of a first episode of AF and apply these according to history and clinical status of the patient.1,2 We will detail below those recommendations based on the nature of paroxysmal or persistent AF.
Management of the First Episode of Paroxysmal AF
As already said, the thrombo-embolic risk in paroxysmal AF does not differ from persistent or permanent forms, and is present especially in case of underlying cause of AF.19-21 Therefore, every patient with paroxysmal AF should be assessed carefully for the risk of stroke and should be screened to receive oral anti-thrombotic therapy (anticoagulation or anti-aggregation) according to their risk score.
The previously used CHADS2 score does not include many stroke risk factors, and other “stroke risk modifiers” are considered in a comprehensive stroke risk assessment resulting in a new risk factor-based approach for patients with non-valvular AF, also expressed as an acronym, CHA2DS2-VASc (Table 1).22 “Major” risk factors are prior stroke, transient ischemic attack (TIA) or thrombo-embolism, and older age (≥75 years). The presence of some types of valvular heart disease (mitral stenosis or prosthetic heart valves) would also categorize such “valvular” AF patients as “high risk” and require oral anti-coagulation (OAC). “Clinically relevant non-major” risk factors are heart failure, hypertension, or diabetes, female sex, age between 65 and 74 years, and vascular disease (myocardial infarction, complex aortic plaque, peripheral artery disease). Risk factors are cumulative, and the simultaneous presence of two or more “clinically relevant non-major” risk factors would vindicate a stroke risk that is high enough to require anticoagulation. In patients with a CHA2DS2-VASc score of ≥2, chronic OAC therapy (vitamin K antagonists), is recommended in a dose adjusted to achieve an INR value in the range of 2–3, unless contraindicated. New OAC drugs, such as dabigatran, may ultimately be considered.23
Table 1. Risk factor-based approach expressed as a point based scoring system, with the acronym CHA2DS2-VASc (maximum score is 9 since age may contribute 0, 1, or 2 point) (from [2])
| Risk Factor |
Score |
| Congestive heart failure, LV dysfunction <40% |
1 |
| Hypertension |
1 |
| Age > 75 |
2 |
| Diabetes mellitus |
1 |
| Stroke/TIA/thrombo-embolism |
2 |
| Vascular disease |
1 |
| Age between 65 and 74 |
1 |
| Female sex |
1 |
In patients with a CHA2DS2-VASc score of 1, we may consider OAC or aspirin, after evaluation of the risk of bleeding complications, ability to safely sustain adjusted chronic anticoagulation, and patient preferences. In patients with a CHA2DS2-VASc score of 0, it is recommended to consider no antithrombotic therapy rather than aspirin (Table 2).
Table 2. Approach to thromboprophylaxis in patients with AF according to their CHA2DS2-VASc score (from [2])
| CHA2DS2-VASc Score |
Recommended Antithrombotic Therapy |
| ≥ 2 <40% |
OAC |
| 1 |
Either OAC or aspirin |
| 0 |
Either aspirin or no antothrombotic therapy |
However, these recommendations are not so concerning about the anticoagulation after a first isolated episode of paroxysmal AF, because of the remote risk of embolism (admittedly rare) due to atrial stunning post-AF reduction.24
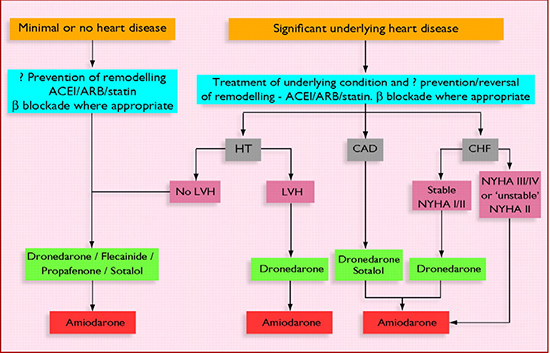
In the situation of a first episode of paroxysmal AF, the issue of rate versus rhythm control is not standing here because of the self-terminated AF episode by definition. The only question is whether or not there is a place for an AA treatment. First detected AF is the most symptomatic type of AF, with paroxysmal AF. The lack of control of heart rate is possibly responsible for the more symptomatic nature of the first episode of AF.4 Palpitations, chest pain and shortness of breath must not justify an AA prescription, even in the presence of either a minimal, either a significant underlying heart disease, but we should take into account patients comorbidities such as age or diabetes.16 Conversely, if critical symptoms occur at the time of the AF episode, such as anginal pain, hypotension or heart failure, that are usually observed in the setting of an advanced or unstable underlying cardiomyopathy, the prescription of an AA treatment is undoubtedly recommended. This rhythm control strategy is based on different antiarrhythmic drug therapy such as dronedarone, sotalol, flecainide, propafenone or amiodarone. The choice of the first line AA therapy should take into account whether or not the patient has significant underlying heart disease. (Figure 2). Catheter ablation could be an alternative to AA drugs as a first-line therapy of AF, because of patient preference or contra-indication to AA drugs. A recent study showed that ablative therapy performed at an earlier stage of the disease was associated with a significantly higher success rate and with a decreased need for repeat procedures.25 Another study proposed a cryoballoon ablation as first-line treatment of lone paroxysmal AF, with good results on short-term AF recurrence.26
Figure 2. Choice of antiarrhythmic drug according to underlying pathology (from [2])
Management of the First Episode of Persistent AF
Persistent AF is present when an AF episode either lasts longer than 7 days or requires termination by cardioversion. For most patients in whom the duration of new onset AF is suspected to be more than 48 hours (or when the duration is unknown),6the risk of embolization is substantially increased, and it is preferable to anticoagulate and use transesophageal echo (TEE) to rule out left atrial thrombi before attempting cardioversion. If TEE is not available, then anticoagulation for approximately three to four weeks is preferable to allow any left atrial thrombi to resolve.27 This recommendation includes patients with a low CHADS2 score (0 or 1). Because of delayed return of atrial mechanical function (atrial stunning) after cardioversion, it could increase the risk of a thromboembolic event after this approach with cardioversion.24 Even with the lower CHADS2 score, oral anticoagulation is recommended for at least 4 weeks after cardioversion that is electrical, chemical or even more after catheter ablation. An alternative approach to four weeks of OAC therapy is to perform a transesophageal echocardiography (TEE) to rule out the presence of any thrombi prior to cardioversion. The recent ACUTE trial has compared both strategies. ACUTE directly compared a TEE-guided strategy to the conventional strategy in patients with AF of more than 48 hours duration who were undergoing electrical cardioversion.28 There was no difference in the incidence of stroke or thromboembolic events within eight weeks of cardioversion, but patients undergoing the TEE-guided strategy had a lower incidence of hemorrhagic events and a greater incidence of successful reversion.
Delayed cardioversion and anticoagulation is reasonable for patients who have an associated mitralattivalve disease, significant cardiomyopathy, heart failure, a prior history of a thromboembolic event or of transesophageal echocardiography evidence of left atrial thrombus. 29
Rate Versus Rhythm Control
Before considering rate or rhythm control strategy, an important question should be discussed: is there a need for urgent or emergent cardioversion? In four critically clinical situations this matter must considered:
- Active ischemia (symptomatic or electrocardiographic evidence)- Evidence for organ hypoperfusion - Severe manifestations of heart failure - Presence of a preexcitation syndrome, which may lead to an extremely rapid ventricular rate due to the presence of an accessory pathway
In a patient with any of these indications for urgent cardioversion, the need for restoration of sinus rhythm takes precedence over the need for protection from thromboembolic risk. Intravenous anticoagulation with heparin should be started, but it should not cause a delay in emergent cardioversion.
In the absence of urgent cardioversion, most patients who present with AF will require slowing of the ventricular rate to improve symptoms. Then a decision regarding the long-term approach to the management of the rhythm disturbance (rhythm versus rate control) should be made. Two studies, AFFIRM and RACE, show evidence that rhythm and rate control strategies are associated with similar rates of mortality and serious morbidity, such as embolic risk.30,31 In addition, assessments of quality of life have not shown significant differences between the two in most studies. However, after a first episode of persistent AF, owing to the natural time course of AF and its consequences, a rhythm control strategy should reasonably be chosen first with a set routine, with the exception of patients who are completely asymptomatic, and particularly those who are very old (>80 years). Indeed, in patients with multiple comorbidities, the risk of undergoing cardioversion or using AA drugs may outweigh the benefits of restoring sinus rhythm. The rhythm control strategy uses the6same drugs as described above (Figure 2).
Rate slowing drugs are generally started before rhythm control strategy in patients with either excessive heart rate or disabling symptoms and are sometimes continued in patients who remain are sinus rhythm (in the event of AF recurrence). The rate control strategy generally uses drugs that slow conduction across the atrioventricular (AV) node, such as beta blockers, rate slowing calcium channel blockers, or digoxin.
Finally, in case of failure in the reduction of a first episode of persistent AF, before abandoning the idea of reduction of the AF, a new shock after antiarrythmic impregnation could be performed with a high-energy biphasic antero-posterior thoracic shock (300 Joules). 32 Several AA drugs have proved their efficacity in facilitating cardioversion, such as ibutilide, amiodarone, and propafenone.33-35 Moreover, continuous use of Class Ic drugs or amiodarone appears to be an independent predictor of sinus rhythm at 1-year follow-up after cardioversion.36 In case of reccurent symptomatic, persistent AF, with major symptoms, or AF-related LV dysfunction, a left atrial (LA) catheter ablation could be proposed. There is evidence that patients with heart failure benefit from LA ablation as the ejection fraction and exercise tolerance may improve significantly.37,38 However, in such patients, successful ablation is more difficult to achieve, and often requires several attempts. The procedure can be long and technically challenging, and is associated with greater risk than pulmonary vein isolation alone. Hence, major symptoms should be present to vindicate those procedures.
Management of a first detected episode of AF is driven by US and European recommendations, but there are certain specific conditions, particularly with anti-thrombotic drugs, where a determined attitude is impossible. The first episode of AF can occur with a infraclinic preexisting atrial remodeling, which may move to recurrence, or persistent AF, with their well-known adverse outcomes. Thus, it is essential to focus on detection of AF and treatment of underlying heart disease, considering the use of upstream therapy.39 Regarding the antiarrythmic therapy, our attitude must be tailored to each patient according to its symptoms, its land, its embolic risk and we must not hesitate to challenge the published recommendations according to evolution of AF.