How Do Atrial-Selective Drugs Differ From
Antiarrhythmic Drugs Currently
Used in the Treatment of Atrial Fibrillation?
Alexander Burashnikov, Charles Antzelevitch
Masonic Medical Research Laboratory, Utica, NY.
Current pharmacologic strategies for the management of atrial fibrillation (AF) include use of 1) sodium channel blockers, which are contraindicated in patients with coronary artery or structural heart disease because of their potent effect to slow conduction in the ventricles, 2) potassium channel blockers, which predispose to acquired long QT and Torsade de Pointes arrhythmias because of their potent effect to prolong ventricular repolarization, and 3) mixed ion channel blockers such as amiodarone, which are associated with multi-organ toxicity. Accordingly, recent studies have focused on agents that selectively affect the atria but not the ventricles. Several atrial-selective approaches have been proposed for the management of AF, including inhibition of the atrial-specific ultrarapid delayed rectified potassium current (IKur), acetylcholine-regulated inward rectifying potassium current (IK-ACh), or connexin-40 (Cx40). All three are largely exclusive to atria. Recent studies have proposed that an atrial-selective depression of sodium channel-dependent parameters with agents such as ranolazine may be an alternative approach capable of effectively suppressing AF without increasing susceptibility to ventricular arrhythmias. Clinical evidence for Cx40 modulation or IK-ACh inhibition are lacking at this time. The available data suggest that atrial-selective approaches involving a combination of INa, IKur, IKr, and, perhaps, Ito block may be more effective in the management of AF than pure IKur or INa block. The anti-AF efficacy of the atrial-selective/predominant agents appears to be similar to that of conventionally used anti-AF agents, with the major apparent difference being that the latter are associated with ventricular arrhythmogenesis and extracardiac toxicity.
Correspondence to: Dr. Alexander Burashnikov, PhD , Masonic Medical Research Laboratory: 2150 Bleecker Street,Utica, N.Y. 13501. Phone: (315)735-2217, Fax: (315)735-5648, Charles Antzelevitch, PhD, FACC, FAHA, FHRS,Executive Director and Director of Research,Gordon K. MoeScholar, 2150 Bleecker Street,Utica, N.Y. 13501.
The development of atrial-selective antiarrhythmic agents was necessitated by the proclivity for induction of life-threatening ventricular arrhythmias and/or extra-cardiac toxicity of currently available anti-atrial fibrillation (AF) agents. This review is an attempt to briefly summarize currently current knowledge relative to this effort.
It has been more that decade since Wang et al1 first described the ultrarapid delayed rectified potassium current (IKur, carried by Kv 1.5 channels encoded by the KCNA5 gene) which is present only in atria, but not ventricles. Block of IKur affects only atrial electrical parameters, which makes this current a potential target for chamber-specific management of atrial arrhythmias.2 Among other atrial specific targets suggested to be used for the suppression of atrial arrhythmias is the acetylcholine (ACh)-regulated inward rectifying potassium current (IK-ACh), encoded by Kir3.1/3.4 alpha-subunits) and, to a certain degree, connexin 40 (Cx40, encoded by GjA5and).2-4
Most recently, another approach has been proposed for the management of AF, consisting of atrial-selective/predominant depression of sodium channel current (INa)-dependent parameters. INa blockers, such as ranolazine, which predominantly or selectively, depresses INa-dependent parameters in atria vs. ventricles.5 Ranolazine has been shown be effective in suppressing AF in a variety of experimental models5 as well as reducing supraventricular arrhythmias (p<0.001) and new onset AF (p=0.08) in patients with non-ST segment elevation acute coronary syndrome.6 Block of IKr has also been shown to cause a preferential prolongation of atrial vs. ventricular repolarization.7-13
Atrial-Specific Antiarrhythmic Approaches for AF
Atrial-specific targets are those that are present exclusively or almost exclusively in atria. Atrial-specific agents include those that inhibit IKur and IK(ACh). Agents that modulate Cx40, found in atrial but not ventricular myocardium, are commonly included in this category with the caveat that Cx40 is present in the conduction system of the ventricles.2,4 While it is conceivable that an effect on Cx40 may suppress some forms of AF, there are no specific Cx40 inhibitors available yet, so that the hypothesis remains to be tested.
Vagally-mediated AF is the most likely form of AF to be suppressed by IK-ACh inhibition. A vagal component may also contribute to the initiation of paroxysmal AF.14,15 Normally, IK-ACh is activated through the muscarinic receptors in response to release of ACh, leading to an abbreviation of atrial repolarization and, thereby, promoting AF. In the atria of human patients with chronic AF, ACh-activated IK-ACh is reported to be either increased16 or decreased.3 There is another form of IK-ACh that does not require vagal influences or muscarinic receptors for activation, i.e., the constitutively active IK-ACh.17-19 This current is present in normal human atria and is significantly increased in atria of chronic AF patients.18,19 In canine atria, a corresponding constitutively active IK-ACh is also present under baseline conditions and this current is up-regulated in tachycardia-remodeled atria.17,20 The constitutively active IK-ACh is likely to contribute to abbreviation of atrial APD and AF vulnerability.18-20 Selective block of IK-ACh with tertiapin prolongs atrial APD and suppresses AF in experimental AF models.20,21 Block of IK-ACh, however, may be pro-arrhythmic in post-operative AF cases, since the preservation of the anterior fat pad (containing mostly parasympathetic nerves endings) decreases the incidence of postoperative AF.22 There are no clinically available selective IK-ACh blockers at the present time. An important caveat in the development of clinically safe IK-ACh blockers is that these agents should not produce significant vagolytic influences in other organs. Thus, the clinical feasibility of an “IKA-Ch approach” is yet to be established.
Among atrial-specific targets, IKur is the most investigated and is considered by many as the most promising target at the present time. The pharmacological response of “healthy” and “remodeled” atria (displaying a plateau-shaped and triangular-shaped AP morphology, respectively) to IKur block is very different (Fig. 1).23,24 Block of IKur in “healthy” atria prolongs only the early repolarization phase but abbreviates the late repolarization phase (APD70 or APD90) and the effective refractory period (ERP)23-25 In contrast, in remodeled atria, a reduction of IKur prolongs APD70-90.23 Interestingly, loss-of-function mutations in KCNA5, the gene that encodes the Kv1.5 channel protein, have been associated with familial AF,26 suggesting that a reduction in IKur may predispose to the development of AF. In support of this hypothesis, block of IKur with 10-50 µM of 4-AP was shown to promote the induction of non-sustained AF in “healthy” canine arterially-perfused atrial preparations, secondary to the development of an abbreviation of APD90 and ERP.25
Figure 1. Block of IKur with 4-aminopyridine (4- AP, 50 μM)
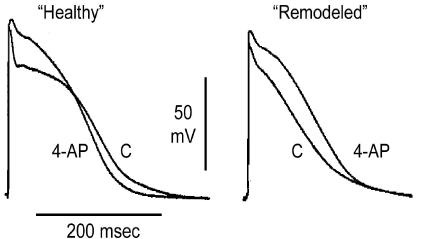
abbreviates APD90 in “healthy” (plateau-shaped action potential), but prolongs it in “acutely remodeled” (triangular-shaped action potential) canine coronary-per fused Atrial preparations (pectinate muscles). Low flow ischemia was used to generate the “acutely remodeled” atria. Left panel is from Burashnikov et al.,24 with permission.
A number of studies have demonstrated that agents capable of blocking IKur (AVE0118, AVE1231, S9947, S20951, ISQ-1, DPO-1, vernakalant; AZD7009; NIP141, NIP-142) selectively prolong atrial ERP both in electrically-remodeled and non-remodeled (i.e., “healthy”) atria in vivo and in vitro.27-34 Because ERP prolongation in “healthy” atria is not consistent with APD70-90 abbreviation recorded in “healthy” atrial preparations in vitro,23-25 the ERP prolongation observed in response to these agents may be related to their action to also depress INa. Prolongation of ERP in the absence of APD90 prolongation is a well-known feature of sodium, but not potassium, channel blockade. This is the result of post-repolarization refractoriness (PRR), which develops more readily in atria than in the ventricles (Fig. 2).35,35,36 Consistent with this line of thinking, IKur blockers such as AZD7009 and vernakalant have been also shown to be capable of potently block INa.32,37,38 AZD7009 has been shown to behave as an atrial selective INa blocker in the canine heart in vivo, slowing conduction velocity and increasing diastolic threshold of excitation in atria, but not ventricles.32 ISQ-1 may also block INa, since this agent slows down conduction velocity in atria in vivo.39 AVE0118 prolongs ERP but not APD90 and reduces VMax in canine coronary-perfused atrial preparations (Burashnikov et al, unpublished). Note that with the exception of AZD7009 (see above), comparison of the effects of IKur blockers on INa or sodium channel-dependent parameters in atria and ventricles has not been conducted.
Figure 2. Ranolazine specifically induces prolongation of the effective refractory period (ERP) and development of post-repolarization refractoriness in atria
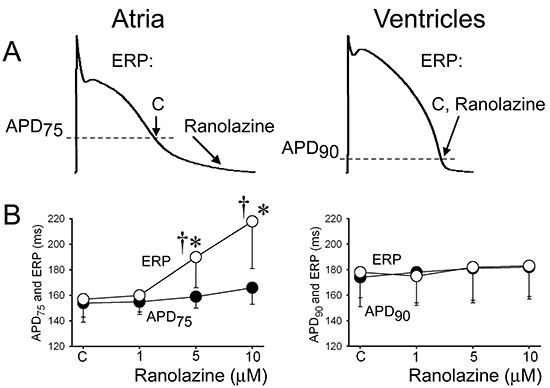
(PRR, the difference between ERP and APD75 in atria and between ERP and APD90 in ventricles; ERP corresponds to APD75 in atria and APD90 in ventricles). CL = 500 ms. C – control. The arrows in panel A illustrate the position on the action potential corresponding to the end of the ERP in atria and ventricles and the effect of ranolazine to shift the end of the ERP in atria but not ventricles. * p<0.05 vs. control. † = p<0.05 vs. APD75 values in atria and APD90 in ventricles; (n=5-18). From Burashnikov et al5 with permission.
IKur blockers that have been shown to be experimentally and clinically effective in terminating AF (i.e., AZD7009 and vernakalant) have also proven to exert potent block of INa and IKr.37,38 It is not clear whether IKur or INa plays the greater role in producing atrial-selective prolongation of ERP and suppression of AF. Perhaps the most-investigated IKur blocker, AVE0118, suppresses AF in goats and pigs, but at concentrations that inhibit Ito and IK-ACh.27,40 Another IKur blocker ISQ-1 can terminate AF in in vivo dogs at the concentrations that block IKr and possibly INa, since conduction time is significantly increased in atria.39 Low concentrations of 4-AP (10-50 µM, which selectively inhibit IKur) do not prevent the initiation of AF or terminate persistent ACh-mediated AF in canine coronary-perfused atrial preparations.25
Thus, available experimental and clinical data suggest that “pure” IKur inhibition alone is incapable of effectively suppressing AF and that the antiarrhythmic effects of most IKur blockers under development are attributable to associated inhibition of other ion channels including INa, Ito, and/or IKr). The relative contribution of IKur reduction is not clear at this time.
Atrial Predominant Antiarrhythmic
Approaches for AF
We refer to atrial selective or predominant targets as to those that are present in both chambers of the heart, but inhibition of these targets produces greater effects in atria vs. ventricles. “Atrial-predominant” refers to a lesser degree of atrial selectivity. The results of recent experimental studies indicate that some INa blockers (such as ranolazine and chronic amiodarone) depress sodium channel-dependent parameters in an atrial selective or predominant manner.5,35,36 While not well appreciated, IKr blockers are also atrial-predominant in that they preferentially prolong atrial repolarization at normal heart rates.7-13
Atrial Predominant Effects of IKr Block on Cardiac Repolarization
In direct comparisons, selective IKr blockers such as E-4031, sotalol, d-sotalol, dl-sotalol, dofetilide, WAY-123,398, ibutilide, MK499, and almokalant preferentially prolong atrial vs. ventricular ERP and APD at normal pacing rates.7-13 At slow pacing/heart rates, however, ventricles, but not atria commonly develop exaggerated APD prolongation, early afterdepolarizations, and Torsade de Pointes in response to a reduction of IKr.41,42
Does Ito Block Preferentially Alter Atrial vs. Ventricular Repolarization?
The IC50 of 4-AP’s action to block atrial Ito is one third of that of ventricular Ito in human and canine myocytes.43,44 If this proves to be the case with other Ito blockers, then Ito block might be expected to produce a greater effect on atrial vs. ventricular repolarization. Because most IKur blockers also reduced Ito, inhibition of Ito may contribute to the atrial-selectivity of IKur blockers, both with respect to their antiarrhythmic and proarrhythmic actions.
Atrial Predominant Sodium Channel Block
In recent studies, we examined atrioventricular differences of the effects of ranolazine, chronic amiodarone, lidocaine and propafenone on sodium channel-dependent parameters, such as the maximum rate of rise of the action potential upstroke (Vmax), diastolic threshold of excitation (DTE), conduction velocity (CV), and PRR.5,35,36,45 Using canine isolated coronary-perfused atrial and ventricular preparations, we evaluated therapeutically-relevant concentrations of these agents. Ranolazine, a recently marketed antianginal agent, was found to depress Vmax, DTE, CV, and induce PRR exclusively or predominantly in atrial preparations.5 Thus, when studied in beating multicellular preparations, ranolazine proved to be an atrial-selective/predominant sodium channel blocker (“an atrial selective Class I agent”).
Chronic amiodarone was found to depress sodium-channel dependent parameters in both atrial and ventricular preparations, but much more effectively in atria.35,36 Lidocaine was also atrial-predominant, but far less atrial-selective than ranolazine or amiodarone.5 Propafenone showed no chamber selectivity for INa block at a normal pacing rate (CL = 500 ms), but some atrial predominance at rapid pacing rates, likely due to atrial specific APD prolongation (see later).45 As previously mentioned, AZD7009 also behaves as an atrial-selective INa blocker.32
Ranolazine, propafenone, and chronic amiodarone all produce prolongation of APD90 in the canine atria, likely to due to their actions to inhibit IKr. This effect of these agents potentiate their effects to reduce INa and depress INa-dependent parameters, thus contributing to their atrial-selective effects, particularly at rapid activation rates (Fig. 3C).
Figure 3. Ranolazine produces a much greater rate-dependent inhibition of the maximal action potential upstroke velocity (Vmax) in atria than in ventricles
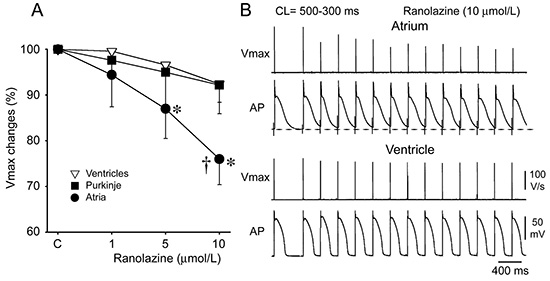
A: Normalized changes in Vmax of Atrial and ventricular cardiac preparations paced at a cycle length (CL) of 500 ms. C: Ranolazine prolongs late repolarization in atria, but not ventricles and acceleration of rate leads to elimination of the diastolic interval (during which the recovery from sodium channel block occurs), resulting in a more positive take-off potential in atrium and contributing to Atrial selectivity of ranolazine. The diastolic interval remains relatively long in ventricles. * p<0.05 vs. control. † p<0.0 vs. respective values of M cell and Purkinje (n=7- 21). From Burashnikov et al5 with permission.
The atrial-selective action of these agents is thought to be due to important distinctions in action potential characteristics as well as biophysical properties of sodium channels of atrial and ventricular myocytes. The half inactivation voltage (V0.5) in canine atrial myocytes is 12-16 mV more negative than that of ventricular myocytes and resting membrane potential (RMP) in atria is less negative than ventricles (approx. – 83 vs. -87 mV).5,46 These factors indicate that there is a larger fraction of inactivated sodium channels at RMP in atria vs. ventricles and a smaller fraction of resting sodium channels at RMP in atria vs. ventricles. This is expected to slow the unbinding of the drug and recovery of the sodium channel from pharmacologic block in atria, since this recovery occurs principally during the resting state.47
Anti-AF Potential of Atrial Selective vs. Conventional Agents
We compared the effectiveness of therapeutically-relevant concentrations of ranolazine, propafenone, and lidocaine in suppressing and preventing the re-induction of AF in isolated canine coronary-perfused right atrial preparations.5,35,45 The effectiveness of chronic amiodarone in preventing induction of AF was examined as well. Ranolazine prevented the initiation acetylcholine-mediated AF, terminated persistent AF, and prevented its re-induction in coronary-perfused atrial preparations (Fig. 6).5 This anti-AF efficacy of ranolazine (10 μM) was greater than that of lidocaine (21 μM) and similar to that of propafenone (1.5 μM). In atria isolated from chronic amiodarone-treated dogs (40 mg/Kg for 6 weeks), persistent ACh-mediated AF could be induced only in 1 out of 6 atria (vs. 10/10 atria isolated form untreated controls).35 These antiarrhythmic effects of ranolazine, amiodarone, and propafenone were associatedwith both APD prolongation (in the presence of ACh) and the development a significant PRR, with the duration of the latter being much longer the extent of APD prolongation, suggesting that sodium-channel block plays a more predominant role in the anti-AF actions of these agents.5,35
Ranolazine and propafenone both suppress AF but ranolazine, unlike propafenone, does it without prominent effects on ventricular myocardium. These findings suggest that atrial-selective/predominant sodium channel block, perhaps with additional IKr block, may be a promising new atrial-selective approach for the management of AF.5 Interestingly, all clinically effective anti-AF INa blockers also inhibit IKr. Pure INa blockers, such as lidocaine, are not very effective in suppression of AF in the clinic.
Clinical efficacy has been reported for only three atrial-selective agents: AZD7009, vernakalant (agents that block IKur, INa, and IKr) and ranolazine, which blocks INa and IKr. There is therefore little basis for a comparison of atrial-selective agents with conventional anti-AF agents. In a study that was not designed to test the anti-AF efficacy of ranolazine, this agent was found to reduce the incidence of new onset AF onset by 30% in acute coronary syndrome patients (p=0.08).6 AZD7009 was reported to successfully convert up to 70% of patients with an average AF duration of 43 days to sinus rhythm48 whereas vernakalant was successful in converting 52-56% of patients with recent AF onset (< 7 days) but only 8% of patients with long-duration AF (< 45 days).49 These findings are not very different from those of conventionally used anti-AF agents, such as flecainide, propafenone, dofetilide, amiodarone, ibutilide, etc.50 The benefit of the atrial selective agents is that they do not produce significant electrophysiological changes in the ventricles. It appears that amiodarone can also be categorized as atrial-selective.35 It is noteworthy that direct comparisons of the effects of most clinically-used anti-AF agents in atria and ventricles are not available either in in vivo or in coronary-perfused preparation studies.
Current pharmacologic strategies for the management of AF include sodium channel blockers such as propafenone and flecainide, potassium channel blockers such as sotalol and dofetilide and mixed ion channel blockers such as amiodarone. All have demonstrated efficacy but distinct indications based on their proclivity to promote ventricular arrhythmogenesis under different conditions.50 These adverse effects distinguish these agents from the newer atrial-selective agents. The sodium channel blockers are contraindicated in patients with coronary artery or structural heart disease because of their potent effect on conduction in the ventricles, potassium channel blockers predispose to the development of acquired long QT and Torsade de Pointe arrhythmias because of their potent effect to prolong ventricular repolarization, and mixed ion channel blockers such as amiodarone are associated with multi-organ toxicity.
Atrial Selectivity and Atrial Remodeling
It is important to recognize that the atrial selective/predominant effects of some INa as well as IKr blockers have been tested in relatively “healthy” atria and ventricles.5,7-10,35 35 Clinical AF commonly occurs in conjunction with a number of conditions (congestive heart failure, hypotrophy, dilatation, hypertension, etc) associated with electrical and/or structural remodeling of the atria. These pathophysiologic changes can importantly modify the response to sodium and potassium channel blockers,23,51,52 and thus modify the atrial selectivity of these agents.
There is no robust evidence in support of the hypothesis that “pure” inhibition of IKur may effectively suppress AF. No clinical data are available relative to the anti-AF efficacy and safety of IKACh or Cx40 as atrial-specific approaches. The available data suggest that atrial-selective approaches involving a combination of INa, IKur, IKr, and, perhaps Ito blockade, may be more effective in the management of AF than pure IKur or INa block. The anti-AF efficacy of the atrial-selective/predominant agents appears to be similar to that of conventionally used anti-AF agents, with the major difference being that the latter are associated with ventricular arrhythmogenesis as well as extracardiac toxicity. It is noteworthy, however, that the long-term toxicity of the atrial-selective drugs, with the exception of ranolazine, is not known.
Dr. Antzelevitch consults for CV Therapeutics, AstraZeneca. Dr. Antzelevitch received lecture fees from CV Therapeutics, Cardiome, Solvay, Pfizer, Aventis. Dr. Dr. Antzelevitch received grant support from CV Therapeutics, AstraZeneca, Cardiome, Epix, Solvay, Genzyme