Barriers to Emergency Department Utilization of AFIB Protocol in Uncomplicated Lone AFIB Patients-Results from an Online Survey Study.
Britt T1, Janson JP1, Knisely T1, LaBond VA1
1
Genesys Regional Medical Center One Genesys Parkway Grand Blanc, MI 48439
.
Historically, atrial fibrillation (AFIB) management has focused on rate control and anticoagulation, necessitating hospital admission. Recently, some emergency departments (EDs) have implemented protocols to avoid hospital admission when managing lone AFIB. Despite this recent trend, there is still reluctance toward the implementation of these protocols by some emergency physicians (EPs).
This study investigates barriers to implementation of ED AFIB protocols by surveying which aspects may impede their use.
To analyze the perceived barriers from EPs, we formulated a survey assessing the various components of ED AFIB management to identify which aspects might impede EP utilization. It was distributed as an email to large national ED physician group. Data was analyzed using descriptive means and weighted averages.
Of 185 respondents (response rate 6.1%), 17.4% already had AFIB protocols in place at their home institutions and 82.6% did not. Majority opinion of largest barriers toward the implementation of AFIB protocols were the extended ED length of stay and discharge with unclear follow-up. There was little concern with chemical and electrical cardioversion and very limited concern with rate control and initiating oral anticoagulation. EPs supported placement in Observation for implementation and involvement of discharge planning to establish prescriptions and follow-up.
EP input regarding the development of ED AFib protocols will be essential in order to develop cost effective, convenient and safe methods of treatment. This survey of EP suggests that ED length of stay and insuring close outpatient follow up are key issues to address as protocols are designed.
Key Words : Utilization, Protocol, Cardioversion, Fibrillation, Pharmacology.
Correspondence to: Virginia Ann LaBond MD, MS, FACEP
Genesys Regional Medical Center
One Genesys Parkway
Grand Blanc, MI 48439
Atrial Fibrillation (AFIB) is a common cardiovascular arrhythmia effecting 2.6-6.1 million Americans, and 9% of Americans greater than 65. [1]. In addition to high disease prevalence, AFIB also carries a healthcare burden of 750,000 annual hospital visits and 130,000 annual deaths, costing the US healthcare system roughly six billion dollars per year [1].
AFIB is the most commonly diagnosed arrhythmia in US emergency departments [2,3]. The classical management of atrial fibrillation in the emergency setting consists of either heart rate control with anticoagulation or heart rhythm control with electrical or chemical cardioversion. Traditionally, emergency physicians (EPs) and Advanced Practice Providers (APPs) have opted for the former method, often starting patients on rate controlling and anticoagulant drips, requiring subsequent admission and transition to oral medications. This has resulted in high admission rates for AFIB as well as a significant cost burden to the US healthcare system [4,5].
With the current US health care trends shifting away from hospitalization and toward outpatient management there has been an increased emphasis on ED management of AFIB with subsequent discharge home when possible [5]. This method has been shown to be both safe as well as offering significant cost reduction [6]. One retrospective analysis evaluated 35,255 combined inpatients and outpatients to compare annual costs of management in both settings, and found the average inpatient cost to be $11,307 versus an outpatient cost of $2,827 when AFIB was the primary diagnosis. This cost differential was also present when AFIB was a secondary diagnosis, costing $5181 for inpatient management and $1376 for outpatient management, respectively [7].
In response, hospital emergency departments have been taking steps to create protocols to safely identify candidates of ED treatment and discharge home with further management in the outpatient setting. One such protocol developed by Mansour et al. at Massachusetts General Hospital looked at 382 patients with AFIB over a one year period and was found to greatly reduce admissions (15% admission versus historical 79%) [5]. In the aggressive Ottawa protocol for AFIB, 385 patients with new onset (<48hr) AFIB were retrospectively evaluated after being electrically and chemically cardioverted with 42% and 91% discharge rates, respectively, with no deaths or cerebrovascular accidents [8].
Despite success in discharging these patients, many EPs still opt for inpatient management, posing a significant barrier to changing traditional management practices. These barriers consist of increased length of stay while in the ED, inability to establish appropriate follow up, concern when initiating anticoagulation without clear follow-up, and concern surrounding electrical or chemical cardioversion. To evaluate these barriers, we designed an online survey distributed to various emergency departments throughout the country to evaluate barriers to the implementation of AFIB protocols.
Surveys (online supplement A) were created using an online survey software. Respondents were first asked to identify themselves as residents, attendings, or APPs. Next, they were asked if they had a protocol in place in their home institution. Sample protocols for ED AFIB management were provided for both less than and greater than 48 hours of AFIB onset for reference ([Figure 1] and [Figure 2]). If no protocol was in place in the respondent’s home institution, they were asked to answer questions using the sample protocols.
Six domains of potential concern were identified for ED lone AFIB management: rate control, rhythm control, anticoagulation, feasibility, discharge, and patient satisfaction. The domains were measured by a 5-point Likert scale (Very and Relatively Concerned, Neutral, Very and Relatively Unconcerned). Scoring labels were 1 – 5 and responses were averaged for each domain. The percentage of respondents choosing each level of concern was also independently quantified. In each category, respondents were given the choice of choosing “not applicable”. For those with established AFIB protocols at their home institution, free text boxes were provided where respondents were asked to elaborate and explain how key institutional differences which might invalidate or otherwise compromise the question.
In addition to the above questions relating to AFIB protocols, respondents were asked to rate their support for adjustments to the protocol to increase ED feasibility as it relates to discharge planning, observations management, and consultant evaluation prior to discharge.
Two free text boxes were provided at the end of the survey to offer suggested improvements as well as subjective experiences in using AFIB protocols at their home institutions to glean further qualitative evidence relating to EP AFIB utilization and barriers.
The study was reviewed and approved by the Institutional Review Board (IRB) on August 23, 2017 at the home institution (a community teaching hospital) to ensure informed consent and ethical standards were met in the surveys and study implementation.
The survey was then embedded within a survey link contained within the body of an email describing the study and asking consent to fill out the survey. By completing the survey physicians consented to their participation within the study. The email and survey were distributed to members of a large national ED physician group. The emails were accessed after approval from the group’s clinical governance board. The ED group mailing list encompassed one hundred eighty different emergency departments in twenty-one different states. No personal data was collected.
Results were collected Sept. 25th - Oct. 1st 2017 after the email was distributed and then closed for analysis. Descriptive analysis was used to describe survey results.
Figure 1 AFIB Less Than 48 Hour Protocol.
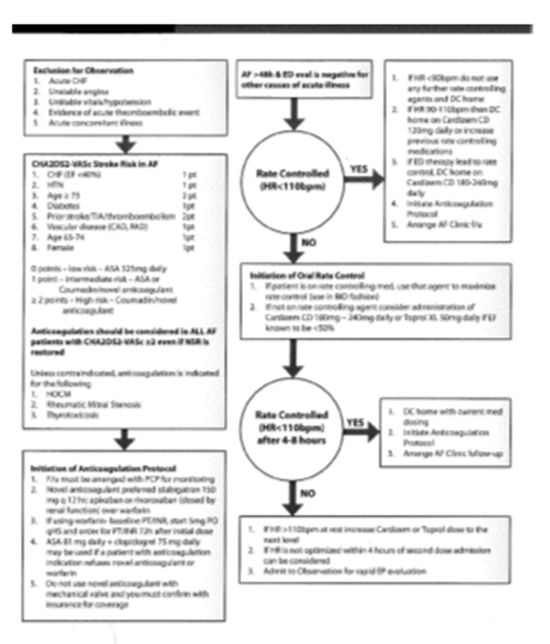
Authors’ home institution protocol provided for respondents’ reference during survey completion.
Figure 2 AFIB Greater Than 48 Hour Protocol
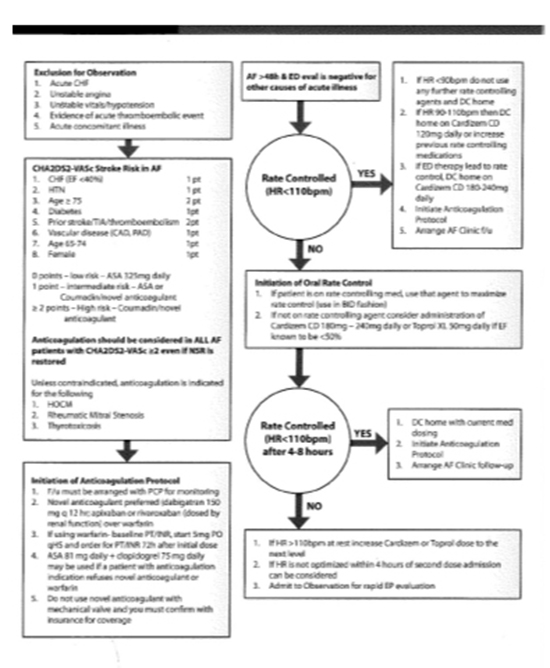
Authors’ home institution protocol provided for respondents’ reference during survey completion.
One-hundred-eighty-five EPs and APPs responded to the survey (6.1% response rate). Only one respondent (0.54%) was a resident, 154 were attendings (81.1%), and 34 APPs (18.2%) made up the group. Of those who responded, 17.4% had an AFIB protocol already in place (“P”- Protocol in place) while 82.6% did not (“NP”-No Protocol in place) and utilized the supplemental protocol to respond to the survey.
Using the weighted averages (from one to five) as an estimate of concern level regarding different aspects of AFIB protocols, the strongest levels of concern were regarding increased ED length of stay, extended ED length of stay while attempting protocol, lack of comfort discharging someone on flecainide or other oral anti-arrhythmic, and no clear way of establishing follow-up. Data is presented in [Figure 3] and [Figure 4].
Within the protocol group, there was a relative concern for initiating oral anticoagulation while there was less concern of this in the no protocol group. Both protocol and no protocol groups had relatively low concern for oral anticoagulants for stroke prevention and for time consumption for anticoagulant insurance availability.
With regards to rhythm control, both groups were both relatively unconcerned when it came to rhythm control methods in the emergency department whether it be by chemical cardioversion or electrical cardioversion however there was more concern overall about discharging patients home on flecainide, as mentioned above.
In line with a concern for lack of follow-up for those patients who are discharged home, respondents were likely to see Cardiology/electrophysiology consultation in the ED prior to discharge as reassuring. Both groups also endorsed the ideas of placement in observation and/or discharge planning to establish follow-up and medication prescription prior to discharge.
A sub-group analysis of the greatest area of concern, ED length of stay, was performed comparing attending physicians to APPs. Attendings demonstrated a weighted average of 3.76 and 4.04 (no protocol, protocol). The group demonstrating the greatest area of concern were APPs who had a protocol at their facility with a weighted average of 4.4. APPs with no protocol were about equal to their attending counterparts (3.81).
Select comments offered regarding respondent opinions and experience are included in [Table 1].
Figure 3 Support of Suggested improvements to AFIB Protocol
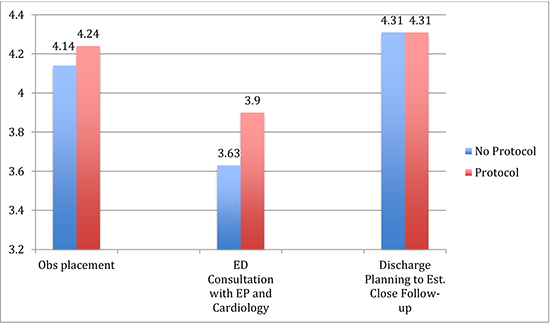
Figure 4 Selected Barriers to Implementation of AFIB Protocol
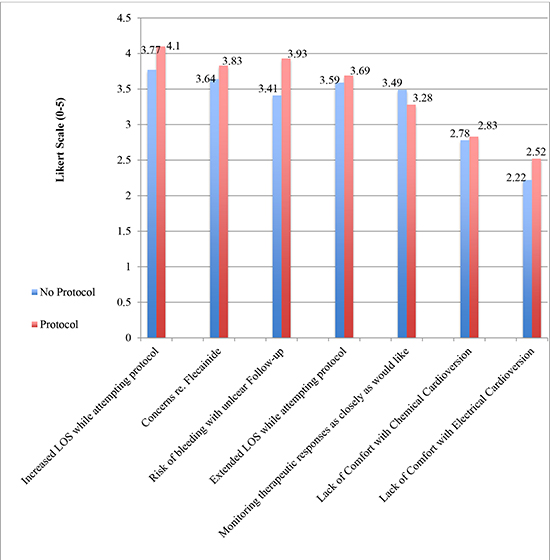
Table 1. Free text comments offered by respondents. Organized by potential barriers
| If you have used protocol in the ED:
• Impossible to prescribed new oral anticoagulants due to insurance problems.
• I found this worked well, when I worked at a hospital with this protocol in place. My only issue was that it was much faster to sedate and electrically cardiovert the patient than waiting for pharmacy to send the antidysrhythmic medication, then wait for a response.
|
| Extended ED length of stay while attempting protocol:
• The protocol takes way too long to read, it's too much in an ED situation.
• We have not routinely utilized our similar protocol as it is burdensome for the ED with a long LOS.
|
| Lack of comfort with electrical cardioversion:
• DC cardioversion not permitted in ED by ED MD. Done by cardiology when admitted.
|
| Lack of comfort on discharging patient on flecainide or other oral antiarrhythmic:
• Not comfortable discharging with flecainide,etc . |
| Increased ED length of stay:
• Time in ED if PO flecanide and then 4 hours wait/watch. |
| No clear way to ensure ok follow up:
• We have specific A-Fib F/U with cardiology.
• We can obtain this.
• Our system can talk with cardiology 24/7 to arrange f/u and/or send electronic messaging to cardiology clinic, however sometimes uninsured cause an issue.
|
| Any adjustments or improvements you would make to your protocol:
• It's not feasible to have specialist come to the ED for every new onset afib patient. the wait time is too long.
• I the above stated protocol should be implemented in an observation unit. However, pts that are virtually asymptomatic, relatively rate controlled (with minimal intervention; such as 1 or 2 IV dose of Cardizem) and have closed loop follow up can easily be discharged. All others should be admitted for obs as likely do not know EF or CAD status at time.
• Discharge after discussion with EP or A fib clinic Physician. |
| If you have used the protocol in your ED:
• I discharged someone with new onset Afib with RVR almost weekly with no known bad outcomes.
• Similar to the above and works well.
• EP follow up unreliable.
• Is cardiology dependent- Patients that I feel comfortable to be DC they want in the hospital.
• Time consuming.
• Two patients with poor outcomes with protocol / Flecainide.
|
AFIB is a common cardiac arrhythmia that poses a significant healthcare burden in the US. There are multiple barriers surrounding the implementation of protocols emphasizing patient discharge from the ED. Our results indicate that among emergency physicians with AFIB protocols in place there is a relative concern surrounding the lack of clear follow-up after discharge as well the time and attention necessary to implement these protocols in busy ED settings.
It is not surprising that EPs and APPs were found to be relatively unconcerned with chemical and electrical cardioversion as these are common practice in EDs for many cardiovascular diseases. Similarly, the use of AV nodal blocking agents and initiation of anticoagulation has been the mainstay of ED AFIB treatment in the past. While often administered in IV formulations and followed by admission to telemetry units, EPs and APPs are familiar with the mechanism of action and adverse reactions of AV nodal blockers and comfortable with their administration and prescription following discharge. Similarly, the initiation of the so called Noval Oral Anticoagulants (NOVACs) in both DVT management as well as AFIB is now common practice in the ED and there is a relative lack of concern surrounding their prescription and discharge.
With regards to initiation of rate control, the majority of concern centers around the time needed to achieve rate control rather than discomfort with placing the patient on a new AV nodal blocking agent prior to discharge. This is consistent with the overall lack of comfort with an increased ED length of stay also demonstrated in the survey. There were six comments re-emphasizing the time-consuming nature of this protocol feature. One respondent stated that their home institution abandoned their AFIB protocol altogether due to the time burden associated with the protocol.
Given these barriers, emergency physicians supported two major areas of adjustment to AFIB protocols: after initiation of the protocol in the ED, placement of patients in observation for the remaining steps to relieve the time burden of frequent re-evaluation and intervention. When observation is unavailable, ED consultation with cardiology/electrophysiology in combination with discharge planning to establish close follow-up was largely supported by respondents. This latter option fails to alleviate the concern surrounding the time burden in the ED but may have the benefit of facilitating discharge and avoiding unnecessary admission with IV drips and long hospital stays.
Notably, there was an overall lack of support for adjusting protocols to include EP and Cardiology evaluation of patients in person while in the ED prior to discharge. Three comments were made on this point, two suggesting telephone conversation or direct messaging to “close the loop” and one stating that routine AFIB cases should be discharged from the ED with concern for over utilizing these consultants in Routine AFIB cases. On the whole, respondents favored discussion with Cardiology/electrophysiology but it seems they did not feel the need for ED evaluation in person by these consultants.
Current US healthcare trends are going away from admission where possible and appropriate. In addition, there is increasing emphasis on emergency departments to meet metrics regarding ED length of stay, door to doc time, and boarding time, among others. There is significant pressure on EPs and APPs to both see patients quickly, facilitate turnover in emergency department beds, and discharge where appropriate and possible. The sample protocol provided at longest would take six hours (<48 hour onset) or eight hours (>48 hours). With many EDs having door to discharge goals of four hours (and often less), AFIB protocols can pose a significant hurdle to meeting these ED metrics. To this end, it is not surprising that EPs have concern surrounding the time needed to implement such protocols.
When taken together with our data, it seems that EPs and APPs are relatively comfortable managing the medical side of AFIB but remain concerned with their ability to do so in a time sensitive manner while optimizing emergency department patient flow. Although APPs with a protocol in place did show the highest level of concern regarding increased length of stay, our subgroup analysis demonstrated minimal difference in the comfort levels of EPs versus APPs.
Based upon our results, we suggest two possible solutions to ED AFIB protocols to alleviate concerns and improve utilization. If present, cardiac observation or clinical decision units can be utilized for stable lone AFIB patients. Treatment can be rapidly initiated in the ED with subsequent placement of patients in observation under the supervision of healthcare providers who are able to reassess, intervene, establish follow-up, and discharge patients without compromising ED metrics or necessitating frequent re-evaluation and intervention from emergency physicians.
In institutions where this is not feasible, consultation with cardiology/electrophysiology in conjunction with discharge planning to establish medication regimens and close follow-up may be useful adjuvants in the discharge of AFIB patients.
This study did face limitations with regards to the sample pool. The respondent pool takes into account EPs and APPs across 22 states, most of which are clustered in the midwest, mountain west, northeast, and southeast and are not symmetrically distributed between these regions. For this reason, regional differences may not be reflected in the survey.
While 185 respondents participated in the survey, this number reflects a small proportion (roughly 0.5%) of the total estimated pool of potential respondents and for this reason may not be an accurate reflection of the total group of physicians and APPs. While there were over 180 sites the survey was sent out to, there was no way of knowing exactly which respondents came from which sites and significant geographical variations may have been missed. A study with a larger sample size from a multitude of different groups and regions would need to be performed to eliminate these areas of potential sampling bias.
Despite efforts of many hospitals toward the implementation of outpatient driven protocols, emergency physicians in this study reported reluctance toward implementation of these protocols due to increased emergency department length of stay, the need for close and frequent observation, and lack of follow-up with specialists. While these protocols may be effective in decreasing hospital admissions, hospital length of stay, and financial burden to the patient, EP utilization of such protocols are impeded by the ability to implement the frequent re-evaluations and interventions in crowded emergency departments. These results beg the question of implementing such protocols in cardiac observation units or similar which would obviate the need for frequent patient re-evaluation and serve to free-up emergency department beds. Alternatively, EPs are in favor of closed loop communication with cardiology and/or electrophysiology in conjunction with discharge planning for close follow-up as a suitable alternative in lieu of observation and clinical decision units.
EP input regarding the development of ED AFib protocols will be essential in order to develop cost effective, convenient and safe methods of treatment. This survey of EP and APP opinion on the topic suggests that ED length of stay and insuring close outpatient follow up are key issues to address as protocols are designed.