Value of Interatrial Block for the Prediction of Silent Ischemic Brain Lesions
Göksel Çinier1, Ahmet İlker Tekkeşin1, Tuğba Yanar Çelik2, Özlem Mercan2, Halil İbrahim Tanboğa3, Muhammed Burak Günay1, Ceyhan Türkkan1, Mert İlker Hayıroğlu4, Bryce Alexander4, Ahmet Taha Alper1, Adrian Baranchuk5
1
Dr. Siyami Ersek Thoracic and Cardiovascular Surgery Research and Training Hospital, Department of Cardiology, Kadikoy, Istanbul, Turkey.2
HaydarpasaNumuneEgitimveArastırmaHastanesi, Department of Neurology, Kadikoy, Istanbul, Turkey.3
Hisar Intercontinental Hospital, Department of Cardiology, Umraniye, Istanbul, Turkey.4
Haydarpaşa Sultan Abdulhamit Han EğitimveAraştırmaHastanesi, Department of Cardiology, Kadikoy, Istanbul, Turkey.5
Kingston General Hospital, Department of Cardiology, Queen’s University, ON, Canada.
Previous studies demonstrated that interatrial block (IAB) is associated with atrial fibrillation (AF) in different clinical scenarios. The aim of our study was to determine whether IAB could predict silent ischemic brain lesions (sIBL), detected by magnetic resonance imaging (MRI).
Patients presented to a neurology clinic with transient ischemic attack (TIA) symptoms and underwent brain MRI were included to the study. sIBL were defined as lesions without corresponding clinical symptoms regarding lesion localization evaluated by two neurologists. A 12-lead surface ECG was obtained from each patient. IAB was defined as P-wave duration > 120 ms with (advanced IAB) or without (partial IAB) biphasic morphology in the inferior leads.
sIBL was detected in 61 (49.6%) patients. Patients with sIBL were older (P<0.001), had more left ventricular hypertrophy (LVH) (P=0.02) and higher CHA2DS2-VASc score compared to those without (P<0.001). P-wave duration was significantly longer in patients with sIBL (124 [110.5 – 129] msvs 107 [102 – 116.3] ms) (P<0.001). IAB was diagnosed in 36 patients (59%) with sIBL (+) and in 11 patients (18%) with sIBL (-); p<0.001. Multivariate logistic regression analysis identified age [Odds ratio (OR), 1.061; 95% confidence interval (CI), 1.012 - 1.113; p=0.014], CHA2DS2-VASc score (OR, 1.758; 95% CI, 1.045 - 2.956; p=0.034), LVH (OR, 3.062; 95% CI, 1.161 - 8.076; p=0.024) and IAB (including both partial and advanced) (OR, 5.959; 95% CI, 2.269 - 15.653; p<0.001) as independent predictors of sIBL.
IAB is a strong predictor of sIBL and can be easily diagnosed by performing surface 12-lead ECG.
Key Words : Interatrial Block, Atrial Fibrillation, Silentischemic Stroke.
Correspondence to: Göksel Çinier,
Dr. Siyami Ersek thoracic and cardiovascular surgery
research and training hospital, department of cardiology,
Selimiyemahallesi, Tıbbiyecaddesi, No: 13, 34668,
Uskudar, Istanbul, Turkey
Interatrial block (IAB) refers to a conduction delay or block between the right and left atrium and is manifested as P-wave duration greater than 120 ms[1]
. Multiple studies have demonstrated the association of IAB with atrial fibrillation (AF) and ischemic stroke in many different clinical scenarios[2-10]. Fibrosis of the atrial conduction system, mainly in the Bachmann region, contributes to the alteration in structural and electrical properties of atrial myocytes and development of IAB. Magnetic resonance imaging (MRI) allowsfor detection of both symptomatic and silent ischemic brain lesion (sIBL) with high accuracy. SIBL is encountered with high prevalence following short pulmonary vein isolation[11], transcutaneous aortic valve replacement[12] and carotid stent implantation procedures[13]. Although its clinical significance is still being debated, several studies have demonstrated sIBLis a predictor of future ischemic stroke, decline in cognitive function and depression [14].
In this study, we evaluated the predictive value of IAB for sIBL detected by MRI.
The study population consisted of patients who presented to a neurology clinic with transient ischemic attack (TIA)symptoms and had a brain MRI.SIBL was defined as lesionspresent on radiological assessment that did not correspondto clinical symptoms according to lesion localization. If symptoms did correspond withradiographic lesion localization, the patient was determined to have a symptomatic infarct and was excluded from the study. Patients underwent ECG, TTE and carotid Doppler examination as a routine evaluation for possible source of their clinical symptoms.Exclusion criteria were; 1) presence of non-sinus rhythm on ECG, 2) presence of any lesion on brain MRI corresponding to their clinical symptoms,3) history of ischemic or hemorrhagic stroke or TIA, 4) history of atrial tachyarrhythmia, 5) valvular heart disease, valvuloplasty or valve replacement procedure and 6) detection of carotid artery disease during carotid artery doppler examination.All patients participating in the study provided informed written consent. The study was approved by the institutional ethics committee.
Baseline patients’ characteristics and medical history were recorded. A standard 12-lead electrocardiogram (ECG) (Schiller, CardioVit, AT-10 plus) (Filter 150 Hz, 25 mm/s, 10 mm/mV) was obtained for all study patients. ECG’s were scanned at 300 DPI and images were amplified 10x. The P-wave onset was defined as the point of initial upward or downward deflection from the baseline and the offset as the return of the waveform to the initial baseline.The interval between the onset and the offset of P wave in the frontal leads were measured by using Iconico semiautomatic calipers [Figure 1].Two measurements were made in each ECG and if the P wave onset and offset were not determined easily, up to four measurements were made. All ECG analyses were performed by an observer blinded to the clinical data of patients, and in case of any doubt, second expert opinion was consulted.Partial and advanced IAB were classified as recommended in the international consensus report(1):1) Partial IAB: P-wave duration ≥120 ms without negative final component in the inferior leads; 2) Advanced IAB: P-wave duration ≥120 ms with biphasic (±) morphology in the inferior leads.
Figure 1. An example of advanced interatrial block (a-IAB) (P-wave duration ≥120 ms with biphasic (±) morphology).
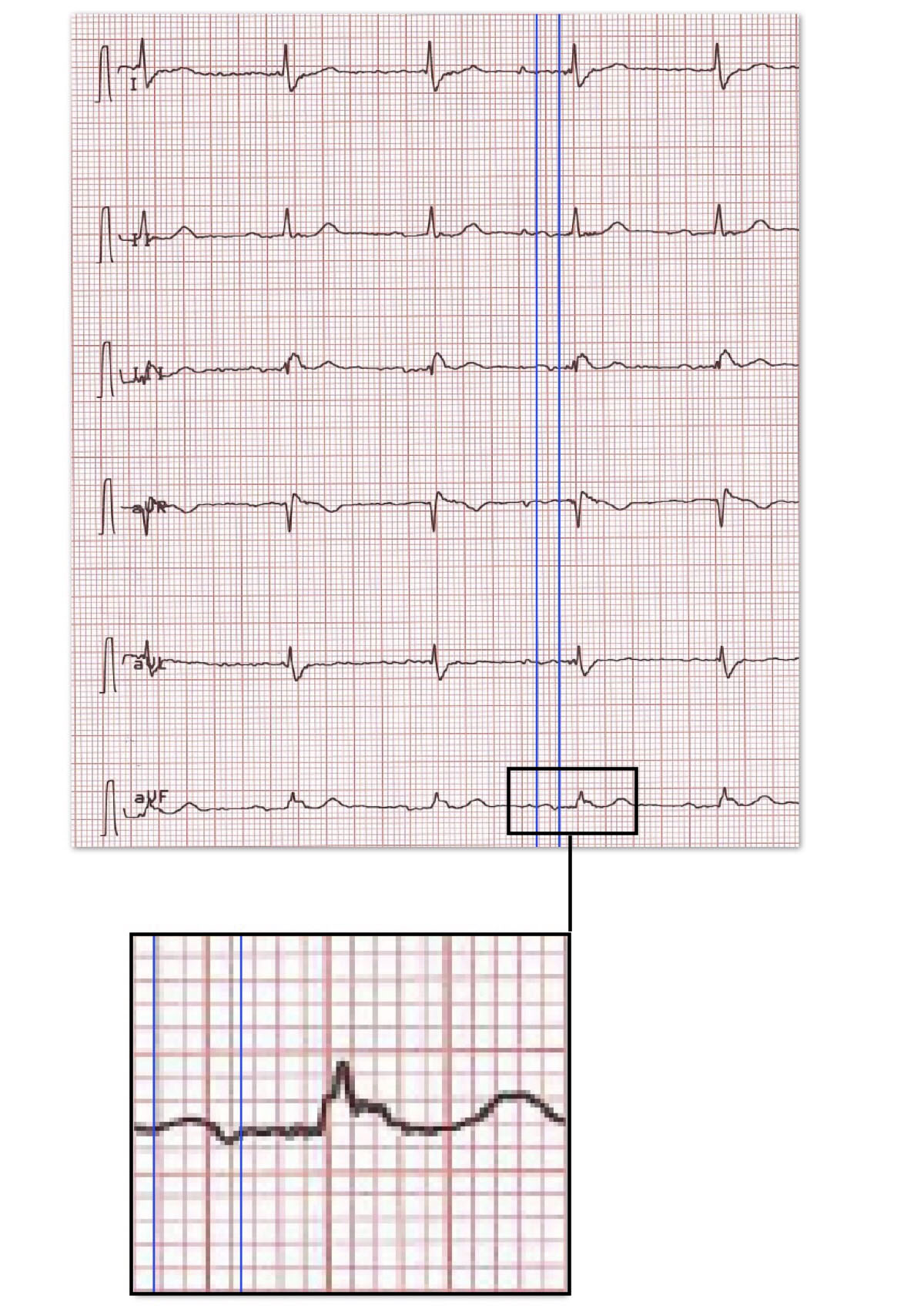
All patients underwent 2-dimensional transthoracic echocardiography (TTE) (Vivid 7, GE healthcare; Horten, Norway) evaluation by an expert on cardiovascular imaging.M-Mode and 2D measurements were performed in accordance withthe current guidelines on chamber quantification from the American Society ofEchocardiography[15].
Patients were routinely screened for AF in a clinical visit at 12 months. 12- lead surface ECG was performed on each patient. In addition, our hospital’s electronic database was searched for any 12-lead ECG and 24-h Holter monitoring records that detected AF in patients within 12 months.
Brain MRI scans wereperformed using 1.5 Tesla MRI scanners (MagnetomAvento, Siemens Healthcare, Erlangen, Germany). The imaging protocol includeddiffusion-weighted imaging (DWI) sequence and T2-weighted fluid-attenuated inversion recovery (FLAIR) sequence.For each DWI sequence, the apparent diffusion coefficient (ADC) map was obtained by using appropriate software. sIBL weredefined as hyperintensity on DWI sequence with corresponding hypointensity and hyperintensity on ADC map and FLAIR sequence respectively. Each individual sIBL was recorded independently of size. All MRI images were analyzed by a radiologist blinded to all other clinical data.
All data were evaluated using IBM SPSS 22 (IBM, SPSS, USA). Mean and standard deviations were used for quantitative variables. Student T test was used for normally distributed variables in both groups and Mann-Whitney U test was used for variables which were not normally distributed. Qualitative variables were evaluated by Pearson chi-square and continuity (Yates) correction. Logistic regression analysis was used for multivariate analysis to identify risk factors for the presence of sIBL. A P value of <0.05 was accepted as statistically significant.
During the period from November 2016 through June 2017, 318patientsunderwent brain MRI in neurology clinic due to TIA symptoms. 108 patients were excluded from the study due to presence of MRI findings corresponding to their clinical symptoms. 29patients were in AF, 32 patients had prior history of ischemic or hemorrhagic stroke, 9 patients had valvular heart disease, prior valve replacement or valvuloplasty procedure,10 patients had carotid artery disease detected during Doppler examination. These patients were excluded from the study. In addition, 7 patients were excluded from the study due to a conflict on their radiological and clinical data. A total of 123 patients constituted the final study population.
Patients were divided into two groups with respect to the presence of sIBL in brain MRI. sIBL was detected in 61 (49.6%) patients. Baseline demographic and clinical characteristics of each study group are depicted in [Table 1]. Presence of IAB, including both partial and advanced IAB, was significantly higher in patients with sIBL [36 patients (59%) vs 11 patients (18%), p<0.001]. The prevalence of advanced IAB was comparable between the two groups [5 patients (8%) vs 2 patients (3%), P=NS]. Patients with sIBL were more likely to have LVH compared to those without sIBL [29 patients (48%) vs 17 patients (27%), p=0.02].
Table 1. Baseline and clinical characteristics for study patients with sIBL (+) and sIBL (-).
| Baseline characteristics |
Group sIBL (+)
(n = 61)
|
Group sIBL (-)
(n = 62)
|
P value |
| Age (years) |
68 [58.5 – 74.5] |
55 [45 – 62.3] |
> 0.001 |
| Gender (male)(%) |
19 (31) |
25 (40) |
0.289 |
| BMI (kg/m2) |
27.8 [25.4 – 29.4] |
27.9 [24.2 – 30.2] |
0.929 |
| Hypertension (n) (%) |
32 (53) |
30 (48) |
0.652 |
| Diabetes Mellitus (n) (%)
|
25 (41) |
23 (37) |
0.659 |
| Hyperlipidemia (n) (%) |
11 (18) |
13 (21) |
0.681 |
| Heart Failure (n) (%) |
7 (12) |
6 (10) |
0.746 |
| CKD (n) (%) |
7 (12) |
6 (10) |
0.746 |
| CAD (n) (%) |
3 (5) |
3 (5) |
0.984 |
| OSAS (n) (%) |
6 (10) |
7 (11) |
0.793 |
| Smoking (n) (%) |
13 (21) |
10 (16) |
0.461 |
| Hyperthyroidism (n) (%) |
2 (3) |
2 (3) |
0.661 |
| Hypothyroidism (n) (%) |
1 (2) |
3 (5) |
0.317 |
| CHA2DS-VASC |
2 [2 – 4] |
1 [1 – 2] |
> 0.001 |
| Beta-Blocker (n) (%) |
8 (13) |
6 (10) |
0.548 |
| ASA (n) (%) |
21 (34) |
13 (21) |
0.095 |
| P2Y12 inhibitor (n) (%) |
3 (5) |
3 (5) |
0.984 |
| Statin (n) (%) |
6 (10) |
1 (2) |
0.049 |
| ACEI/ARB (n) (%) |
25 (41) |
19 (31) |
0,232 |
| EF (%) |
60 [55 – 60] |
60 [55 – 60] |
0.816 |
| LVH (n) (%) |
29 (48) |
17 (27) |
0.020 |
| LA-AP diameter (mm) |
37 [35 – 41] |
39 [35 – 41] |
0.400 |
| P wave duration (ms) |
124 [110.5 – 129] |
107 [102 – 116.3] |
> 0.001 |
| Partial IAB (n) (%) |
31 (51) |
9 (14) |
> 0.001 |
| Advanced IAB (n) (%) |
5 (8) |
2 (3) |
0.234 |
| Total IAB (n) (%) |
36 (59) |
11 (18) |
> 0.001 |
ACEI: Angiotensin converting enzyme inhibitor, ARB: Angiotensin receptor blocker, ASA: Acetylsalicylic acid, BMI: Body mass index, CAD: Coronary artery disease, CKD: Chronic kidney disease, EF: Ejection fraction, IAB: Interatrial block, LA-AP: left atrial antero-posterior, LVH: Left ventricular hypertrophy, OSAS: Obstructive sleep apnea syndrome, sIBL: Silent ischemic brain lesion.
During 12 months of follow-up, 12 (9.8%) patients developed new-onset AF. Among those 7 and 6 were in the sIBL (+) and sIBL (-) group respectively.
Multiple logistic regression analysis demonstrated that age [Odds ratio (OR), 1.061; 95% confidence interval (CI), 1.012 - 1.113; p=0.014], CHA2DS2-VASc score (OR, 1.758; 95% CI, 1.045 - 2.956; p=0.034), LVH (OR, 3.062; 95% CI, 1.161 - 8.076; p=0.024) and the presence of IAB (including both partial and advanced) (OR, 5.959; 95% CI, 2.269 - 15.653; p<0.001) were independent predictors of sIBL in the overall population[Table 2].
Table 2. Prediction of sIBL by using multiple logistic regression analysis.
|
OR
|
CI 95 % |
P value |
| Age |
1.061 |
1.012 - 1.113 |
0.014 |
| Gender |
1.025 |
0.352 - 2.987 |
0.964 |
| CHA2DS2-VASc |
1.758 |
1.045 - 2.956 |
0.034 |
| LVH |
3.062 |
1.161 - 8.076 |
0.024 |
| t-IAB
|
5.959 |
2.269 - 15.653 |
> 0.001 |
LVH: Left ventricular hypertrophy, sIBL: Silent ischemic brain lesion, t-IAB: Total interatrial block
The major finding of this case-control study is that IAB is significantly associated with the incidence of sIBL detected during MRI examination in patients presented with TIA symptoms. IAB was present in almost 60% of patients with sIBL. The other findings include that patients with sIBL were older, more likely to use statins, had greater incidence of LVH and higher CHA2DS2-VASc score as compared to patients without sIBL.
Other studies have looked at the prevalence of IAB in patients with neurological conditions.O’Neal et al. identified IAB as a risk factor for ischemic stroke (10). Their findings were derived from the Atherosclerosis Risk in Communities Study of 14,716 adults with digital ECGs measured at baseline and then followed for more than 20 years for incident ischemic stroke events. Incidence of ischemic stroke was more than two-fold in patients with advanced IAB as compared to those without. After adjustment for traditional risk factors, advanced IAB continued to remain a significant risk factor for ischemic stroke. An interesting finding from that study was that advanced IAB is a risk factor for ischemic stroke independent from symptomatic AF. Similarly, Ariyarajah et al. investigated the frequency of IAB in patients with sinus rhythm hospitalized for stroke[16]. The prevalence of IAB in this cohort was 61% and LA thrombi were present in 15% of patients with IAB as compared to none in those without. In the present study we found that IAB was present in 59% of patients with sIBL. Our result was consistent with the previous studies showing that IAB was highly prevalent in ischemic stroke.
In the current study, it is reasonable to speculate that IAB not only associated with symptomatic stroke but also asymptomatic episodes. The pathophysiologic relationship between IAB and stroke is unclear [Figure 2]. Patients with a-IAB have deteriorated atrial hemodynamics as shown by reduced atrial stroke volume and kinetic energy[17]. The resultant dysfunctional atria may cause increased risk of stroke. IAB causes atrial electrical remodeling by modifying atrial refractory periods leading to atrial premature beats (APB). It is reasonable to consider IAB as the necessary substrate for APB leading to ischemic stroke given the recent evidence that frequent APB is associated with stroke[18].In addition, IAB predisposes to the occurrence of subclinical AF episodes which is shown to be associated with ischemic stroke[19].
Figure 2. : Pathophysiologic relationship between advanced interatrial block (a-IAB) with atrial fibrillation(AF) and ischemic stroke.
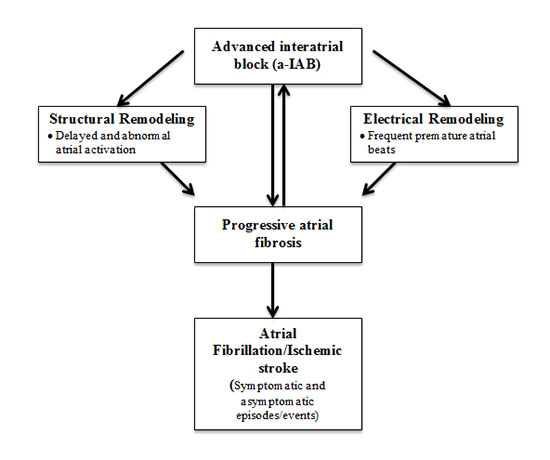
sIBL are frequently encountered in patients with AF [120].Gaita et al. evaluated 180 patients with AF and compared the prevalence of sIBL with 90 patients in sinus rhythm[21].On multivariate analysis the presence of AF was strongly associated with the presence of sIBL (OR: 7.2; 95% CI: 2.3 to 22.3; p = 0.001). In addition, patients with AF had worse performance on cognitive function assessed by neuropsychological test as compared to those in sinus rhythm.Recent studies identified sIBL as a significant risk factor for future symptomatic ischemic stroke, memory impairment and cognitive decline. Vermeer et al. studied an elderly population from The Rotterdam Scan Study and concluded that elderly patients with sIBL had three-fold increased risk of ischemic stroke compared to those without sIBL[22]. Patients with sIBL had comparable risk of ischemic stroke within 4 years with those who were diagnosed with a TIA.According to these data, we would argue that sIBL could be the harbinger of future ischemic stroke and cognitive decline in AF patients.
The direct link between the ischemic stroke and AF was recently challenged by the absence of temporal relationship between stroke events and AF episodes[23]. The emerging concept of fibrotic atrial myopathy as the major cause of stroke necessitates appropriate tools to detect atrial fibrosis. Many researchers now consider AF not as the cause of stroke but rather a risk factor of it. It is reasonable to perform cardiac MRI and novel echocardiographic techniques but, in their absence, presence of IAB on 12-lead ECG is a reliable and non-invasive method to predict atrial fibrosis particularly for given the evidence that extensive atrial fibrosis assessed by late gadolinium enhancement cardiac MRI was associated with a-IAB[24]. Future studies are needed to clarify the beneficial effect of starting anticoagulation in patients with sinus rhythm with additional risk factors for ischemic stroke including a-IAB.
Age and hypertension are the most widely accepted risk factors for sIBL[25]. Similarly, our data indicates that older patient were more likely to have sIBL. Although prevalence of hypertension was comparable between the two groups, LVH which is an echocardiographic predictor of uncontrolled hypertension was significantly more common in patients with sIBL. A possible explanation for this is the high percentage of patients with undiagnosed hypertension. In our data, patients with higher CHA2DS2-VASc were associated to the presence of sIBL. This finding is consistent with results of previous studies that identified CHA2DS2-VASc score as an independent risk factor for ischemic stroke and TIA in patients with IAB without AF [26]. CHA2DS2-VASc score includes various independent risk factors for sIBL. Although, presence of hypertension, diabetes mellitus, and congestive heart failure were comparable solitarily between the two groups, as a whole parameter, CHA2DS2-VASc score was associated with sIBL in our population.
Some limitations of this study should be acknowledged. This is a single center study. Baseline characteristics and symptoms were self-reported by some patients. Other potential conditions that may predispose to arterial embolism were not evaluated.Patients with asymptomatic AF episodes could not be evaluated with clinical assessment only thus evaluation of patients with holter monitoring and other rhythm monitoring devices would effect results.The number of patients that developed new-onset AF at 12 months was limited. Thus we could not further analyze the predictors of new-onset AF.
Interatrial block detected by the surface ECG can help in identifying patients at high risk of sIBL.
Conflict of Interest/Disclosure
None.