Incidence of New Onset Atrial Fibrillation After Cardiovascular Surgery in Vietnam: Results From A Novel Screening Strategy
Linh Ngo123, Thinh Duc2, Ba Vu Van2, KienTrung Hoang2, Dzung Tien Le2, Huu Cong Nguyen2, Thuy Tran Nguyen2, Ben Freedman4, Nicole Lowres4
1Faculty of Medicine, The University of Queensland, Queensland, Australia.2Department of Cardiovascular and Thoracic Surgery, Cardiovascular Centre, E Hospital, Hanoi, Vietnam.3Department of Cardiology, The Prince Charles Hospital, Queensland, Australia.4Heart Research Institute, Charles Perkins Centre, The University of Sydney, New South Wales, Australia.
To examine the incidence of atrial fibrillation (AF) newly developed after cardiovascular surgery in Vietnam, its associated risk factors, and postoperative complications. We also sought to evaluate the feasibility of a novel screening strategy for post-operative AF (POAF) using the combination of two portable devices.
Single-centre, prospective cohort study at the Cardiovascular Centre, E Hospital, Hanoi, Vietnam. All patients aged≥18 years, undergoing cardiovascular surgery and in sinus rhythm preoperatively were eligible. The primary outcome was occurrence of new-onset POAF detected by hand-held single-lead electrocardiography (ECG) or a sphygmomanometer with AF-detection algorithm. Multivariate logistic regression was used to identify risk factors of developing post-operative AF. Feasibility was evaluated by compliance to the protocol and semi-structured interviews.
112 patients were enrolled between 2018-2019: mean age 52.9±12.2 years; 50.9% female;92.0% (n=103) valve surgery; 9.8% (n=11)coronary surgery. New-onset POAF developed in 49patients (43.8%) with median time to onset 1.27days (IQR 0.96 -2.00 days). Age≥65 years was the only significant risk factor for the development of POAF(OR 3.78, 95% CI 1.16-12.34).The median thromboembolism risk scores (CHA2DS2-VASc score) were comparable among patients with and without POAF (1.0 vs. 1.0, p=0.104). The occurrence of POAF was associated with higher rates of postoperative complications (24.5% vs. 3.2%, p<0.001). Both doctors and nurses found this screening strategy feasible to be implemented long-term with the main difficulties being the instructions on both devices were in English, and an increase in workload.
In this single-centre study, new-onset POAF occurred in 43.8% of patients who underwent cardiovascular surgery. This novel POAF screening strategy was feasible in a low resource setting, and its implementation could be improved by providing continuous training and translation to local language.
Key Words : .
Dr Linh Ngo, Northside Clinical Unit, The Prince Charles Hospital, 627 Rode Road, Chermside, QLD, Australia, 4032
Up to 80% of patients undergoing cardiac surgery could develop new atrial fibrillation (AF) – a cardiac rhythm disorder1. Besides its high incidence, this arrhythmia is also associated with a higher risk of stroke, and worse surgical outcomes including higher risk of death, infections, prolonged length of stay, and increased healthcare cost 2.
In Vietnam, data regarding AF are sparse, with only three studies identified in the literature. One study has shown the estimated the prevalence of AF among elderly patients admitted to the National Geriatric Hospital was 3.9%, among which22.9% did not receive guideline-recommended anticoagulation3. The other two studies, in surgical settings, focused on treatment of pre-existing AF with one investigating the use of intraoperative amiodarone (an anti-arrhythmic drug)4 and the other examining the application of an additional Cox-Maze procedure5. To our knowledge, evaluation of new-onset post-operative AF (POAF) has never been conducted in Vietnam, in part due to the limited resources for screening. Therefore, it is important to examine the incidence of POAF in Vietnam to provide more insights into this common post-surgical complication.
Accordingly, we developed a novel POAF-screening strategy using two devices that could detect AF with high specificity and sensitivity while minimally increase the workload of the involved staff. We sought to investigate the incidence of POAF, its associated risk factors and its association with other post-operative complications. The results of this study will provide preliminary data regarding POAF, increase the awareness of this common disorder, and assist efforts to improve POAF detection and outcomes after cardiovascular surgery in Vietnam.
This was a prospective single-centre study testing a novel strategy to screen for POAF, at the Cardiovascular Centre, E Hospital, Hanoi Vietnam between August 2018 – December 2019. Ethical approval was granted by the Scientific Board of Cardiovascular Centre, Hanoi, Vietnam (reference number 2862). The full study protocol has been published previously 6, and is summarised in brief below.
Consecutive patients who were ≥18 years old, undergoing coronary artery bypass graft (CABG) surgery and/or valve surgery and in sinus rhythm prior to operation were eligible for inclusion. Patients with known AF (we did not screen for history of atrial flutter), congenital heart diseases, and those with 3rd degree atrioventricular nodal block requiring pacemaker after surgery were excluded. Written informed consent was obtained from all participants.
In brief, participants were screened for POAF daily from day-1 post-surgery until hospital discharge. During their Intensive Care Unit (ICU) stay, nursing staff reviewed the participants bedside patient monitor hourly for heart rate observations (as part of usual care). If AF was suspected on the monitor, then a 30-second single-lead ECG recording was taken to document the participant’s heart rhythm using the hand-held smartphone Alive CorKardia Mobile device [Figure 1]as no facility exists to print the trace from the bedside monitor. The Alive CorKardia device records a 30-second single-lead ECG, and provides an automated algorithm diagnosis with a sensitivity of 98% and specificity of 97% 7.
Figure 1. AliveCorKardia Mobile device and app
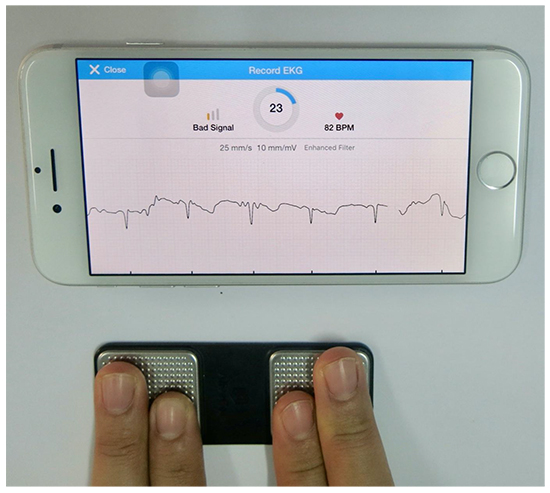
When a patient was transferred from ICU to the Department of Thoracic and Cardiovascular Surgery, POAF screening was then performed 3-times a day using the Micro life BP200 Afib sphygmomanometer [Figure 2] instead of the standard-care BP monitor. The Micro life sphygmomanometer records three consecutive measurements and uses an algorithm to automatically detect irregular heart rhythm 8. If AF was suspected, a single-lead ECG was recorded using the Alive CorKardia Device.
If AF was suspected, the treating physicians were notified to review the patient and the single-lead ECG trace, ordering a 12-lead ECG where necessary. All ECGs were reviewed and confirmed by the investigator (Dr Do), and AF episodes ≥30 seconds were classified as POAF (refer to [] for a detailed pathway of POAF screening).
Figure 2. Microlife BP200 Afib

. The incidence of POAF: the percentage of patients with new-onset AF after cardiac surgery out of the total number of patients included in the study (measured with the Alive CorKardia Mobile and confirmed with a 12-lead ECG).
. Feasibility of monitoring cardiac surgery patients for POAF during their inpatient stay, in Cardiovascular Centre, E Hospital (evaluated by compliance to the protocol, and qualitative process evaluation data using semi-structured interviews with doctors and nurses involved in the screening for POAF). The structured interview is included as supplementary appendix.
. Thromboembolic and bleeding risk profile of patients with POAF (measured using the CHADSVASC score and HASBLED score)9.
. Risk factors associated with development of POAF: including demographic data, types of heart disease, co-morbidities, clinical laboratory tests, and intraoperative parameters.
. Postoperative complications associated with POAF: including infections, ICU length of stay, postoperative hospital length of stay, reoperation, and bleeding events.
Data are presented as frequencies and percentages for categorical variables. For continuous ones, data are presented as mean and standard deviation (SD) if normally distributed (if the mean and median are quite similar) or median and interquartile range (IQR) otherwise. Differences between groups were compared using student T-test or Mann-Whitney U-test for continuous variables and Chi-square or Fisher’s exact test for categorical variables where appropriate. We also reported the difference in means or medians among patients with POAF and those without POAF. The corresponding 95% confidence intervals (CI) were estimated using the mean and standard deviation of each group 10 or bootstrapping techniques with 1000 replications respectively 11.
To identify risk factors for developing POAF, we used multivariate logistic regression with independent variables including age, gender, and comorbidities. Candidate variables including those which are significant in univariate analysis (p<0.25). Backward elimination was applied until only significant variables with p<0.05 remained in the model. Results are reported as frequency and percentages for incidences of events, odd ratio (OR) and 95% confidence intervals (CI) for logistic regression. All analyses were performed using STATA version 16.0. A p value of <0.05 with two-tailed analysis is considered statistically significant.
Between August 2018 and December 2019, 337 patients underwent coronary and/or valvular surgery in our centre. Among these patients, 113met the selection criteria and provided informed consent, as indicated in the study flow diagram [Figure 3]. After surgery, one patient developed complete heart block requiring pacing and was excluded from the study, resulting in a final sample size of 112 patients. Participant baseline characteristics are summarised in [Table 1]. The mean age of participants was 52.9±12.2years, 50.9% were females and the median total length of stay was 22.0days (IQR: 18.0-29.0days). Most patients underwent valvular surgery (n=103, 92.0%) with only 9.8%(n=11) undergoing CABG. Participants had a wide range of cardiac comorbidities including hypertension (n=25, 22.3%), heart failure (n=16, 14.3%), and non-cardiac comorbidities such as diabetes (n=9, 8.0%) and renal failure(n=43, 38.4%). The median CHA2DS2-VASc score was 1 (IQR:0to2), and median HASBLED score was 0 (IQR: 0 to 1). Among patients undergoing valvular surgery, 18 patients underwent valve repair, 34 received bioprosthetic valve, 30 received mechanical valve, and 21 patients underwent aortic valve reconstruction surgery using autologous pericardium. The mean left ventricular ejection fraction was 63.2%, mean left ventricular diameter was 53.0 mm, and mean left atrial diameter was 42.3 mm.
Table 1. Baseline characteristics of the study cohort
| Characteristics |
Overall cohort N=112 |
With POAF N= 49 |
No POAF N=63 |
Difference in means or mediansꝉ (mean and 95% CI) |
P value* |
| Age (mean ± SD) |
52.9 ± 12.2 |
55.2 ± 13.5 |
51.1 ± 10.9 |
4.2 (-0.5 – 8.8) |
0.074 |
| Age group |
| <65 years old |
92 (82.1%) |
35 (71.4%) |
57 (90.5%) |
|
0.009 |
| ≥ 65 years old |
20 (17.9%) |
14(28.6%) |
6 (9.5%) |
|
|
| Female |
57 (50.9%) |
27 (55.1%) |
33 (52.4%) |
|
0.432 |
| BMI (kg/m2, mean ± SD) |
21.7 ± 3.2 |
21.6 ± 3.7 |
21.7 ± 2.9 |
-0.1 (-1.4 – 1.1) |
0.867 |
| Total LOS (median [IQR]) (days) |
22.0 (18.0 – 29.0) |
27.0 (21.0 – 35.0) |
21.0 (17.0 – 24.0) |
6 (1.3 – 10.7) |
0.002 |
| Post-operative LOS (median [IQR]) (days) |
12.0 (10.0 – 17.0) |
15.0 (11.0 – 23.0) |
11.0 (9.0 – 14.0) |
4 (1.5 – 6.5) |
0.003 |
| ICU LOS (median [IQR]) (days) |
4.0 (3.0 – 6.5) |
6.0 (4.0 – 8.0) |
3.0 (3.0 – 5.0) |
3 (1.3 – 4.7) |
<0.001 |
| Type of surgery |
| Coronary artery surgery |
11 (9.8%) |
4 (8.2%) |
7 (11.1%) |
|
0.753 |
| Valve surgery |
103 (92.0%) |
47 (95.9 %) |
56 (88.9%) |
|
0.175 |
| Combined surgery |
2 (2.0%) |
2 (4.1%) |
0 (0.0%) |
) |
0.189 |
| Type of valvular disease |
| Aortic valve surgery |
52 (46.4%) |
22 (44.9%) |
30 (47.6%) |
|
0.775 |
| Mitral valve surgery |
61 (54.5%) |
29 (59.2%) |
32 (50.8%) |
|
0.376 |
| Surgery involved more than one valve |
29 (25.9%) |
15 (30.6%) |
14 (22.2%) |
|
0.315 |
| Type of prosthetic valve used |
| None |
18 (16.1%) |
10 (21.3%) |
8 (14.3%) |
|
0.159 |
| Bioprosthetic |
34 (33.0%) |
19 (40.4%) |
15 (26.8%) |
|
|
| Mechanical |
30 (29.1%) |
9 (19.2%) |
21 (37.5%) |
|
|
| Autologous pericardium |
21 (20.4%) |
9 (19.2%) |
12 (21.4%) |
|
|
| Cardiac comorbidities |
| Hypertension |
25 (22.3%) |
12 (24.5%) |
13 (20.6%) |
|
0.627 |
| Vascular disease |
16 (14.3%) |
10 (20.4%) |
6 (9.5%) |
|
0.102 |
| Coronary artery disease |
12 (10.7%) |
5 (10.2%) |
7 (11.1%) |
|
0.878 |
| Heart failure |
16 (14.3%) |
9 (18.4%) |
7 (11.1%) |
|
0.276 |
| Non-cardiac comorbidities |
| Diabetes |
9 (8.0%) |
6 (12.2%) |
3 (4.8%) |
|
0.176 |
| History of stroke |
3 (2.7%) |
2 (4.2%) |
1 (1.6%) |
|
0.577 |
| Renal failure |
43 (38.4%) |
22 (44.9%) |
21 (33.3%) |
|
0.212 |
| Chronic hepatitis |
3 (2.7%) |
3 (6.1%) |
0 (0.0%) |
|
0.081 |
| Chronic lung disease |
4 (3.6%) |
2 (4.1%) |
2 (3.2%) |
|
1.000 |
| Thyroid disease |
3 (2.7%) |
1 (2.0%) |
2 (3.2%) |
|
1.000 |
| CHA2DS2-VAScscore (median, IQR) |
1 (0 – 2) |
1 (1 – 2.5) |
1 (0 – 2) |
0 (-0.6 – 0.6) |
0.155 |
| HASBLED score (median, IQR) |
0 (0 – 1) |
0 (0 – 1) |
0 (0 – 1) |
0 (-0.7 – 0.7) |
0.201 |
| Pre-operative echocardiography |
| Left ventricular ejection fraction (%, mean±SD) |
63.2 ± 11.8 |
63.4 ± 11.8 |
63.1 ± 11.9 |
0.4 (-4.0 – 4.8) |
0.870 |
| Left ventricular diameter (mm, mean±SD) |
53.0 ± 11.7 |
54.0 ± 12.2 |
52.3 ± 11.5 |
1.7 (-2.8 – 6.1) |
0.455 |
| Left atrial parameter (mm, mean±SD) |
42.3 ± 8.8 |
43.3 ± 8.6 |
41.6 ± 8.9 |
1.7 (-1.5 – 5.0) |
0.301 |
Footnote: CI=confidence interval, SD=standard deviation, BMI=body mass index, LOS=length of stay, IQR=interquartile range, ICU=intensive care unit, eGFR=estimated glomerular filtration rate, CHA2DS2-VASc score=a score to evaluate stroke risk of patients with atrial fibrillation (C=Congestive Heart Failure, H=hypertension, A=Age, D=Diabetes, S=Stroke, Vasc=Vascular disease), HASBLED score= a score to evaluate major bleeding risk of patients with atrial fibrillation (H=Hypertension, A=Abnormal liver or kidney function, S=Stroke, B=history of major Bleeding, L=Labile international normalised ratio, E=Elderly, D=Drugs or alcohol).
Figure 3. Study flow chart
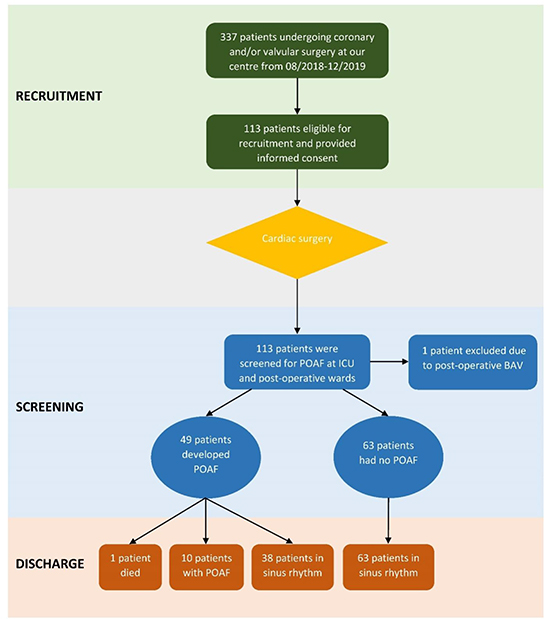
New-onset POAF occurred in 43.8% (n=49)of participants post-surgery. The median time to first occurrence of new-onset POAF was 1.27 days (IQR 0.96 – 2.0 days) [Figure 4]. Almost all episodes (48/49 patients, 98.0%) were captured in the ICU by using AliveCorKardia Device. The remaining one case was identified on the Thoracic and Cardiovascular Surgery ward.
Figure 4. Timing of new-onset POAF
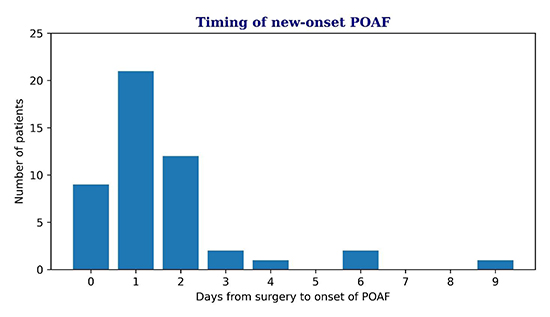
Footnote: POAF=post-operative atrial fibrillation
Most patients with POAF (46/49, 93.9%) were consulted by a cardiologist. The primary treatment for POAF was antiarrhythmic drugs (amiodarone n=24; digoxin n=3). At discharge, 79.6% (39/49) of POAF cases converted to sinus rhythm, mainly with the use of anti-arrhythmic medications while 13 cases having spontaneously conversion. The other 20.4% (10/49) of patients remained in AF, of whom 7 had undergone bioprosthetic valve replacement, 2 received mechanical valves, and 1 valve repair surgery.
Patients with POAF had higher proportion of the older age group (≥65 years old, 28.6% vs. 9.5%, p=0.009). Rates of other comorbidities were comparable between patients who experienced POAF and who did not. Similar, median CHA2DS2-VASc (1.0 vs. 1.0, p=0.155) and HASBLED (0.0 vs.0.0, p=0.201) were comparable between groups. When different types of surgery were considered, incidences of POAF were comparable among patients underwent coronary artery surgery and valve surgery (36.4% vs. 44.6%, p=0.753).
Variables considered for logistic regression included age group (OR 3.68, 95% CI 1.30 – 10.49, p=0.014), vascular disease (OR 2.38, 95% CI 0.80 – 7.06, p=0.120), diabetes (OR 2.73, 95% CI 0.65 – 11.50, p=0.172), renal failure (OR 1.57, 95% CI 0.73 – 3.38, p=0.247), and left atrial diameter (OR 1.03, 95% CI 0.98 – 1.07, p=0.247) [Table 2]. After logistic regression, we found that older age (≥65 years old) was the only factor significantly associated with an increased risk of developing POAF (adjusted OR 4.53, 95% CI 1.34 – 15.38, p=0.015).
Table 2. Risk factor associated with the occurrence of new-onset post-operative atrial fibrillation
| Characteristics |
Univariate logistic regression |
Multivariate logistic regression |
|
|
OR (95% CI) |
P value |
aOR (95% CI) |
P value |
| Age |
1.03 (1.00 – 1.06) |
0.076 |
|
|
| Age group |
|
|
|
|
| <65 years old (reference group) |
|
|
|
|
| ≥65 years old |
3.80 (1.34 – 10.80) |
0.012 |
3.78 (1.16 – 12.34) |
0.028 |
| Female gender |
1.47 (0.69 – 3.11) |
0.318 |
|
|
| BMI |
0.99 (0.88 – 1.11) |
0.865 |
|
|
| Type of surgery |
|
|
|
|
| Coronary artery surgery (reference group) |
|
|
|
|
| Non-coronary surgery |
0.71 (0.20 – 2.58) |
0.604 |
|
|
| Cardiac comorbidities |
|
|
|
|
| Hypertension |
1.25 (0.51 – 3.04) |
0.627 |
|
|
| Vascular disease |
2.44 (0.82 – 7.25) |
0.110 |
1.88 (0.56 – 6.30) |
0.305 |
| Coronary artery disease |
0.91 (0.27 – 3.05) |
0.878 |
|
|
| Heart failure |
1.80 (0.62 – 5.24) |
0.281 |
|
|
| Non-cardiac comorbidities |
|
|
|
|
| Diabetes |
2.79 (0.66 – 11.78) |
0.163 |
2.06 (0.42 – 10.09) |
0.371 |
| History of stroke |
2.70 (0.24 – 30.64) |
0.424 |
|
|
| Renal failure |
1.63 (0.76 – 3.52) |
0.213 |
0.95 (0.38 – 2.36) |
0.912 |
| Chronic hepatitis |
NA |
NA |
|
|
| Chronic lung disease |
1.30 (0.18 – 9.56) |
0.798 |
|
|
| Thyroid disease |
0.64 (0.06 – 7.22) |
0.715 |
|
|
| Pre-operative echocardiography |
|
|
|
|
| Left ventricular ejection fraction |
1.00 (0.97 – 1.04) |
0.869 |
|
|
| Left ventricular diameter |
1.01 (0.98 – 1.05) |
0.452 |
|
|
| Left atrial diameter |
1.02 (0.98 – 1.07) |
0.299 |
|
|
Footnote: OR=odd ratio, aOR=adjusted odd ratio, CI=confidence interval, NA=not applicable
Postoperative complications
Patients with POAF spent significantly longer time in the ICU (6.0 vs. 3.0 days, difference in medians: 3 days [95%CI 1.3-4.7], p<0.001) and in-hospital post-surgery (15.0 vs. 11.0 days, difference in medias: 4 days [95%CI 1.5-6.5], p=0.002) compared with those without POAF. POAF patients also had higher rates of major complications (26.0% vs 3.2%, p <0.001) which was driven by higher rate of pulmonary oedema (12.0% vs. 0.0%, p=0.006) [Table 3]. Rates of death (4.0% vs. 0.0%, p=0.194), stroke (2.0% vs. 0.0%, p =0.442), major bleeding (8.0% vs. 1.6%, p=0.169), sepsis (4.0% vs 0.0%, p=0.194), delirium (14.0% vs. 6.4%, p=0.211) and pleural effusion (6.0% vs. 1.6%, p=0.320) were all higher in the POAF group although the differences did not reach statistical significance.
Table 3. Association of POAF occurrence and other postoperative complications.
| Complications |
Overall cohort N=113 |
With POAF N=50 |
No POAF N=63 |
P value |
| Any major complication |
14 (12.5%) |
12 (24.5%) |
2 (3.2%) |
<0.001 |
| Death |
1 (0.9%) |
1 (2.0%) |
0 (0.0%) |
0.437 |
| Stroke |
1 (0.9%) |
1 (2.0%) |
0 (0.0%) |
0.437 |
| Major bleeding |
5 (4.5%) |
4 (8.2%) |
1 (1.6%) |
0.166 |
| Sepsis |
1 (0.9%) |
1 (2.0%) |
0 (0.0%) |
0.437 |
| Pulmonary oedema |
6 (5.4%) |
6 (12.2%) |
0 (0.0%) |
0.006 |
| Delirium |
11 (9.8%) |
7 (14.3%) |
4 (6.4%) |
0.206 |
| Pleural effusion |
4 (3.6%) |
3 (6.1%) |
1 (1.6%) |
0.317 |
Feasibility of POAF screening strategy
Overall, the compliance rate was high and most of interviewees believed that this strategy could be implemented in the long-term, especially if regular training and Vietnamese translation are added.
Twelve staff including five doctors and seven nurses completed the semi-structured interviews (Supplemental Appendix 1). All nurses who performed the POAF screening complied with the protocol. Most staffs reported the devices to be smaller, more convenient, quicker to be deployed, and provided results faster than the standard ECG recorder. They were supportive of screening for POAF, as they realised that the importance of POAF has not been adequately addressed in Vietnam. Almost all interviewees (11/12) thought that it may be possible to implement the POAF screening protocol in the long-term.
However, several difficulties were reported with the implementation of these devices. Firstly, both devices operate in English and not Vietnamese, which required prolonged time to follow the instructions and record the ECG, especially when errors happened. Secondly, the patients were mostly unconscious for several days post-surgery which significantly affected the patient-device contact and accordingly, quality of the recorded ECG. Therefore, it often took 15 minutes to record a 30-second single-lead ECG tracing with the Alive-Cor device (including time for patient preparation, repeated recordings due to low-quality ECG) while the Micro life device may take up to 5 minutes to measure blood pressure for 3 times consecutively. Consequently, staffs acknowledged that the POAF screening increased their usual workload moderately due to extra time needed to explain to the patients and record the ECG or measure blood pressure. Another interesting finding was that the quality of recording was significantly affected by the contact between the patient and the Alive CorKardia device given that the tracings were often collected in the postoperative setting on sedated patients. One nurse suggested that this could be resolved, at least in part, by applying 70-degree ethanol alcohol on the patient’s fingers before recording.
The above issues were acknowledged to potentially impact the implementation and sustainability of the POAF screening strategy. Suggested solutions to overcome these hurdles and facilitate successful implementation of the POAF screening strategy include continuous training, and translation of the Alive CorKarida Device into Vietnamese. Specifically, the interviewees suggested that a monthly training session on how to recognize POAF on ECG tracing, how to use these devices, in addition to Vietnamese translation of the instructions could significantly facilitate the long-term implementation of such POAF screening strategy. They also suggested that the identification of new-onset POAF could be improved by using a telemetry system in the ICU that has the capacity to store all ECG recordings that could be reviewed later.
In this first-ever POAF screening study in Vietnam, we found that the novel POAF screening strategy was feasible and detected a POAF incidence of44.2%. The only risk factor for developing POAF identified in our study was older age (≥65 years old). The occurrence of POAF is associated with significantly prolonged ICU and post-operative length of stay, as well as higher risk of post-surgical pulmonary oedema. Staffs who were involved in this study showed good compliance with study protocol and provided important insights to its future implementation. Collectively, these findings suggest that the novel POAF screening strategy is feasible in a limited-resources-setting and provide some exploratory data regarding POAF in Vietnam.
AF newly develops after cardiac surgery has long been recognised as an important complication due to its high incidence as well as the worse surgical outcomes associated with this condition2. In Vietnam, however, little is known about this devastating disorder, in part due to the lack of equipment like telemetry as well as the shortages of staffs who already have a high workload. Consequently, there is a lack of awareness of POAF and strategies to prevent it. This study demonstrated that our novel POAF screening strategy is feasible as it is simple, uses devices that require minimal training and is integrated into the normal workflow so it does not significantly increase workload for staff6. This is in line with two other recent studies that also demonstrated the feasibility of using these devices in low-resource settings in the community in both India 12and Thailand 13. Importantly, the semi-structure interviews provided important insights into the potential long-term implementation of this novel POAF screening strategy, identifying suggestions for improvement such as additional training and the need for translation of the devices into Vietnamese. Furthermore, as the majority of POAF cases were identified in the ICU, the potential use of telemetry that has the capability to store ECGs, could be a long-term solution to POAF screening, however the cost of this equipment would need to be considered.
Our study has provided the first preliminary data of POAF in Vietnam. Incidence of POAF in this study (43.8%) falls in the centre of the range reported in the literature(10-80%) 2, 14-16. However, this rate is much higher than the 3.9% reported among elderly patients admitted to the National Geriatrics Hospital in Vietnam3, suggesting that POAF is not a trivial event which occurs with much higher incidence compared with that in the general population. Our study identified age ≥65 years as arisk factor of POAF and showed that the occurrence of this arrhythmia was associated with prolonged length of stay and higher risk of postoperative complications, which are consistent with previous literature1. Encouragingly, most events were consulted with a cardiologist and that most of these patients were discharged on sinus rhythm. However, ten patients were still in atrial fibrillation at discharge, of which seven had a bioprosthetic valve that may require long-term anticoagulation beyond the typically recommended three-month period 17. Collectively, our findings confirm that in Vietnam, new-onset AF also had high incidence and associated with worse outcomes for patients undergoing cardiac surgery.
Some practical implications could be drawn from our findings. Firstly, healthcare providers (e.g. physicians, surgeons, doctors and nurses) taking care of patients after cardiac surgery in Vietnam all need to be more aware of the risk of developing POAF after cardiovascular surgery given its high incidence and its association with higher risk of postoperative complications, as well as its long-term management. Secondly, although our study was not powered to identify causes of POAF, we found advanced age to be the only risk factor and efforts to prevent patients from developing POAF may need to focus more on this specific group of patients. There are several strategies that have been shown to be effective in reducing the incidence of new-onset AF. For example, a systematic review of eight randomised trial involving 1,060 patients reported that the use of vitamin C treatment was associated with a more than 50% reduction in rate of POAF 18. Other possible therapies include beta-blocker19, corticosteroid 20, and colchicine 21. We also suggest that this POAF screening strategy should be implemented in other centres to provide a more comprehensive understanding about POAF after cardiovascular surgery in Vietnam. It could also be used for POAF screening with other surgeries, or to follow response to therapeutic interventions like beta blockers, amiodarone, or Cox-Maze procedure.
When interpreting our results, several limitations should be considered. This is only a single-centre experience with small sample size that has limited the statistical power of several comparisons. Nevertheless, it has provided foundation for future studies including those applying this POAF screening strategy in similar settings, or with other surgeries, or those using this strategy to follow-up response to treatment of POAF. The variable educational background and skills of the participating staffs in two different departments may have missed some cases and underestimated the true incidence of POAF.
In this single-centre study, using a novel POAF screening strategy, we found that 44.2% of patients undergoing cardiovascular surgery experienced new-onset POAF which was associated with higher risk of postoperative complications. Further studies using this strategy in other settings are encouraged, as well as to monitor response to therapeutic interventions.