Association Between Left Atrial Compression And Atrial Fibrillation: A Case Presentation And A Short Review Of Literature
Niloy Ahmed, MD, Morales-Mangual Carlos, MD, Gunsburg Moshe, MD, Rosen Yitzhak, MD
Department of Medicine, Brookdale University Hospital, Brooklyn, New York, USA.
This case report describes a patient who developed palpitations and chest pain and was found to be in atrial fibrillation, which was likely due to the presence of an extra-cardiac mass. This was compressing the left atrium. The mass was related to small cell carcinoma, which decreased significantly in size after chemotherapy. Resolution of the atrial fibrillation correlated temporally with reduction in the size of the mass and alleviation of the left atrial compression.
Key Words : Atrial Fibrillation, Compressing, Mass, Left Atrium, New Onset.
Correspondence to: Carlos Morales-Mangual, Brookdale University Hospital, Department of Medicine, 1 Brookdale Plaza, Brooklyn, NY 11212.
Atrial fibrillation (AF) is the most common sustained cardiac arrhythmia characterized by irregular, disorganized and rapid atrial activation leading to an irregular ventricular rhythm.1 Almost any cardiovascular condition can predispose to AF, common causes being hypertension, coronary artery disease, heart failure, valvular heart disease, cardiomyopathy, pericarditis. Extra-cardiac causes include thyrotoxicosis, chest trauma, thoracic surgery, obstructive sleep apnea, pulmonary embolism, medication use, alcohol excess and withdrawal etc.1,2,3
The left atrium (LA) is highly susceptible to compression by extra-cardiac structures. There have been reports of LA compression by bronchogenic cysts,4 esophageal cancer,5 achalasia,6 diaphragmatic hernia,7 aorta8 etc. Such compression usually leads to hemodynamic instability, decreased cardiac output, pulmonary congestion and hypoxia.8
In this paper, we report a case of LA compression and new onset AF, wherein the AF resolved after chemotherapy and discuss the possible association between LA compression and new onset AF.
66 year old female with a past medical history including hypertension, COPD, interstitial lung disease (ILD) and peripheral neuropathy presented to the emergency room (ER) with complaints of worsening shortness of breath for one week and substernal chest pain radiating to back, 9/10 on intensity, which began after drinking soup. The pain lasted for 3 hours and was relieved by sublingual nitroglycerin in the ER. Her troponins were negative all along. Initial EKG showed sinus rhythm without any acute changes. The patient also reported that she had been nauseated and felt as if solid food was sticking in her chest for about 3 weeks. CT chest was done that showed an infracarinal mass (6.2x7.7x8.9 cm) that had increased in size, moderate mediastinal lymphadenopathy, right lower lobe masses and nodule in the right upper lobe along with pulmonary changes consistent with emphysema and ILD.
On the second day, patient had persistent chest discomfort and was found to be tachycardic. An EKG showed AF with a rapid ventricular response (137 bpm). This was new with no known previous history of AF. CT angiogram of the chest ruled out pulmonary embolism and reconfirmed the presence of enlarged mediastinal and hilar lymph nodes along with an 8.0 cm mass/node in the subcarinal space (see figure #1 below) that was occluding the right lower lobe bronchus. Echocardiogram done early in the presentation showed that there was an echogenic mass located outside of the lateral free wall, of the left atrium causing partial compression of the left atrial cavity (see figure #2 below).
Figure 1.
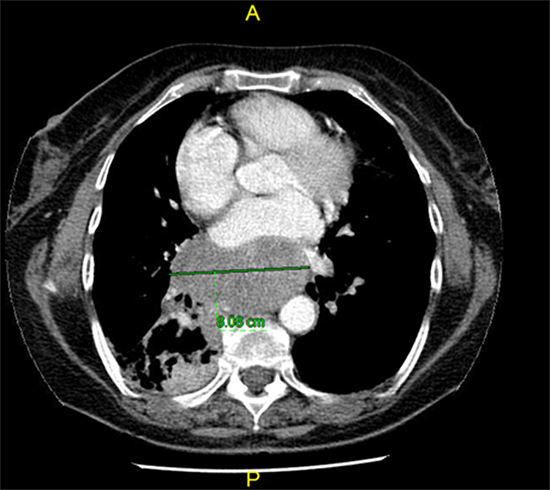
Figure 2.
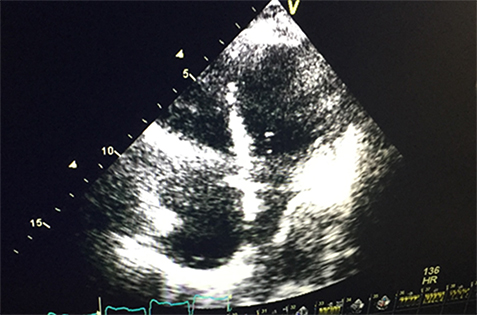
A biopsy of the lung masses revealed small cell lung cancer. The patient received four cycles of chemotherapy, which included carboplatin and etoposide. Atrial fibrillation converted to sinus rhythm without electrical or pharmacological cardioversion. A follow-up chest CT four months later and after receiving chemotherapy showed a decrease in the size of the mediastinal and subcarinal nodes (2.3cm and 4.3cm in size)(see figure #3) with an increase in size of the right lower lobe mass. Patient remained in sinus rhythm.
Figure 3.
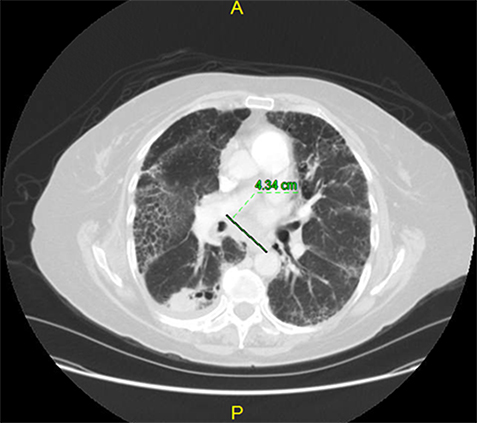
In summary, this was a patient who developed new AF, palpitations and chest pain, which was likely due to the presence of an extra-cardiac mass, which was compressing the LA. The mass was related to small cell carcinoma, which decreased significantly in size after chemotherapy. Resolution of the AF correlated temporally with reduction in the size of the mass and alleviation of the LA compression.
Although a causal relationship is difficult to establish, several case reports have tried to show an association between external compression of the LA and AF.8 Upile et al described a case where AF was attributed to external compression of LA by an enlarged esophagus due to achalasia. The AF resolved after removal of food debris from the esophagus.6 Bayraktar et al reported a case of a patient with a mid esophageal mass (squamous cell carcinoma on biopsy) who was found to have one episode of AF. Chest CT showed subcarinal lymphadenopathy and esophageal thickening resulting in compression of the LA. While the patient has had HTN for 5 years, an echocardiogram revealed a structurally normal heart. Hence it was proposed that AF was precipitated by the esophageal carcinoma compressing the LA or pulmonary veins.5 Volpi et al described a case of a patient with a bronchogenic cyst compressing the LA leading to reduced LA cavity size on echocardiogram and associated AF. The authors postulate that the AF was probably due to mechanical stretching of atrial myocardial fibers.4 One case report describes a non-aneurysmatic segment of the descending aorta compressing the LA which was felt to be a possible cause of significant hemodynamic compromise, pulmonary congestion and AF in that patient.8 Malik et al reported on a patient who had palpitation during swallowing and was shown to have AF induced by deglutition.9 In our case, the patient did not have a previous history of AF; it is very likely that both AF and difficulty in swallowing were related to the subcarinal mass.
Table 1. This table shows several reported cases of compressing masses and their association with atrial fibrillation
| Clinical scenario |
Association |
Ref |
| 36 years old man with unremarkable past history presented with palpitation, AF found on EKG. CT scan and echocardiography showed a mediastinal cystic mass (later diagnosed as bronchogenic cyst) that was compressing the LA. |
No apparent cause of AF other than external compression. The case report does not mention if the patient stayed sinus after the mass was surgically removed. |
4 |
| 58 years old man presented with dysphagia, later diagnosed with esophageal carcinoma. His initial EKG was sinus, later developed AF that converted to sinus spontaneously. CT scan showed subcarinal lymphadenopathy and esophageal thickening that compressed LA. |
No other cause of AF identified. AF was short-lived and did not recur. |
5 |
| 84 years old woman presented with dysphagia, later diagnosed as achalasia. She was found to have AF. |
Patient reverted back to sinus rhythm after about 300 ml food debris was removed from esophagus. |
6 |
| 75 years old woman presented with palpitation was diagnosed with AF. CT scan and echocardiography showed descending aorta compressing LA. |
Possible causes of AF include external compression, hypertension and heart failure (ejection fraction 44%). |
8 |
| 38 years old woman without significant medical history presented with palpitation during swallowing. She was found to have AF during deglutition. |
Esophageal manometry with simultaneous EKG showed AF occurring with deglutition. No other cause of AF was found. |
9 |
While a definite causal relationship has not been established, multiple case-reports have shown a possible association between mechanical compression of the LA and AF. It is possible that such compression may cause ectopic beats in susceptible individuals leading to AF. Echocardiography is a nice modality through which to demonstrate compression of the LA. Further study is needed to establish a causal relationship and predict the pattern of AF in cases of LA compression. Further understanding of the electrical and mechanical mechanisms underlying this entity may have significant therapeutic implications.