Hyperacute And Chronic Changes In Cerebral Magnetic Resonance Images After Pvac, nmarq And Epicardial Thoracoscopic Surgical Ablation For Paroxysmal Atrial Fibrillation
Conn Sugihara MBBS, Neil Barlow MBBS, Emma Owens MBBS, David Sallomi MB ChB, Neil Sulke MD
Eastbourne Hospital, East Sussex Healthcare NHS Trust, UK.
Threshold testing of cardiac rhythm devices is essential to monitoring the proper functioning of such devices (1). However, the currently method of applying multiple ECG leads to the patient is burdensome and time consuming (2). We are presenting a completely new way to perform cardiac rhythm device threshold testing using pulse oximetry.
Twenty patients, with varying cardiac rhythm devices and pacing modes, were enrolled and had their atrial and ventricular thresholds tested. A comparison was made between simultaneous threshold determinations via the standard EGM based method and the new pulse oximetry based method. 75% of the ventricular threshold tested and 58% of the atrial thresholds tested were the same with the two testing methods. The remainder of the tests (25% of ventricular threshold and 42% of the atrial threshold tests) varied by +0.25 V.
This study shows that pulse oximetry based testing is an accurate, reliable, and easy way to perform cardiac rhythm device threshold testing and may complement traditional methods to perform such tests in the future.
Key Words : Silent Cerebral Event, Atrial Filbrillation Ablation, Thoracoscopic Epicardial Surgical AF Ablation.
Correspondence to: Conn Sugihara,
Eastbourne General Hospital,
Kings Drive, East Sussex,
BN21 2UD, UK.
Patients with atrial fibrillation (AF) are at increased risk of symptomatic cerebral ischaemic events.1 Cerebral magnetic resonance imaging (MRI), especially using Diffusion Weighted Imaging (DWI), is the current gold standard for detection of acute cerebral ischaemia2 in clinical practice. Asymptomatic cerebral events (ACE), defined as changes on DW-MRI without detectable neurological symptoms, have been described in the setting of invasive neurovascular3,4 and cardiac5 procedures. However, since the first report of ACEs in the setting of AF ablation.6 a number of studies have reported an incidence of ablation-related ACE of between 2% and 41%.7-16 ACEs have recently been subdivided into either silent cerebral events (SCE) or silent cerebral lesions (SCL) based on MRI criteria.17
Attention has been focused on the platinum-tipped electrode pulmonary vein ablation catheter (PVAC, Medtronic Inc., Carlsbad, CA, USA ). In initial reports, this decapolar non-irrigated duty-cycled radiofrequency ablation system was associated with the highest rates of ablation-related ACE. However, the PVAC system has been shown to have similar antiarrhythmic efficacy to conventional ablation,18,19 and modifications to the ablation procedure have resulted in an apparent ACE rate comparable to other techniques.7
nMARQ (Biosense Webster, Diamond Bar, CA, USA), like PVAC, is a ‘single-shot’ multipolar pulmonary vein mapping and ablation system.20 A key difference is that all electrodes on the nMARQ catheter are continuously irrigated. Irrigation is thought to reduce the risk of thrombus formation and microbubble cavitation,21 and consequently the incidence of cerebral microembolism.22
Minimally invasive thoracoscopic epicardial surgical AF ablation, an evolution of conventional open surgical AF ablation,23 appears highly effective.24 There is evidence to suggest that epicardial ablation causes fewer cerebral emboli than endocardial ablation.25
This is the first prospective randomised controlled study comparing the incidence of SCE after PVAC using modified techniques, the nMARQ system and thoracoscopic surgical AF ablation.
Study Population and Protocol
A prospective randomised study was conducted in a single tertiary arrhythmia referral centre between May 2012 and September 2014. Patients with symptomatic paroxysmal AF were randomised 1:1:1 to PVAC ablation, nMARQ ablation and surgical AF ablation. The study protocol was developed by the investigators and was approved by the institutional review board and national ethics committee. All patients gave written informed consent. Inclusion criteria were age over 18 and symptomatic paroxysmal AF suitable for AF ablation. Exclusion criteria were: prior cardiac or thoracic surgery, inability to undergo general anaesthesia for AF ablation, pregnancy, the presence of pre-existing permanent pacemakers or implantable loop recorders that did not allow for continuous monitoring for AF occurrence, or were not MRI-safe, and cardiac rhythm disorders other than AF. Patients who had atrial flutter induced during the ablation procedure were not excluded. All patients were offered pre-procedural cerebral MRI (baseline), followed by MRIs as soon as possible after ablation (acute) and 3 months after ablation (follow up).
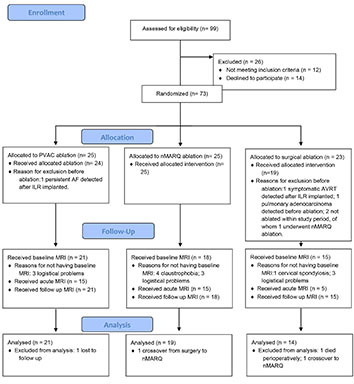
In total, 73 patients were recruited. 10 of 64 patients who were ablated did not undergo pre-procedural cerebral MRI (see Fig 1). 54 patients had both baseline and follow up scans. 12 patients (predominantly patients allocated to surgical ablation) were unable to have an acute scan, all because they were not stable enough to undergo MRI. One patient allocated to surgical ablation crossed over to nMARQ ablation.
Figure 1. Study flow diagram
Cerebral MRI was performed using a 1.5T scanner (Signa HDXT, GE Medical Systems, Milwaukee, WI, USA). Coronal T1 and axial T2, fluid-attenuated inversion recovery (FLAIR) and DWI sequences were acquired, and apparent diffusion coefficient (ADC) maps constructed. Slice thickness was 4-5mm (1mm spacing) for T1, FLAIR and T2 sequences, and 5mm (no spacing) for DWI sequences.
As per the prospectively-defined analysis plan, cerebral infarction (CI) and white matter change (WMC) were defined as a focal lesion (>3mm in any axis) with associated T2 and FLAIR hyperintensity in any part of the lesion. CI was distinguished from WMC if there was corresponding T1 hypointensity within the lesion such that any part of the lesion appeared isointense to cerebrospinal fluid. Acute lesions (AL) were defined as a focal or wedge-shaped hyperintense lesion seen on DWI, with a hypointense signal in the corresponding region on the ADC map. No FLAIR criterion was used to evaluate AL, i.e. asymptomatic ALs are equivalent to silent cerebral events (SCEs). The location and temporal resolution of lesions were analysed. Three blinded consultant radiologists independently analysed all MRI images. Lesions were considered present if independently reported by at least two of the three blinded radiologists.
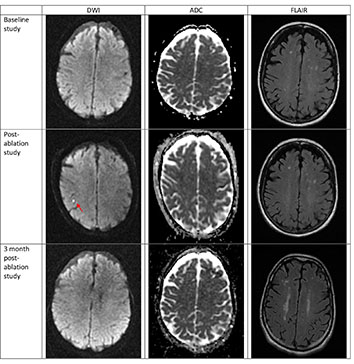
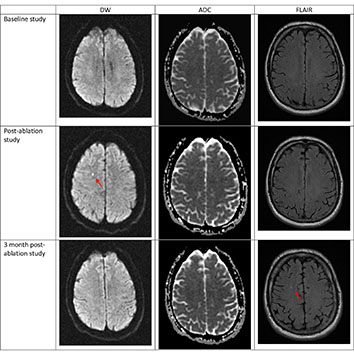
Figure 2. Silent cerebral event (SCE) after nMARQ ablation This patient with a CHA2DS2Vasc score of 2 underwent nMARQ ablation. Baseline MRI shows multiple areas of cerebral white matter change on the FLAIR sequence. A new DWI hyperintense, ADC hypointense lesion is seen on the post ablation study. 3 months after ablation, the lesion is no longer present
All scans were anonymised, and the radiologists were blinded to the treatment assignments throughout. Scans were reported by the radiologists in three phases. In the first phase, radiologists were not aware whether a scan was the first, second or last scan performed. Scans were examined for the presence or absence of CI, WMC or AL without reference to any other study. In the second phase, scans were re-anonymised, and the radiologists examined the 3 month post-ablation MRI in comparison to the baseline MRI. Radiologists assessed whether there was new or increasing CI or WMC. Finally, in the third phase radiologists examined all three scans in patients who had an apparent ablation-related AL (i.e. an acute lesion appearing on the post-ablation scan). Radiologists assessed whether the lesion was new (i.e. not present in the baseline scan), and whether it had resolved (i.e. whether it was detectable on the 3 month MRI).
All patients underwent the Mini Mental State Examination (MMSE) and Montreal Cognitive Assessment (MoCA) cognitive function tests immediately before ablation, 6 weeks post ablation and 3 months post ablation.
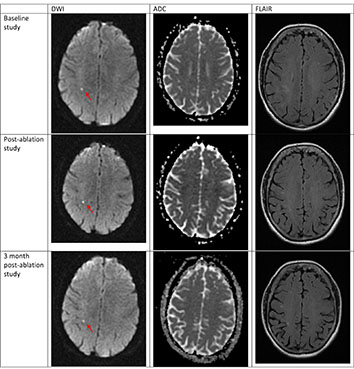
Figure 3. DWI positive lesion present before nMARQ ablation This patient with a CHA2DS2Vasc score of 4 underwent nMARQ ablation. Examination of the post-ablation MRI demonstrates a clear DWI hyperintense, ADC hypointense lesion. If there were no symptoms, this would fit the criteria for a silent cerebral event (SCE). However, this lesion is evident on the pre-ablation study, demonstrating that it is not ablation-related
All patients were therapeutically anticoagulated preprocedurally, and anticoagulation (including with Dabigatran or Rivaroxaban) was continued through the procedure. No routine pre-procedural imaging (e.g. transoesophageal echocardiography) was performed. Through femoral venous access, a decapolar catheter was placed in the coronary sinus. A deflectable trans-septal sheath was used to perform a single trans-septal puncture, after which a bolus of unfractionated Heparin (approximately 70 units per kg of body weight) was injected intravenously. Thereafter, unfractionated Heparin was administered to maintain the activated clotting time (ACT) above 300 seconds whilst the left atrium (LA) was instrumented. Pulmonary vein (PV) anatomy was determined fluoroscopically using the PVAC catheter and guide wire, i.e. without routine left atrial angiography. The PVAC catheter was used to perform PV ablation using the GENius generator Version 15.1, which did not allow simultaneous ablation through the proximal and distal ablation electrodes. PV isolation was tested using the PVAC catheter. Inducibility of arrhythmia was tested with incremental atrial pacing and isoprenaline infusion. PV isolation was rechecked during isoprenaline infusion. A cavotriscuspid isthmus (CTI) line using a standard non-irrigated 8mm ablation catheter was performed if there was prior evidence of atrial flutter or it was induced during the case. Immediately following removal of the left atrial catheter, 25mg to 50mg of Protamine was injected intravenously.
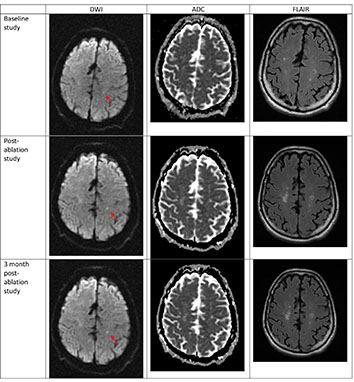
Figure 4. DWI positive lesion present before PVAC ablation This patient, with a CHA2DS2Vasc score of 5, underwent PVAC ablation. As with the previous case, the DWI hyperintense lesion is present prior to ablation
nMARQ irrigated ablation was performed in a similar manner to PVAC ablation. Differences included use of a CARTO geometry created using the nMARQ catheter. The nMARQ catheter is not an over-the-wire system, and the nMARQ ablation system displayed live data from Tissue Connect, an impedence-based tissue contact algorithm, onto the CARTO geometry. nMARQ ablations were performed prior to changes in energy settings and algorithms were recommended. Hence the maximum bipolar power delivered was 25W. Otherwise, all other aspects of the procedure were similar to the PVAC ablation.
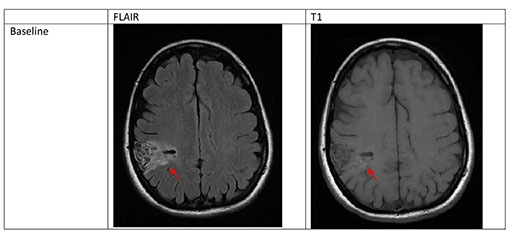
Figure 5. Silent cerebral event after PVAC ablation with residual white matter change at 3 months This patient (CHA2DS2Vasc score of 2) underwent PVAC ablation. A new SCE (asymptomatic DWI hyperintense, ADC hypointense lesion) is evident in the right frontal lobe. At 3 months, there is a FLAIR hyperintensity in the same region, consistent with cerebral white matter change (WMC)
Patients were all anticoagulated for at least 6 weeks prior to ablation, and stopped anticoagulants pre-procedurally without any bridging anticoagulation. Patients underwent general anaesthesia with double-lumen endobronchial intubation. Central venous and radial arterial access was routinely attained. A transoesophageal echocardiogram was performed after intubation but before surgery commenced. Thereafter, surgical ablation was performed as previously described.23 Briefly, PV isolation was achieved by epicardial ablation using a bipolar radiofrequency clamp (AtriCure Inc, Cincinnati, Ohio, USA). Empiric ganglionated plexi ablation, as well as an anterior right atrial line, posterior left atrial roof line and left atrial appendage excision or clipping was routinely performed. Oral anticoagulation was reinstated immediately after the procedure.
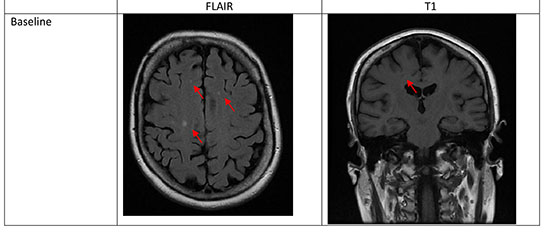
Figure 6. Pre-existing asymptomatic cerebral infarction This patient with CHA2DS2Vasc score of 1 underwent cerebral MRI prior to ablation. There was no prior history of cerebrovascular disease. This demonstrated several areas of white matter change (WMC), with one area of cerebral infarction (FLAIR hyperintense, T1 hypointense)
Data analysis was performed using SPSS statistical software (version 22, IBM Corp, New York, USA). Baseline characteristics of all randomised subjects were summarised. Categorical variables are reported as observed number of patients (percentage). A p-value of less than 0.05 was considered significant. Categorical variables were compared using the chi-squared test, ordinal data compared using the Kruskal-Wallis test, and continuous variables compared using ANOVA. Repeated measures were compared using the Wilcoxon signed-rank test.
54 patients were included in a per-protocol analysis of patients ablated with either PVAC, nMARQ, or surgical ablations. Baseline demographic data are displayed in Table 1. There were no significant differences between groups, including in their CHADS2 and CHA2DS2Vasc scores. No patients had congestive cardiac failure or prior documented stroke. Procedural factors relevant to the risk of periprocedural cerebrovascular events are shown in Table 2.
Table 1. Baseline demographics of per protocol study population. TIA: transient ischaemic attack; IQR: interquartile range. No patients had prior documented stroke or congestive cardiac failure
|
PVAC |
nMARQ |
Surgery |
Total |
| n |
21 |
19 |
14 |
54 |
| Mean age (years) |
66 |
67 |
62 |
65 |
| Gender (female) |
12 (57%)
|
13 (68%)
|
7 (50%)
|
32 (59%)
|
| Prior AF ablation |
3 (14%)
|
3 (16%)
|
2 (14%)
|
8 (15%)
|
| Prior TIA |
3 (14%)
|
0 (0%)
|
0 (0%)
|
3 (6%)
|
| Hypertension |
11 (52%)
|
11 (58%)
|
6 (43%)
|
28 (52%)
|
| Hyperlipidaemia |
7 (33%) |
5 (26%) |
4 (29%) |
16 (30%) |
| Coronary artery disease |
3 (14%)
|
4 (21%)
|
2 (14%)
|
9 (17%)
|
| Diabetes |
4 (19%) |
1 (5%) |
1 (7%) |
6 (11%) |
| Median CHA2DS2Vasc score (IQR) |
2 (1 to 3) |
3 (1 to 3.5) |
1 (1 to 2) |
2 (1 to 3) |
| Median CHADS2 score (IQR) |
1 (0 to 2) |
1 (0 to 1) |
0.5 (0 to 1) |
1 (0 to 1) |
Table 2. Procedural factors relevant to the risk of periprocedural embolic events. SD: Standard deviation; IQR: Interquartile range; NA: Not applicable
|
PVAC |
nMARQ |
Surgery |
Total |
| N |
21 |
19 |
14 |
54 |
| Mean procedure time in minutes (SD) |
87 (21) |
77 (23) |
284 (50) |
124 (87) |
| Preprocedural Warfarin (%) |
19 (90.5%) |
14 (73.7%) |
9 (64.3%) |
42 (77.8%) |
| Preprocedural Dabigatran (%) |
1 (4.8%) |
4 (21.1%) |
5 (35.7%) |
10 (18.5%) |
| Preprocedural Rivaroxaban (%) |
1 (4.8%) |
1 (5.3%) |
0 (0%) |
2 (3.7%) |
| Median days prior to procedure anticoagulant stopped (IQR) |
0 |
0 |
3 (2 to 4) |
|
| Mean preprocedural INR for patients on Warfarin (SD) |
2.3 (0.4) |
2.2 (0.3) |
NA |
|
| Mean heparin dose given (SD) |
9,632 units
(2,290) |
10,412 units
(2,293) |
NA |
|
| Mean ACT during procedure (SD) |
300 seconds
(56) |
313 seconds
(54) |
NA |
|
Blinded Assessment Of All Scans
The outcome of the first blinded assessment of all scans is displayed in Table 3. There was a high rate of prevalent cerebrovascular disease on the baseline MRIs, despite the fact that no patient had any prior history of clinical cerebrovascular accident. Similarly there was a high rate of prevalent DWI-positive acute lesions seen both on the baseline and 3-month post ablation scans. None of these lesions can be attributable to the AF ablations. Pre-existing SCEs were no more likely in the patients who had had prior AF ablation (p = 0.33).
Table 3.
| Baseline |
PVAC |
nMARQ |
Surgery |
Total |
p-value |
| N |
21 |
19 |
14 |
54 |
|
| CI |
4 (19.0%) |
5 (26.3%) |
0 (0.0%) |
9 (16.7%) |
0.12 |
| WMC |
18 (85.7%) |
16 (84.2%) |
14 (100.0%) |
48 (88.9%) |
0.31 |
| AL |
1 (4.8%) |
2 (10.5%) |
0 (0.0%) |
3 (5.6%) |
0.41 |
| Mean Fazekas score |
1.1 |
1.0 |
1.3 |
1.1 |
0.41 |
| After ablation |
PVAC |
nMARQ |
Surgery |
Total |
Total |
| N |
15 |
15 |
5 |
35 |
|
| CI |
1 |
3 |
1 |
5 |
0.54 |
| WMC |
13 (86.7%) |
13 (86.7%) |
4 (80.0%) |
30 (85.7%) |
0.93 |
| AL |
3 (20.0%) |
2 (13.3%) |
0 (0.0%) |
5 (0.0%) |
0.54 |
| Mean Fazekas score |
1.1 |
0.9 |
1.3 |
1.1 |
0.36 |
| 3 months post ablation |
PVAC |
nMARQ |
Surgery |
Total |
p-value |
| N |
21 |
19 |
14 |
54 |
|
| CI |
4 (19.0%) |
4 (21.1%) |
2 (14.3%) |
10 (18.5%) |
0.82 |
| WMC |
19 |
16 |
12 |
47 |
0.80 |
| AL |
1 (4.8%) |
1 (5.3%) |
0 (0.0%) |
2 (3.7%) |
0.70 |
| Mean Fazekas score |
1.2 |
1.0 |
1.2 |
1.1 |
0.68 |
Overall, there were no significant differences observed between the three ablation groups in the rate of CI, WMC or AL at any time point. However, only five patients who underwent surgical AF ablation were able to have MRI scans in the early post-ablation period. Whereas the median time from ablation to the post-ablation scan was 1 day for both the nMARQ and PVAC groups, the median delay to MRI scan for these five surgical patients was significantly longer (3 days, p=0.003).
Figure 7. A similar finding is evident in this patient, also with a CHA2DS2Vasc score of 1. A large pre-existing cerebral infarction is seen. The patient underwent further cerebral imaging after this study, and was reviewed by independent neuroradiologists and neurologists. They concurred that the patient had suffered a prior asymptomatic cerebrovascular accident
Blinded Comparison Of Baseline And 3 Month Post-Ablation Scans
The baseline and 3 month post-ablation scans were compared and examined for evidence of new CI or WMC. No new CI were reported at all, however 20% of patients showed evidence of progressive WMC disease (Table 4). The extent of the progression in WMC was not great. All progressive WMC lesions were reported in the cerebrum supplied by the anterior circulation. No patient had more than one de novo WMC lesion (maximum diameter 5mm) and one existing WMC which increased in size (from 3 to 5mm in length measured at maximal dimension). There was no significant difference seen in the rate of progressive WMC disease between the ablation methods.
Table 4. Outcome of analysis of MRIs in temporal sequence. AL: Acute lesion; SCE: Silent Cerebral Event
|
PVAC |
nMARQ |
Surgery |
Total |
p-value |
| N |
21 |
19 |
14 |
54 |
|
| Number with evidence of progressive white matter change at 3 month MRI (%) |
5
(24%) |
4
(21%) |
2
(14%) |
11
(14%) |
0.79 |
| Number of acute scans with AL evident (%) |
3 |
2 |
0 |
5 |
0.35 |
| Number of apparent ablation-related SCE reclassified as pre-existing on comparison with baseline scan |
1 |
1 |
0 |
2 |
0.69 |
| Number of ablation-related SCE |
2 (10%) |
1 (5%) |
0 (0%) |
3 |
0.48 (6%) |
Blinded Comparison Of All Scans In Temporal Sequence
Five scans where an AL had been reported on the acute scan were compared with the baseline and 3 month post ablation scans. Two of five (40%) scans with an apparent ablation-related SCE were shown to be pre-existing, i.e. the DWI hyperintense lesion was already apparent on the pre-ablation scan. In total, only three patients had new ALs when baseline and the acute scans were compared: two after PVAC ablation and one after nMARQ ablation. In the nMARQ case, there was a new 3mm AL detected in the right frontal lobe, with no residual MRI abnormality in the corresponding region at 3 months. In one of the PVAC cases, there were a total of three new ALs detected: one 18x2mm left cerebellar, one 4mm left frontal and one 3mm left occipital AL. All three ALs had completely resolved with no MRI abnormality at 3 months. However, in the remaining PVAC ablation, there was a new 5mm right frontal lobe AL, with a corresponding 3.5mm new WMC lesion at that site 3 months after the ablation. Selected images are presented in the Supplementary Appendix.
Overall, there was no significant difference in the rate of ablation-related SCE observed between the three types of AF ablation.
Overall, baseline cognitive function assessed by the MMSE and MoCA tests were normal across all three groups (Table 5). There were no significant differences between groups at before or after ablation. On repeated measures analysis, there were no significant changes seen in cognitive function test scores. At no point within study follow up was there any change in neurological status including any new clinical signs.
Table 5. Baseline and post-ablation cognitive function test results. MMSE: Mini Mental State Examination; MoCA: Montreal Cognitive Assessment; IQR: Interquartile range
|
PVAC |
nMARQ |
Surgery |
Total |
| Median baseline MMSE score (IQR) |
100%
(97 to 100%) |
100%
(97 to 100%) |
97%
(97 to 99%) |
97%
(97 to 100%) |
| Median post ablation MMSE score (IQR) |
98%
(98 to 100%) |
100%
(97 to 100%) |
98%
(95 to 100%) |
99%
(97 to 100%) |
| Median baseline MoCA score (IQR) |
93%
(87 to 97%) |
90%
(86 to 93%) |
87%
(84 to 93%) |
90%
(86 to 94%) |
| Median post ablation MoCA score (IQR) |
97%
(93 to 98%) |
93%
(88 to 97%) |
95%
(91 to 97%) |
94%
(90 to 97%) |
In this prospective randomised controlled trial of three different AF ablation techniques in paroxysmal AF, we performed serial cerebral MRI assessments up to 3 months post-ablation. The platinum-tipped PVAC catheter has previously been reported to have a very high rate of ACE, Non-randomised studies have suggested that with some procedural modifications, the apparent ACE rate can be reduced. Consequently the reported rate of PVAC-related ACE has varied between 39%16and 2%.7 The nMARQ ablation system has similarities to the PVAC system, but with the difference that all ablation electrodes are continuously irrigated. Non-randomised studies have suggested varying rates of ACE,20,26 but this is the first randomised study examining this technique. Finally, there are few published data describing minimally invasive thoracoscopic surgical AF ablation, an entirely epicardial procedure. This is the first study to ever report cerebral MRI changes associated with stand-alone surgical AF ablation.
Ablation-Related Silent Cerebral Events (SCE)
The main finding of this study was that in 54 patients undergoing different types of AF ablation, there were only 3 ablation-related SCEs detected. Overall, there were no significant differences seen in the rate of ablation-related SCE seen between the three ablation strategies. However, a major limitation of this study was that a number of patients, disproportionately those who underwent surgical ablation, did not receive an early MRI. No surgically ablated patient was found to have an ablation-related SCE, but it is possible that undetected SCE occurred in some patients who could not receive an early MRI scan. In practice, it proved very challenging to perform cerebral MRIs in patients recovering from surgical ablation. With improvements in post-operative recovery after surgical ablation, this may become feasible in the future.
Comparison of the PVAC and nMARQ patients showed that the ablation-related SCE rate was similar between the groups, and is within the range described in other studies.7-16 Although it is not possible to draw conclusions from such few events, we did observe a numerically higher number of ablation-related SCE in the PVAC group, and the only patient with an SCE which did not resolve at 3 months had had a PVAC ablation.
An unexpected finding was the high rate of background DWIhypertense acute lesions (AL) seen at baseline (5.1%) and at 3 months (3.3%), which has not been reported elsewhere. The study design meant that all ALs were reported without the potential bias of radiologists knowing the order in which scans were undertaken. This revealed a surprising number of SCEs which could not be related to any ablation. All patients were therapeutically anticoagulated throughout the study, and the median CHA2D¬S2-Vasc was only 2. The high background rate of asymptomatic lesions in this population raises further questions as to the clinical relevance of post-ablation SCE defined by DW-MRI signal abnormality.
High Background Prevalence Of MRI-Detected Cerebrovascular Disease
In addition to the unexpectedly high baseline rate of AL (5.1%), there was a high rate of established cerebral infarction (15.1%) and white matter change (90.0%). This is particularly remarkable given the low prevalence of clinical cerebrovascular disease, and the low CHA2D¬S2-Vasc scores. The patients within this study had a much higher rate of existing cerebral lesions than have ever been reported before in any other similar study.7,8,14,27 However, the overall burden of white matter change as indicated by the Fazekas score was appropriate to this age group. Given the highly selected nature of most studies examining the cerebral MRI effects of AF ablation, this study provides further insight into the prevalence of MRI abnormalities in typical AF ablation patients.
The effect of pre-existing MRI abnormalities on the detection rate for new lesions should be considered. It is feasible that embolism to vessels supplying already abnormal cerebral tissue may not result in radiographically detectable new MRI changes. There are little existing data validating the accuracy of DWI in detecting small new lesions in patients with established cerebral infarction or white matter change.
High Rate Of Progressive Cerebral MRI Change
The uncertain validity of DWI for detecting acute lesions in patients with pre-existing cerebral MRI abnormalities was a key reason we prospectively planned to compare baseline and 3 month scans for evidence of progressive disease. To our knowledge, this was the first study to use this methodology. As a consequence of this approach, all studied patients, even those who could not have an acute MRI, could be analysed.
Although there was no evidence of new ablation-related cerebral infarction, there was a high incidence of new cerebral white matter change. In the absence of a comparator group of patients who did not undergo ablation, it is not possible to know if the rate of progressive cerebral disease was higher or lower than expected for this population. However, at least one instance of progressive WMC was directly attributable to an ablation-related SCE, implying that the ablation procedures had at least a partial causal role in progressive cerebral MRI abnormality.
The methodology of comparing all pre-ablation to 3 month post-ablation scans was straightforward for patients and investigators. More new events were detected than with the DWI-based method, including several in patients who had apparently unchanged MRI appearances in the early post-ablation scans. The clinical significance of SCE and asymptomatic new WMC is not certain. However, most SCEs appear to completely resolve whilst new WMC appears to persist. It may be that progressive new WMC is a more clinically relevant MRI end-point than SCE.
Although the overall incidence of new chronic MRI changes was alarmingly high, the number and extent of progressive WMC was limited. Furthermore, it should be noted that no patient had any adverse clinical neurological event at any time and there was no evidence of any ablation-related cognitive deficit at any time. It is feasible that AF ablation may demonstrate protective effects on progressive cerebrovascular disease if assessed at other time-points than 3 months post ablation. At present, there are insufficient data to draw strong conclusions about the interaction between AF ablation and progressive cerebral MRI abnormalities.
The major limitation of this study is that a low number of patients undergoing surgical ablation were able to have an early post-ablation MRI. However, all patients had baseline and 3 month post ablation MRIs. The study was not powered to detect small differences in the rate of cerebral MRI abnormality. Nevertheless, the prospectively defined analysis plan maximised the use of the available data, and demonstrated several new hypothesis-generating findings. Furthermore, the overall event rates for new ablation-related SCE were consistent with other published studies.7-16
The boundaries used to define established cerebral infarction are consistent with the major published work in this field.28,29 However, the requirement for FLAIR hyperintensity meant that some cerebral infarctions (especially lacunar infarctions) were not counted within this scheme. Hence the prevalence of underlying silent cerebral infarction is likely to be underestimated. Nevertheless, the FLAIR criterion acted as an effective way of excluding incidental enhancing periventricular (Virchow-Robin) spaces.30 Furthermore, the aim of this study was to look for the presence of ablation-related cerebral infarction on the 3 month scan. FLAIR hyperintensity consistently occurs within hours of a cerebral infarction,31 and is known to persist for at least 3 months, supporting the use of a FLAIR criterion for detection of ablation-related events.
This study population had the highest rate of prevalent cerebral MRI abnormality so far reported. They, however, represent a clinically relevant group of patients. The overall rate of ablation-related SCE was consistent with other published data, but was overshadowed by a high background rate of SCE which was not ablation-related. The prevalence of spontaneous SCE in this population undermines the clinical significance of asymptomatic acute ablation-related cerebral MRI changes based on DWI.
When pre- and 3 month post-ablation MRIs were compared, 1 in 5 patients had detectable new cerebral white matter change. The volume and number of lesions were low, but the high incidence of these lesions within a short time-frame is alarming. There was no evidence that nMARQ, PVAC or surgical ablation resulted in a difference in the rate of progressive WMC, and no patients were found to have any adverse neurological sequelae or change in cognitive function at any time.