Atrial Fibrillation after Radiofrequency Ablation of Type I Atrial Flutter
Chan-Il Park, Pacale Gentil-Baron, Dipen Shah
Cardiology Service, Department of Medicine, University Hospital of Geneva, Geneva, Switzerland.
Typical atrial flutter (AFL) or type I AFL is the most common type of macroreentrant atrial tachycardia. Its prevalence increases with age and is more common in men. Ablation of the cavo-tricuspid isthmus (CTI), a critical part of the circuit, is safe and highly effective. Despite the long-term efficacy of this therapy, a significant proportion of patients undergoing CTI ablation will develop atrial fibrillation (AF) during the follow-up and identifying them can have an important impact on their management. PV isolation and typical flutter ablation during the same procedure may be an effective treatment strategy for patients with clinical documentation of both arrhythmias.
Key Words : Atrial Flutter, Atrial fibrillation, Radiofrequency Ablation.
Correspondence to: Prof. Dipen Shah Division of Cardiology Geneva University Hospitals 4, rue Gabrielle-Perret-Gentil 1211 Geneva 14 Switzerland
Typical or common atrial flutter (AFL) is the most common type of macroreentrant atrial tachycardia. Its prevalence increases with age and is 2.5 times more common in men.1 Typical AFL results from re-entrant activation in the right atrium (RA) around the tricuspid valve annulus and catheter ablation of the cavo-tricuspid isthmus (CVI) – a critical part of the circuit - is a well-established first-line therapy.2-8 This intervention is safe and highly effective with single procedure efficacy evaluated to be near 95%.9-10
Despite the long-term efficacy of this therapy, a significant proportion of patients4,11-13 will develop atrial fibrillation (AF) during the follow-up. Identifying the patients at risk to develop AF after typical AFL catheter ablation is important, because it will influence their subsequent medical management (e.g. pursuing anticoagulation and/or antiarrhythmics) and they can be informed of the risk of recurrent symptoms and related prognostic implications.
The aim of this report is to review the inter-relationship between typical AFL and AF; the clinical predictors associated with occurence of AF after typical AFL ablation and finally, outline an approach to management of these patients.
The Inter-Relationships of Typical AFL and AF
Typical AFL and AF are both atrial arrhythmias and they frequently coexist in the same patient. Despite the substrate of AF and typical AFL being different in terms of location [(AFL – right atrium (RA) / AF – left atrium (LA)], some observations suggest a mechanistic interaction between them, especially during the initiation of arrhythmia.
Experimental studies in the sterile pericarditis model demonstrated that typical AFL starts preferentially with brief episodes of AF.14 This was also recognized in humans after open heart surgery15 or in patients when AFL was induced in the electrophysiology laboratory16
In experimental studies, the conversion from AF to typical AFL occurred when a functional line of block was created in the RA free wall, between the two vena cava, along the crista terminalis.17-18 The length and location of this line of block, with the presence of areas of slow conduction in the RA, was the key to convert AF to sustained typical AFL.
This conversion was analyzed in patients referred for typical AFL ablation.19 Despite the absence of LA endocardial activation recordings, a characteristic sequence of events was observed in the RA just before the conversion. An organized activation or ¨organized AF¨ along the trabeculated RA was observed, which was preceded and followed by an electrical silent period, a necessary event for conversion to typical AFL. This sequence of activation could be favoured in patients with remodeled RA with pre-existing but incomplete (anisotropic or structural scar-related) intercaval zone of block.
Therefore, one hypothetical scenario may be that short episodes of AF - initiated by rapid firing ectopic foci predominantly of LA origin20- create a functional complete intercaval zone of block in patients with a RA substrate - and a period of LA quiescence or slowing favours the occurence of AFL (see figure 1).
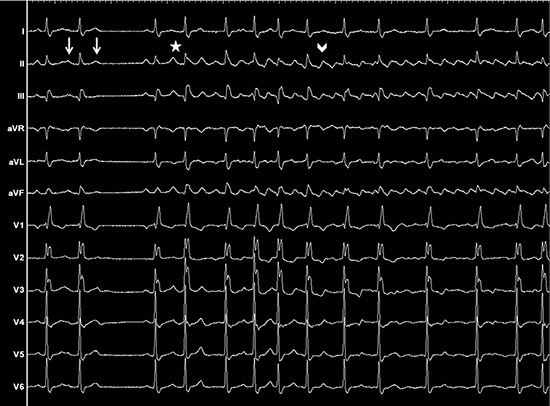
Figure 1. 12-leads ECG from a 77 year-old male with palpitations and without structural heart disease, showing the spontaneous onset of typical atrial flutter. Left : sinus rhythm interrupted by two atrial premature beats (white arrows), one conducted and one blocked. Middle: rapidly firing ectopic foci (white star) arising from the left superior pulmonary vein, inducing a short transitional rhythm corresponding to atrial fibrillation. Right: onset of typical couterclockwise atrial flutter (white arrowhead).
Predictors of AF after Ablation of Typical AFLs
As mentioned earlier, a significant proportion of patients, with successfully ablated typical AFL, will develop subsequent AF. Identifying these patients can have important therapeutical implications, especially in terms of anticoagulation therapy.
There are different clinical predictors associated with the occurence of AF:
Prior history of AF (most significant predictor)
Presence of structural heart disease, especially LA dilatation and/or left ventricular dysfunction11
Sustained AF inducibility after AFL ablation4,21
Patients with prior history of AF and/or structural heart disease or those developing typical AFL under Ic antiarrhythmics,12 are at the greatest risk to develop subsequent AF. In a meta-analysis performed by Péres et al.22 52.5% patients with prior history of AF and 47.7% patients with AFL under Ic antiarrhythmics developped AF during an average follow-up of 15 months. Since CTI ablation may prevent only the conversion from AF to AFL and has no effect to the underlying tendency toward fibrillation (PV triggers or LA substrate), it is not surprising that all these patients may develop AF despite successful CTI ablation.
More importantly, even in the subgroup of patient without prior history of AF, the incidence of subsequent AF remains high when the follow-up was long enough; in the meta-analysis cited earlier22 the occurence of AF continues to rise until reaching the same incidence rate after 5 years of follow-up than patients with prior history of AF. Ellis K. et al10 observed also in this subgroup of patient, 82% of subsequent AF during a follow-up of nearly 4 years. The persistent risk of AF, even in those patients without the clinical predictors, suggests a potentially important role of AF as a trigger rather than a consequence of typical AFL.
In other words, occurence of AF after typical AFL ablation is relatively common and depends mostly on the duration and intensity of the follow-up. The time of appearance of AF seems to be determined by the presence of underlying electrophysiological and structural substrate in the atria. Patients with a prior history of AF and/or structural heart disease (e.g. LA dilatation, left ventricular dysfunction) will be at risk to develop AF after CTI ablation more earlier than patients with lone AFL, reflecting only a more advanced electrical LA disease in the former patients.
In our center, we retrospectively analyzed patients who had AF ablation therapy between 2002-2011. From a total of 762 patients (68% paroxysmal AF, 32% persistent AF) 7% (51/762) had a previous CTI ablation. Of these 51 patients (35 paroxysmal AF, 16 persistent AF), 65% (33/51) had a prior AF history before developing typical AFL, 31% (16/51) had a left ventricular dysfunction at the time of intervention. Despite the limitations associated with this retrospective analysis, our findings confirm that two-thirds of patients, who develop subsequent AF after CTI ablation, had a prior history of AF.
Clinical and Therapeutical Implications
It is well accepted that ablation of typical AFL is recommended as part of an AF ablation therapy, if documented prior to the intervention or occurring during AF ablation.23,24 Conversely, in patients without any prior or induced typical AFL, prophylactic CTI ablation does not provide clinical benefit in terms of AFL incidence25 and could potentially result in procedure-related complications.
In patients presenting primarily with typical AFL, with or without AF, CTI ablation with the endpoint of a bidirectional block by differential pacing26 must be performed. In the subgroup with sustained typical AFL induced by rapid firing ectopic beats (figure 1) ablation of the firing sites combined with CTI block may be necessary, both for symptom alleviation and for the prevention of AF development.
In the subset of patient with AF developing typical AFL under Ic AAD, it was recently demonstrated that an hybrid therapy (ablation of CTI followed by administration of AAD) was not effective as a long-term therapy, with 90% of patients presenting AF recurrence during a follow-up of 5 years.27 These patients can be initially managed with AAD but they must be informed that pulmonary vein isolation (PVI) would be necessary for a better long-term rhythm control.
Because AFL and AF are two inter-related arrhythmia and the majority of patients who get a CTI ablation will develop AF. In patients with coexistence of AF and AFL, PVI combined with CTI ablation should be performed as a first-line therapy. This strategy was recently demonstrated to be beneficial in terms of AF recurrence and quality of life.28 In our center as well, PVI and typical flutter ablation are performed during the same procedure in case of clinical documentation of symptomatic AF and typical flutter.
In terms of surveillance, all CTI ablated patients are advised to perform an arrhythmia follow-up with Holter monitoring at 1 and 3 months followed by 3 to 6 monthly visits to their referring physicians. For patients with lone typical AFL who have no recurrence of arrhythmia, anticoagulation therapy is usually stopped at 3 months.
After CTI ablation, all the patients must be advised of the possibility of recurrent palpitations and require close follow-up. There is no clear strategy concerning the surveillance and the medical management of patients after typical AFL ablation. Continuation of anticoagulation and/or AAD therapy should be chosen on a per patient basis, as well as the choice of performing PVI for those developing clinically significant AF.
Despite the long-term efficacy of CTI ablation for typical AFL, a significant proportion of patients, especially those with prior history of AF and/or structural heart disease, will develop subsequent AF. These patients must be informed about the risk of developing palpitations and other arrhythmia. After successful CTI ablation, close outpatient follow-up with frequent ECG - Holter monitoring must be performed. For the moment on, the pursuit of antiocoagulation and/or antiarrhythmic therapy must be decided in an individual basis, as well as the requirement and timing of AF ablation.