Gender and Racial Characteristics of Patients
Referred to a Tertiary Atrial Fibrillation Center
Pamela K. Mason, MD1, Liza Moorman, RN, ACNP-BC1, Douglas E. Lake, PhD1, J. Michael Mangrum, MD1, John P. DiMarco, MD, PhD1, John D. Ferguson, MBChB, MD1, Srijoy Mahapatra, MD1, Kenneth C. Bilchick, MD1, David Wiggins, BS, RN1, J. Paul Mounsey, MD, PhD2, J. Randall Moorman, MD1
1University of Virginia Health System.2bUniversity of North Carolina.
Atrial Fibrillation Centers (AFCs) are becoming increasingly common and are often developed at institutions to provide comprehensive evaluation and management for patients with atrial fibrillation (AF) including catheter and surgical ablation. Studies have shown that women and racial minority patients are less likely to be offered aggressive or invasive therapies. The University of Virginia (UVA) AFC was opened in 2004. We analyzed data collected during initial visits to our AFC from 2004-2008 to determine the gender and racial characteristics of a tertiary AFC population. Multivariable regression analysis was used to compare clinical characteristics. There were a total of 1664 consecutive initial patient visits. Cardiologists referred 61% and primary care physicians referred 37% of patients. Twice as many men were referred as women (570 vs. 1094; P<0.0001). Women were older (68.0±11.9 vs. 62.4±13.0 years; P<0.0001) and more symptomatic with palpitations (80% vs. 73%; P=0.008), but otherwise were not substantially different from men. Our referring physicians treated the majority of both men and women with anticoagulant and rate-controlling medications. African American patients accounted for 2.8% of AFC initial visits. In contrast, they accounted for 7.4% of patients seen for a primary diagnosis of AF at all other UVA outpatient clinics (P<0.0001). In conclusion, the demographics of a tertiary AFC are different than those of the general population. Women and racial minority patients are underrepresented, and the women have few comorbidities and symptoms than the known epidemiology would lead us to expect.
Correspondence to: Pamela K. Mason, Box 800158, University of Virginia Health System, Charlottesville, VA 22908.
Atrial fibrillation (AF) has reached epidemic proportions in the United States. There are 2.5-3 million Americans with AF currently and it is estimated that this number will more than double by the year 2050.1-3 AF is a major health problem, leading to reductions in quality of life. It is associated with a significant stroke risk and increased mortality.4,5 AF is one of the leading hospital discharge diagnoses and costs the health care system more than $6 billion annually.6
There are known gender and racial differences in the epidemiology of AF. While the incidence of AF is higher in men than women, the prevalence is the same due to increased longevity in women. Compared to men, women with AF are older and have more symptoms, comorbidities, and strokes.7-14 Data for racial and ethnic minorities with AF are lacking, but available evidence suggests that the prevalence of AF is less in African Americans.15,16
Studies show that women and minority patients are less likely to be offered aggressive therapies or included in research trials17-19 This limits our knowledge with regards to the best AF treatments for these groups of patients.
The University of Virginia (UVA) Atrial Fibrillation Center (AFC) was opened in 2004. Our AFC offers a comprehensive menu of medical and ablative therapies. We accept referrals from primary care physicians and general cardiologists, and in many cases, patients are being referred for more aggressive or ablative therapy. The purpose of this study was to describe the gender and racial characteristics of the patients that have been referred to our tertiary AFC.
The UVA AFC opened on 10/31/2004 and is staffed by nurse clinicians, nurse practitioners, physician assistants and adult electrophysiologists with appropriate support staff. We analyzed data from 1664 consecutive initial visits ending on 4/31/2008. For each initial visit a detailed database, designed according to AHA/ACC guidelines, was created using patient history and medical records.20 The data collected included demographic information, date of initial diagnosis of AF, comorbid conditions, types of symptoms, dates of symptomatic recurrences, and all previous cardiac studies and therapies. Comparative demographic information for Virginia and the United States was obtained from the United States Census Bureau.21 This study was approved by the Institutional Review Board of the University of Virginia.
Paroxysmal and Persistent AF
Paroxysmal AF was defined as a self-limited episode that typically lasted less than 48 hours and spontaneously converted. Persistent AF was defined as an episode lasting more than 48 hours or required cardioversion. The term permanent AF was not used as it had not yet been determined if the patient was a rhythm control failure.
The AF Symptom Duration Score. For each patient, an AF Symptom Duration Score was used as an estimate of AF burden:
This represents the proportion of the year spent in symptomatic AF.
This was defined as any bleeding event that required hospitalization or blood transfusion.
Continuous variables are expressed as mean ± standard deviation, and the significance of differences was tested using the t-test. Categorical variables are expressed as numbers and percentages, and the significance of differences was tested using the Z-test. We used multivariable logistic regression to test the significance of differences in clinical characteristics of groups Table 1. Model 1 tested the association of gender with individual symptoms, comorbidities and drugs. Model 2 tested the association of gender with major comorbidities and any antiarrhythmic drug, any rate-controlling drug, and any anti-thrombotic drug. The differences between the AF Symptom Duration Score were tested using the rank sum test.
Table 1. Clinical Characteristics of the University of Virginia Atrial Fibrillation Center Population
|
All Patients (1664) n (%) |
Female (570) n (%) |
Male (1094) n (%) |
P value |
| Paroxysmal AF |
1023 (62) |
389 (68) |
634 (58) |
<0.0001 |
| Symptoms |
1485 (89) |
524 (92) |
961 (88) |
0.02 |
| Palpitations |
1253 (76) |
456 (80) |
797 (73) |
0.008 |
| Syncope |
35 (2.1) |
18 (3.2) |
17 (1.6) |
0.10 |
| Pre-syncope |
321 (19) |
129 (23) |
192 (18) |
.07 |
| Dyspnea |
686 (41) |
252 (44) |
434 (40) |
0.14 |
| Chest Pain |
144 (8.7) |
54 (9.5) |
90 (8.2) |
0.52 |
| Fatigue |
597 (36) |
210 (37) |
387 (35) |
0.70 |
| Comorbidities |
|
|
|
|
| Diabetes Mellitus |
217 (13) |
79 (14) |
138 (13) |
0.55 |
| Hypertension |
931 (56) |
334 (59) |
597 (55) |
1.0 |
| Coronary Artery Disease |
249 (15) |
72 (13) |
177 (16) |
<0.0001 |
| Heart Failure |
156 (9.4) |
62 (11) |
94 (8.6) |
0.03 |
| Chronic Kidney Disease |
54 (3.2) |
17 (3.0) |
37 (3.4) |
0.44 |
| Stroke/TIA |
114 (6.9) |
35 (6.1) |
79 (5.0) |
0.05 |
| Antiarrhythmic Drug |
559 (34) |
199 (35) |
360 (33) |
0.30 |
| Amiodarone |
159 (9.6) |
54 (9.5) |
105 (9.6) |
0.54 |
| Flecainide |
141 (8.5) |
55 (9.6) |
86 (7.9) |
0.10 |
| Propafenone |
58 (3.5) |
20 (3.5) |
38 (3.5) |
0.84 |
| Dofetilide |
55 (3.3) |
17 (3.0) |
38 (3.5) |
0.66 |
| Sotalol |
149 (9.0) |
55 (9.6) |
94 (8.6) |
0.30 |
| Disopyramide |
12 (0.7) |
5 (0.9) |
7 (0.6) |
0.66 |
| Rate Controlling Drug |
1090 (66) |
400 (70) |
690 (63) |
<0.0001 |
| Beta Blocker |
818 (49) |
297 (52) |
521 (48) |
0.02 |
| CCB |
328 (20) |
124 (22) |
204 (19) |
0.03 |
| Digoxin |
215 (13) |
91 (16) |
124 (11) |
0.03 |
| Antithrombotic Drug |
1360 (82) |
458 (80) |
902 (82) |
0.33 |
| Aspirin |
495 (30) |
151 (27) |
344 (31) |
0.01 |
| Coumadin |
971 (58) |
337 (59) |
634 (58) |
0.14 |
AF- atrial fibrillation; TIA- transient ischemic attack; CCB- calcium channel blocker
Primary care physicians referred 37% of the patients, cardiologists referred 61% of patients, and other specialists referred 2% of the patients. Referrals from within the UVA Health System accounted for 19% of the patients. Of the total AFC population, 40% are sent from within our primary referral area and an additional 26% are sent from our secondary referral area. Overall, 91% of patients were referred from within Virginia and 9% were referred from out-of-state. The average duration of AF was 5.2 years at the time of referral. A significant number of patients, 41%, had been diagnosed with AF for less than 2 years at the time of referral. At the other extreme, 11% had carried the diagnosis for more than 12 years Figure 1.
Figure 1. Duration of Atrial Fibrillation Diagnosis in the UVA AFC Population
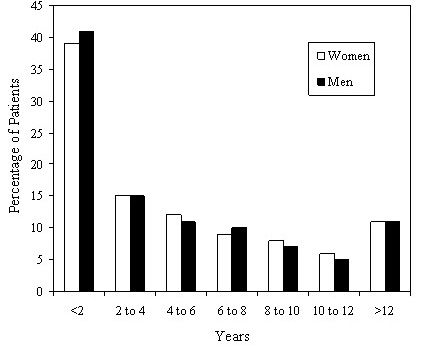
Males numbered 1094 (66%) and females numbered 570 (34%). The baseline characteristics are shown in Table 1. The mean ages for women at diagnosis and referral were 62.7±13.6 and 68.0±11.9 years, respectively, and the mean ages for men at diagnosis and referral were 57.3±14.0 and 62.4±13.0 years (P<0.0001 for each). There was no difference in the length of time from diagnosis to initial visit at the AFC between men and women. The age distribution of the patients at referral is seen in Figure 2.
Figure 2. Age Distribution of Men and Women at the Time of Referral to the UVA AFC
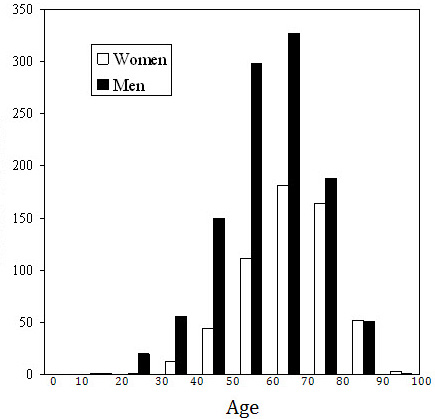
Women were more likely to have PAF (68% vs. 58%; P<0.0001) and described more symptoms, particularly palpitations (80% vs. 73%; P=0.008). However, the AF Symptom Duration Scores were slightly higher in men (0.31±0.40; median 0.23) than women (0.25±0.36; P=0.0002; median 0.04). There were no differences in comorbidities, with the exception of coronary artery disease (CAD) and heart failure (HF). Women were less likely to have CAD (P<0.0001), but were slightly more likely to have HF (P=0.031). Women also had slightly higher CHADS2 Scores (1.03 vs. 0.88; P=0.002). The distribution of CHADS2 scores for men and women are seen in Figure 3.
Figure 3. Distribution of CHADS2 Scores in the UVA AFC Population
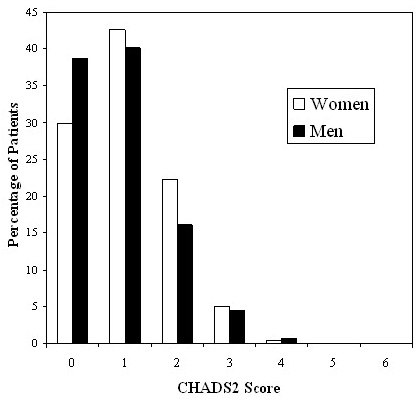
Women were less likely to have received a cardioversion prior to referral to the AFC (23% vs. 32%; P<0.0001). Our referring physicians treated the majority of men and women with antithrombotic medications. Aspirin was used in 27% of women and 31% of men (P=0.014). Warfarin was used in 59% of women and 58% of men (P=0.138). Women and men were equally as likely to have been treated with antiarrhythmic medications (P=0.302). However, only 34% of all patients received any antiarrhythmic drug prior to referral to the AFC and the average number of drugs attempted per patient was 0.35. Women were more likely to have received rate-controlling medications prior to referral (70% vs. 63%; P<0.0001), and this included beta blockers, calcium channel blockers, and digoxin.
Racial and Ethnic Differences
Few racial and ethnic minority patients were referred to the AFC. The racial and ethnic demographics of the AFC patient population as well as all outpatients seen by any UVA physician with a primary diagnosis of AF are shown in Table 2. The racial and ethnic demographics of our primary and secondary referral areas in central Virginia, the state of Virginia, and the United States are also shown in Table 2 for comparison. The proportion of outpatients at our AFC who were African-American was much less than that seen at the other UVA outpatient clinics for a primary diagnosis of AF (2.8% vs. 7.4%; P<0.0001). Moreover, the number of African-American patients referred to our AFC was less than expected based on the demographic data. Whites outnumber African-Americans by 7-fold (83% compared to 12%) in our referral areas, but white referrals are more than 30-fold more common (93% of our AFC practice compared to 2.8%). Some of this difference is due to the lower prevalence of AF in African-Americans, but some may well be due to referral bias.
Table 2. Racial Characteristics of the UVA AFC Population
|
AFC Population (%) |
UVA AF Population* (%) |
Primary Referral Area (%) |
Primary and Secondary Referral Area (%) |
State of Virginia (%) |
United States (%) |
| White, not of Hispanic origin |
93 |
89 |
83 |
83 |
67 |
66 |
| Black |
2.8 |
7.4 |
12 |
12 |
20 |
13 |
| Asian |
0.3 |
0.5 |
0.2 |
0.8 |
4.9 |
4.5 |
| Hispanic |
0.2 |
0.1 |
2.6 |
2.7 |
6.8 |
15 |
| Other, including mixed race |
1.6 |
2.6 |
1.3 |
1.2 |
1.7 |
1.7 |
*Patients seen as outpatients in any clinic at UVA with a primary diagnosis of AF. UVA- University of Virginia; AFC-Atrial Fibrillation Center
In this study, we have defined the population of a tertiary AFC, which is quite different from the population demographics of AF in the United States.7-16 In the United States, studies have shown that the incidence of AF in men is 1.5 times that of women. However, women have greater longevity, and ultimately the prevalence of AF in men and women is the same. It has also been shown that women are more likely to have PAF and their episodes are more frequent and faster. Women have higher symptom burdens and lower quality of life scores. Associated with AF, women have more comorbities and strokes. Fewer studies have evaluated AF in racial and ethnic minorities in the United States, but the prevalence of AF in African Americans is thought to be about half that of whites.17-19
In our AFC population, twice as many men were referred as women. The women were older and more likely to have PAF than the men, but otherwise the two populations were relatively similar. The women had fewer comorbidities and symptoms than the known epidemiology would lead us to expect. This suggests that women with comorbid conditions are not being referred for tertiary care. African Americans and other minority were dramatically less likely to be referred to our tertiary AF center, even when taking into consideration the expected lower prevalence in this population.
Determining why women and racial minorities are referred less often to our AFC is beyond the scope of this study and is likely multifactorial. Similar findings have been seen in other studies.22,23 AFCs tend to serve AF patients who are difficult to manage or who are viewed as being ablation candidates by referring physicians. The data regarding catheter ablation outcomes and complications for AF in women is conflicting, and there is virtually no data for African American patients.24-25 Our referring physicians may view women and racial minority patients as poor candidates for more invasive therapies. In addition, gender and racial disparity have been well described within the field of cardiology. It has been shown that women and African Americans are less likely to be offered aggressive therapies, including cardiac catheterizations and implantable cardioverter-defibrillators.17-19 There are also data to suggest that women are more cautious about undergoing elective procedures compared to men.26-27
One of the most encouraging findings of this study is the aggressive usage of antithrombotic medications in both men and women by our referring physicians, which includes a large proportion of primary care physicians as well as general cardiologists. Over 80% of all patients were receiving aspirin or warfarin at the time of referral to the AFC. Patients were also being aggressively treated with rate-controlling medications, with women being more likely to receive these medications. This may reflect the increased burden of palpitations that the women experienced. Only a third of the patients had ever received any antiarrhythmic therapy prior to referral to our specialized AFC. Studies have demonstrated that women have increased side effects to antiarrhythmic medications over men.7,11,12 However, there were no differences in antiarrhythmic usage between men and women in our patients.
This study is limited as a retrospective review. While our referral area is large, it is still geographically limited and the ability to extrapolate this data to other tertiary AFC centers is unknown. However, we have demonstrated that there are differences in the ways that women and racial minorities with AF are managed. Physiologic differences do occur between different groups of patients; however, determining what those differences are can be difficult due to the disparity in medical care and research. This study highlights the need for further investigation regarding the epidemiology and management of AF in women and racial minorities.