4D Volume Intracardiac Echocardiography for Intraprocedural Guidance of Transcatheter Left Atrial Appendage Closure
Houman Khalili1, Marquand Patton 1, Haider Al Taii2, Priya Bansal2, Matthew Brady3, Jeanellil Taylor3, Arati Gurung3, Brijeshwar Maini12
1Tenet Healthcare Corporation, Delray Beach, FL .2Charles E. Schmidt College of Medicine, Florida Atlantic University, Boca Raton, FL.3Siemens Healthineers, Malvern, PA.
Fluoroscopy and transesophageal echocardiography (TEE) are used to guide transcatheter left atrial appendage (LAA) closure in patients with atrial fibrillation to prevent thromboembolic events. This study examines whether real-time three-dimensional volume ICE guidance (4D volume ICE) can be used as an alternative to TEE during LAA closure (LAAC).
Fifteen patients with atrial fibrillation (AF), who had high risk for stroke and contraindication for long-term warfarin therapy, were enrolled in the study. The WATCHMAN device was used for transcatheter LAAC under fluoroscopy. LAA and device sizing was performed using TEE and volume ICE guidance from the right heart. Intraprocedural ICE measurements were consistent with TEE; LAA maximal width and depth, and maximal diameter of the implanted device were moderately correlated (Pearson's coefficient: 0.63, 0.65, and 0.71 respectively; p<0.05) with good agreement (bias: -0.03 cm, -0.07 cm, and 0.003 cm respectively). The average imaging success rate, defined by the number of patients with all the required intraprocedural measurements, was 67% for ICE and 100% for TEE. The WATCHMAN device was successfully implanted in all patients with a device to patient ratio of 1.33.
4D volume ICE can be used as an intraprocedural sizing and guidance tool for transcatheter LAAC with measurements comparable to TEE. Challenging patient characteristics significantly degrade the diagnostic image quality when imaging from the right heart. Standardized workflow with proper patient selection and optimal preprocedural planning may improve the diagnostic quality of volume ICE guidance for transcatheter LAAC procedure.
Key Words : LAA Closure, WATCHMAN, TEE, ICE.
Correspondence to: Brijeshwar Maini, MD, FACC
Clinical Professor of Medicine, Florida Atlantic University
Regional Medical Director of Transcatheter Therapies
Tenet Healthcare Corporation
4205 W. Atlantic Ave, Suite 201B
Delray Beach, FL 33445
Standard intraprocedural guidance for transcatheter left atrial appendage closure (LAAC) employs a multi-modality integrated approach combining fluoroscopy for guiding the delivery system, and transesophageal echocardiography (TEE) for intracardiac characterization to guide device selection and monitor procedural complications [1-6]. Successful implantation of the device is confirmed with contrast-enhanced fluoroscopy and color Doppler flow imaging on TEE. TEE is the current gold standard for procedural guidance but requires general endotracheal anesthesia (GETA) to avoid patient motion and discomfort during the procedure [6]. General anesthesia, however, is associated with pulmonary complications and patient discomfort due to endotracheal intubation [7,8]. Intraprocedural LAAC guidance under local anesthesia or conscious sedation might help mitigate these GETA-related disadvantages and has motivated multiple clinical studies, including a systematic review [9] and a meta-analysis [10], which have established intracardiac echocardiography (ICE) as a safe and feasible alternative to TEE [4,7,8,11-20].
ICE guidance for LAAC can be provided by placing the catheter, introduced via a femoral venous access, either in the right atrium [11,12,14-16], the right ventricular outflow tract [14], coronary sinus [15], or the left atrium [13,16-20]. Comparatively superior image quality and thus diagnostically optimal guidance for LAAC procedure are obtained with the left atrial ICE approach. This however requires a transseptal access to advance the catheter from the right atrium into the left atrium, either via the same transseptal puncture used for device delivery [17,18] or via a second puncture [8,13]. The residual transseptal shunt is shown to be clinically acceptable for ICE guidance when using 8Fr or 10Fr catheters. While the 2D ICE can provide adequate intraprocedural guidance, the real-time three-dimensional (3D) volume ICE (i.e. 4D volume ICE) can improve characterization of the LAA anatomy and its complex 3D morphology compared to 2D ICE [21,22]. The volumetric acquisition in real-time and in 3D allows the 4D volume ICE technology to reduce the need to acquire images from different anatomical locations wherein the coronal plane allows planar assessment of the LAA anatomy, facilitates spatial orientation, and provides circumferential peri-valvular as well as peri-device flow assessment using Color Doppler.
The primary drawback of the previous generation of 4D ICE was a smaller field of view with limited echo views. The new generation of 4D volume ICE offers a larger imaging volume of 90° x 50° with multiplanar reformatted (MPR) echo views for anatomical landmarks and procedural guidance including sizing (see Supplemental Video 1). We hypothesize that the additional MPR echo views and the anatomical landmarks from the larger imaging volume provide optimal LAAC intraprocedural guidance similar to TEE. This study reports our early clinical experience of using the enhanced 4D volume ICE system (Siemens, Mountain View, CA) for intraprocedural imaging guidance of LAAC with WATCHMANTM (Boston Scientific, Natick, MA), and examines the performance of right sided ICE for LAAC guidance in comparison to TEE.
Patients with permanent or paroxysmal atrial fibrillation, CHADS2-VASc > 2, and contraindication to long-term warfarin therapy were recruited for study participation. Pre-procedural TEE assessment was performed one week to a month prior to the procedure date to rule out the presence of intracardiac thrombus and to assess the dimensions and morphology of the LAA for transcatheter LAAC suitability; patients with LAA thrombus or pericardial effusion were excluded. Participants provided written informed consent prior to enrollment. The study was approved by the institutional review board (DEL16036). Patients were evaluated for the presence of pericardial effusion and thrombus using both TEE and ICE prior to the procedure.
WATCHMAN System and Protocol
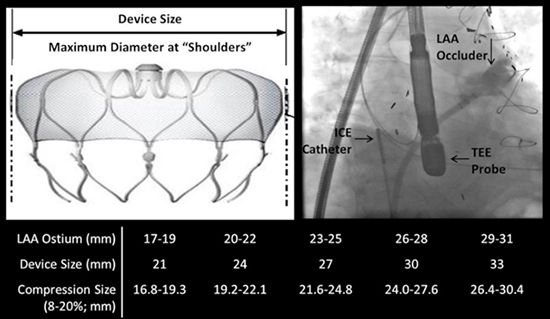
The WATCHMAN system consists of a delivery sheath with a pre-packaged occluder. The occluder size was selected based on the maximal diameter of the LAA orifice following the manufacturer guidelines, and using the maximal length of the LAA measured on Echocardiogram [Figure 1]. Intraprocedural measurements of the LAA width and depth were acquired on both ICE and TEE per protocol. Both ICE and TEE were used to assess for any procedural complications prior to insertion of the device delivery sheath. Under fluoroscopy and echocardiography, a Baylis wire and the device delivery sheath were introduced through the right femoral vein for transseptal puncture. The delivery sheath was subsequently placed into the LAA and the device was deployed after "the tug test" under both ICE and TEE. Success of the WATCHMAN implantation was evaluated via imaging measurements of the device diameter for proper positioning and compression, and color Doppler flow assessment for any peri-WATCHMAN leak. The WATCHMAN occluder was released after confirmation of a successful implantation or removed and replaced with a corrected size until a successful implantation was confirmed. The device per patient ratio was thus calculated as the total number of WATCHMAN selected divided by the total number of WATCHMAN successfully implanted. The manufacturer clinical specialist was present for each of the LAAC procedure.
Figure 1. Device selection criteria for LAA closure. The physical device size is defined as the maximum "shoulder-to-shoulder" diameter of the device and is selected using the manufacturer's guidelines based on the LAA ostium width measured on TEE, ICE or angiogram (left illustration with permission from Boston Scientific). Post deployment, adequate compression of the device is measured.
Intraprocedural Imaging Guidance
Intraprocedural LAAC guidance was provided simultaneously with ICE and TEE via 2D and 4D visualization, 2D and 3D measurements, and color Doppler flow imaging. TEE was performed under general anesthesia using the Z6M transesophageal transducer probe connected to an echocardiogram. ICE was performed by introducing a 12.5Fr ACUSON AcuNav Volume™ ICE catheter into the left femoral vein via a 14Fr delivery sheath and advanced into the right atrium via the inferior vena cava [Figure 2A]. The entire procedure was performed by placing the ICE catheter in the right side of the heart; the ICE catheter was placed in the right atrium and advanced into the right ventricle (RV) or the right ventricular outflow tract (RVOT) in patients where image quality was degraded due to challenging characteristics such as enlargement of the atrial chambers or the inter-atrial septum. The sterile ICE catheter was connected to a second echocardiogram via a SwiftLinkTM adaptor. The intraprocedural ICE workflow constituted acquisition of a reference frame, known as the "home view" wherein the right atrium, the tricuspid valve, and the right ventricle are visualized for reference [Figure 2B]. The inferior and the posterior portion of the interatrial septum were visualized for transseptal puncture guidance ([Figure 2C] and Supplemental Video 2) followed by left atrial characterization including the LAA sizing for device selection [Figure 1]. Lastly, the selected device was deployed into the LAA followed by a tug test to ensure proper positioning and compression, under contrast-enhanced fluoroscopy before releasing the device [Figure 2D].
Figure 2A. LAAC workflow illustration using 4D Volume ICE guidance. The ICE catheter is introduced via a femoral venous access into the right atrium (RA). Under echo guidance, a Baylis wire is used for interatrial transseptal puncture for delivery of the occluder device into the LAA under fluoroscopy (right illustration with permission from Boston Scientific).
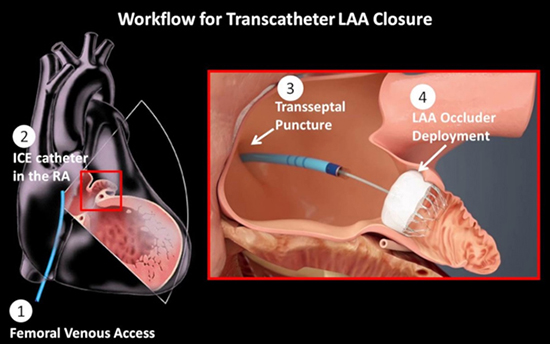
Figure 2B Home View. With the ICE catheter positioned in the right atrium, the anatomical landmarks are visualized to establish spatial orientation (see Supplemental Video 1): a Home View consists of the right atrium (RA), the tricuspid valve (TV), and the right ventricle (RV). The catheter probe is swept to assess for any contraindications in this view and orthogonal multiplanar reformatted (MPR) planes.
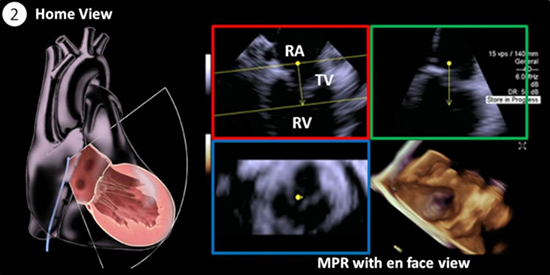
Figure 2C. Transseptal Puncture. ICE from the right heart is used to visualize the interatrial septum (IAS) to guide the Baylis wire for a transseptal puncture. 4D ICE MPR and en face views can be used for TSP guidance (see Supplemental Video 2).
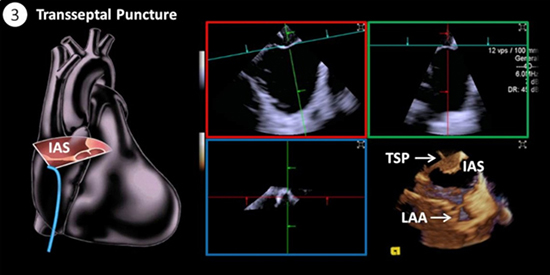
Figure 2D. Device Deployment. Under fluoroscopy, the WATCHMAN LAA occluder device is deployed via a delivery sheath which can be visualized under ICE (See Supplemental Video 3) and TEE. The compression measurement of the occluder is taken on multiple views to determine adequate device positioning and seal following the manufacturer's guidelines for device release.
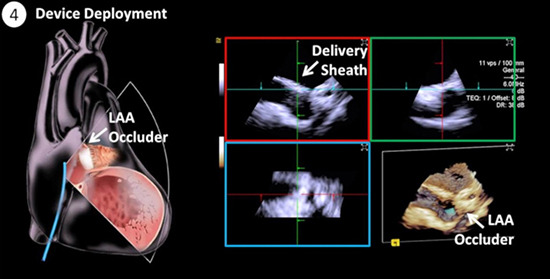
Intraprocedural Volume ICE Workflow
The LAA and the WATCHMAN device were characterized from multiple viewing angles, akin to TEE, by methodically orienting the multiplanar images reconstructed from the volume images [23]. Every effort was made to obtain the equivalent views on the 4D volume ICE that correspond to the requisite angles 0°, 45°, 90°, and 135°. A step-by-step description of a typical 4D volume ICE workflow for acquiring the four equivalent views of TEE is given below:
Step 1: With the ICE catheter tip placed in the middle right atrium, via the inferior vena cava, the ICE catheter can be rotated clockwise to visualize the LAA or the device.
Step 2: Once a 2D image visualizing the largest diameter of the LAA or the device is acquired, the imaging is 'suspended' or put 'on freeze'; this allows the operator to methodically rotate the corresponding planar lines on the MPR planes to view the LAA or the device at any angle of interest e.g. at TEE-equivalent 0°.
Step 3: With the planar tools locked orthogonally, the adjacent green plane becomes the TEE-equivalent 90° view.
Step 4: Rotating these 0° and 90° views clockwise by 45° will then generate the imaging planes at 45° and 135° respectively.
On both TEE and ICE, the LAA orifice width was measured on the coronal plane along the short axis (SAX) and the long axis (LAX) ([Figure 3A]; A: TEE, B: ICE), and on the non-coronal plane ([Figure 3B]; C: TEE, D: ICE). The LAA depth was measured from the center of the orifice to the apex of the appendage ([Figure 3C-Figure 3D]). The size of the compressed device was measured on both ICE and TEE ([Figure 4]; A: TEE, B: ICE) targeting an average compression of 8% to 20% relative to its physical dimension. Color Doppler was used for peri-device leak assessment on both TEE ([Figure 4C]) and ICE ([Figure 4D] and Supplemental Video 3). All the required measurements were acquired from multiple angles including the 2D orthogonal planes reconstructed from the 3D volumes. The ICE measurements were performed prior to the TEE measurements in the last 12 patients to avoid measurement bias. The manufacturer clinical specialist was present for ICE imaging for each of the procedure; TEE was performed by a separate operator.
Figure 3. LAA Sizing. LAA orifice width and depth are measured on multiple views on both TEE and ICE using planar (A and B; SAX: short axis, and LAX: long axis) and non-planar (C and D) views, to determine the maximal LAA sizing for device selection per the manufacturer's guidelines.
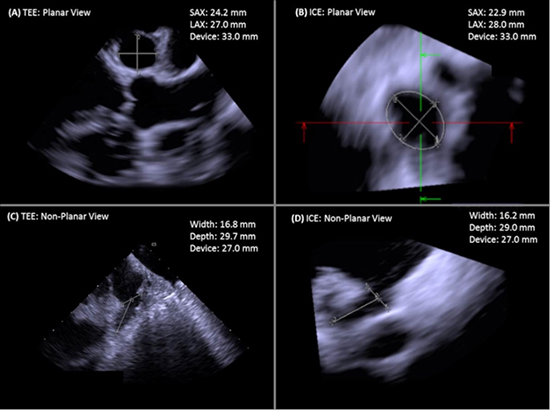
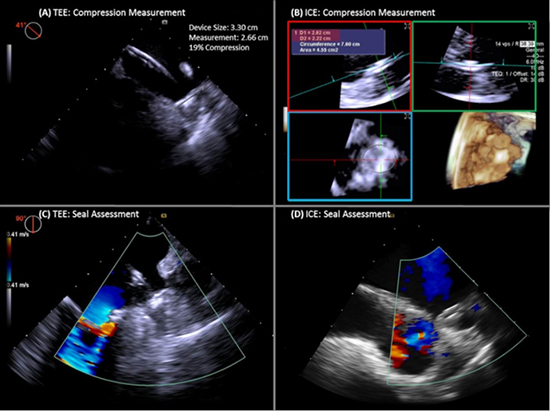
Figure 4. Compression Measurement. The device release criteria is followed to ensure adequate positioning, anchoring, sizing, and seal. Compression measurements are taken on both TEE (A) and ICE (B) to determine the adequate compression rate. Tug test is performed for adequate anchoring prior to device release, and Color Doppler flow is used to assess for peri-device leak (C and D; see Supplemental Video 3).
Measurements and Statistical Analysis
The LAAC procedure duration was calculated from the time of the first groin puncture for venous access to the time when the device delivery sheath was removed. The diagnostic fluoroscopy duration, the air karma radiation dose, and the total procedure duration were analyzed for each of the 15 patients, and accounted for the combined TEE and ICE guidance. Three intraprocedural imaging measurements were required for a successful LAAC guidance: the LAA orifice maximal width, the LAA maximal depth, and the device maximal diameter post implantation. Failure to acquire any of these three measurements was counted against the success rate of the imaging modality for guiding LAAC procedures. The average imaging success rate of TEE and ICE for LAAC guidance was defined by the number of patients with all three intraprocedural measurements. The imaging success rate was calculated for each of the three measurement variables.
The maximal orifice width and depth of the LAA and the maximal diameter of the implanted device were compared between TEE and ICE. The degree of correlation was calculated using the Pearson correlation coefficient (r) and the degree of agreement between the two modalities was assessed using the Bland-Altman method; two standard deviations were used to calculate the 95% limits of agreement and a normality test was performed. Statistical significance was considered at a p-value (p) of less than 0.05. Multiple measurements of the LAA orifice width and depth, and the device diameter post implantation were acquired from 2D images only. The Grubb's test was used to detect outliers. All statistical analyses were conducted using Minitab (version 18, Pennsylvania, USA).
From March 2018 through February 2019, 18 consecutive patients were recruited; 15 patients agreed to participate in the study. Atrial fibrillation was paroxysmal in two patients and permanent in 13 patients (87%) with a CHADS2-VASc score of 4.6±1. All 15 patients (age 78.6±8 years, BMI 28±4 kg/m2, 4 female) underwent successful WATCHMAN implantation [Table 1]. No major adverse cardiac events were observed during the procedures.
Table 1. Patient baseline and procedural characteristics.
| Baseline Characteristics |
Mean ± SD or Number |
| Age (years) |
75.6 ± 10 |
| Number of patients |
15 (4 female; 27%) |
| Body Mass Index (kg/m2) |
28 ± 4 |
| Indication for Exam
Permanent atrial fibrillation
Paroxysmal atrial fibrillation
CHADS2-VASc Score
|
12/15 (80%)
3/15 (20%)
4.6 ± 1
|
| Procedure time (min) |
102 ± 25 |
| Fluoroscopy time (min) |
16.07 ± 7* |
| Fluoroscopy dose (mGy) |
858 ± 792* |
| Contrast Agent (ml)
Visipaque
ISOVUE-300
|
2/15 (80-190)
13/15 (75-175)
|
| WATCHMANTM Device
21 mm
24 mm
27 mm
30 mm
33 mm
Device per patient
Overestimation
Underestimation
|
2/15 (13%)
3/15 (20%)
7/15 (47%)
2/15 (13%)
1/15 (7%)
20/15 (1.33)
3
2
|
| Imaging Measurement Success Rate for ICE
LAA Width
LAA Depth
Device Diameter
|
10/15 (67% overall)
14/15 (93%)
12/15 (80%)
11/15 (73%)
|
ICE = Intracardiac Echocardiography; LAA = Left atrial appendage; SD = Standard deviation; *Outlier removed
Procedural Characteristics
TEE was used for preprocedural LAAC planning. The LAAC procedure was performed under fluoroscopy with a mean air karma radiation dose of 858±792 mGy and a mean diagnostic fluoroscopic duration of 16±7 minutes; the air karma radiation dose for the first patient in the study was 10523 mGy which was detected as an outlier and removed from the mean dose calculation [Table 1]. Visipaque (80 ml to 190 ml) contrast was used in 2 patients whereas ISOVUE-300 (75-175 ml) was used in 13 patients to assess proper positioning of WATCHMAN for adequate LAA occlusion. The average procedure duration was 102±25 minutes.
The WATCHMAN device size varied among the patients from 21 mm to 33 mm with the most common size of 27 mm (47%; [Table 1]). The average device to patient ratio was 1.33 (20/15; the initial device size was overestimated in 3 patients and underestimated in 2 patients). Intraprocedural imaging guidance for LAAC was provided with TEE and volume ICE; the ICE catheter was positioned in the right atrium for all the 15 patients. The LAA orifice width was successfully measured with volume ICE imaging from the right heart in 14 out of 15 patients (93%). The LAA depth was successfully measured in 12 out of 15 patients (80%), and the diameter of the implanted device was successfully measured in 11 out of 15 patients (73%). On average, the three required measurements were successfully acquired with right sided ICE in 10 out of 15 patients (67%); the success rate for TEE was 100% for all the three measurement variables. The 5 patients with the missing measurements had challenging intracardiac morphology such as thickened interatrial septum or atrial hypertrophy that caused significant signal attenuation, or had highly calcified intracardiac tissues with previously implanted artificial valves that caused significant artifacts rendering the ICE image quality diagnostically insufficient.
Intraprocedural Measurements
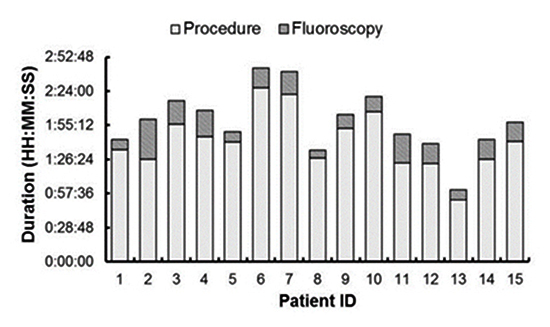
ICE measurements were consistent with TEE ([Figure 3-Figure 4], [Figure 5A]). The LAA orifice maximal width was 2.35±0.4 cm with TEE versus 2.41±0.5 with ICE (a 3% discrepancy in LAA sizing). The LAA maximal depth was 3.14±0.7 cm with TEE versus 3.14±0.6 cm with ICE. TEE and ICE measurements of the LAA orifice maximal width and the LAA maximal depth were moderately correlated (r = 0.63 and 0.65 respectively, both significant at p<0.05) with a systematic bias of -0.03 cm [-0.78, 0.72], and -0.07 cm [-1.32, 1.19] respectively ([Figure 5B-Figure 5C] respectively). The device maximal diameter or compression with TEE was 2.23±0.3 cm with an average compression rate of 15% compared to 2.27±0.3 cm with an average compression rate of 14% with volume ICE (a 2% discrepancy in device sizing); moderate correlation (r = 0.71, p<0.05) with a systematic bias of 0.008 cm [-0.24, 0.25] was observed [Figure 5D]. The procedure duration, including the diagnostic fluoroscopy duration was randomly distributed over the course of the study [Figure 6] and comparable to values reported in literature [7,8,11,13,17-19].
Figure 5. Correlation and Agreement Analysis. TEE and ICE measurements of LAA maximal width and depth, and the device maximal diameter (A) were moderately correlated with good agreement (B, C and D respectively); r = Pearson's correlation coefficient; SD = Standard deviation; 2SD was used to calculated the 95% limits of agreement.
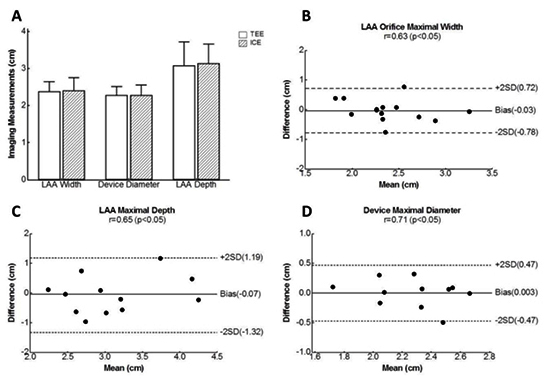
Figure 6. Procedural Characteristics. On average, the procedure duration (white) and the diagnostic fluoroscopy duration (stacked striped) were randomly distributed and comparable to reported values.
The main finding of this study is that volume ICE from the right heart can be used for intraprocedural sizing and guidance for transcatheter LAAC with measurements comparable to TEE. Proper patient selection, however, is essential for imaging success given the LAA distance from the right atrium and challenging patient characteristics such as interatrial hypertrophy or enlarged left atrium with calcific tissues that can impair the diagnostic image quality.
Our study adds to the growing body of literature establishing transcatheter left atrial appendage closure as a standard alternative to anticoagulation therapy for prevention of thromboembolic events in patients with atrial fibrillation. Atrial fibrillation accounts for 20% of all strokes, and LAA remains the primary source of thromboembolism in 90% of the patients with atrial fibrillation [1]. This has motivated the development and advancement of mechanical devices for transcatheter occlusion of the LAA. The WATCHMAN system is the only transcatheter device approved by the United States Food and Drug Administration (FDA) for LAAC. Transcatheter LAAC has shown to reduce risk of thromboembolic events such as stroke and systemic embolism comparable to warfarin [24,25]. LAA was successfully occluded with the WATCHMAN device, with adequate positioning and implantation of the device confirmed by contrast-enhanced fluoroscopy, TEE and ICE. Color Doppler was adequately used on both TEE and ICE for peri-WATCHMAN leak assessment on all 15 patients; no significant leak was observed.
An average of 1.33 WATCHMAN devices was deployed per patient in this study which is comparable to 1.8 devices per patient reported in the first half of the PROTECT AF study [24], 1.38 reported in the post-FDA approval study [25], 1.1 reported in the LAAC study using TEE and 2D ICE [11,16], and 1.25 reported in the LAAC study using TEE and 3D computed tomography (CT) image guidance aided with 3D LAA prototyping for LAAC planning [4]. In the latter study, patient-specific 3D prints of LAA were reconstructed from its preprocedural 3D CT image and used for device selection by test-fitting the WATCHMAN device, ex-vivo, in situations where the LAA ostium was ambiguous. The supplemental 3D printing for LAAC planning combined with 3D CT guidance for WATCHMAN implantation was shown to reduce the procedure duration to 48 minutes (±11) by providing accurate sizing. With the increasing role of 3D printing in the preprocedural planning of a wide range of structural heart interventions, low-cost options for rapid 3D prototyping have emgerged [26]. This is beneficial for LAAC planning given the complex morphology of the LAA [17,26], and could potentially benefit intraprocedural ICE guidance.
Our data demonstrated the feasibility of right sided 4D volume ICE guidance for LAAC, avoiding procedural complications and without the need for transseptal access. Identifying the anatomical landmarks, e.g. the Aortic Valve, facilitates spatial orientation and confidence in catheter navigation. We found that certain intracardiac tissue characteristics could significantly affect the diagnostic image quality. Imaging of the LAA from the right atrium or the right ventricle demands a larger imaging depth requiring the ultrasound signal to travel through the interatrial septum. Larger attenuation in the presence of highly muscular or fibrous interatrial septum or fossa ovalis can greatly reduce the diagnostic image quality of LAA. Atrial hypertrophy or enlargement can have a similar effect on the image quality as observed in this study and previously reported by Matsuo et al [16]. The image quality becomes diagnostically insufficient in the presence of acoustic shadowing and reverberation artifacts caused by highly calcified cardiac tissues such as a calcific aortic valve or annular calcification, or in the presence of mechanical or bioprosthetic valves. Imaging from the right ventricular outflow tract, the left atrium, the coronary sinus, or the proximal pulmonary allows optimal visualization of the LAA although with a steeper learning curve [9,14]. These alternatives were not attempted in this study since the objective was to evaluate the performance of ICE guidance from the right heart for LAAC in comparison to TEE.
Intraprocedural Measurements
Intraprocedural TEE and ICE measurements of the maximal width and depth of the LAA, and the compressed WATCHMAN diameter showed moderate correlation and good agreement. Overall, volume ICE tends to overestimate the LAA dimensions compared to TEE similar to the findings reported by Matsuo et al. (2016) [16]. Likewise, Wang et al. (2016) also reported LAA undersizing by TEE compared to 3D CT and showed 3D CT guided LAAC to be more accurate, safe, and faster than TEE or fluoroscopy alone [4]. In this study, every effort was made to emulate the TEE equivalent views on 4D volume ICE by utilizing its MPR feature. It should also be noted that in TEE the intracardiac anatomy and the intracardiac device are imaged from outside the heart, i.e. from the esophagus, and the heart may be rotated with respect to the viewing angle on TEE. On the contrary, the cardiac rotation becomes inconsequential in ICE since the intracardiac anatomy and the intracardiac device are imaged from within the heart with the ICE angulation adjusted for. Fluoroscopy was used to guide device delivery and implantation throughout the study.
The diagnostic fluoroscopy time in our study was 16.07±7 minutes which is comparable to the fluoroscopy durations reported in similar studies (9.8±4.5 minutes [17]; 25±11 minutes [11]; and 30.4±17 minutes [19]). Because the new ICE catheter used in this study is larger than the previous generation (12.5Fr versus 8Fr for 2D ICE and 10Fr for 3D ICE), additional fluoroscopy was performed for precautionary purposes. This also explains the high air karma radiation dose of 10523 mGy observed in the very first case of the study. Similarly, the total procedure time in this study was 102±25 minutes, which is longer than 42±13 minutes reported in a study evaluating a dual-imaging guidance [14], and 65.8±15 minutes reported in a left atrial ICE guidance [19] but shorter than 103±33 minutes reported in a 2D ICE guided LAAC study [11]. This variability in procedure time, fluoroscopy time, and fluoroscopy dose indicates that the procedural characteristics are dependent on study settings, operator experience, and unique patient characteristics.
The primary benefit of 4D volume ICE imaging guidance for transcatheter LAAC is the possibility to avoid the use of GETA during LAAC and the possibility to expand LAAC care to patients with contraindications to GETA and TEE [27]. A recent case study by Perez et al. (2019) demonstrated successful provision of transcatheter LAAC care to a patient with apixaban-associated gastrointestinal bleeding; the procedure was guided with 4D volume ICE under conscious sedation [27]. Furthermore, procedures with GETA are often associated with masked neurological complications, pulmonary complications related to endotracheal intubation such as airway injury during intubation or post-intubation pneumonia, longer procedure time, higher personnel costs related to the need for an anesthesiologist, and importantly prolonged recovery time for the patient [7,28]. ICE guidance under conscious sedation can avoid GETA related complications, reduce patient discomfort and recovery time, and improve procedural efficiencies by reducing resource utilization [6,27,28]. Although the intraprocedural measurements with volume ICE were comparable to TEE, ICE characterization of the LAA from the right atrium did not have the same diagnostic confidence of TEE in 33% of the patients. While TEE guidance was required for LAAC in these patients, the finding that the diagnostic quality of right sided volume ICE was similar to TEE in the remaining 67% of the patients is suggestive of the possibility that LAAC can be performed without the need for TEE and hence without GETA. Furthermore, right sided ICE guidance avoids transseptal advancement of the ICE catheter into the left atrium and reduces risks for procedural complications.
We believe that proper patient selection, based on their intracardiac anatomical complexity, might help select appropriate imaging modality and optimal catheter placement for adequate intraprocedural guidance. Given the superior diagnostic quality of left sided ICE demonstrated by multiple studies, a direct comparison between the left sided and the right sided volume ICE intraprocedural guidance might help formulate workflow guidelines and standardize LAAC procedures while accounting for unique patient characteristics. In our study, efforts were made to standardize the volume ICE workflow in relation to the established TEE protocol. A workflow integrating preprocedural selection of the imaging modality, either right sided ICE or left sided ICE or TEE or 3D CT, for intraprocedural LAAC guidance may facilitate staff scheduling, e.g. between an echocardiologist and the anesthesiologist, and optimize resource allocation, e.g. TEE versus ICE, or CT angiography versus fluoroscopy. Preprocedural planning using CT might be beneficial in simplifying the LAAC workflow using 4D volume ICE with comparable 3D coronal measurements. The present study did not use CT for preprocedural planning. Preprocedural planning may also be supplemented with 3D LAA prototyping for ex-vivo¬ simulation of the LAAC procedure, particularly in patients where right sided ICE characterization of the LAA may be non-diagnostic. 3D LAAC simulation may contribute to reducing the learning curve associated with ICE guidance particularly by facilitating catheter placement and identifying anatomical landmarks for spatial orientation during the procedure.
Our study is limited by its small sample size. Larger multi-center and randomized studies are needed to expand our understanding of the benefits and challenges of volume ICE intraprocedural guidance for different structural heart procedures, and in comparison, to different imaging modalities such as 3D CT. The intraprocedural measurements required for LAAC guidance were obtained on 2D multiplanar images; future studies should focus on the accuracy and feasibility of 3D imaging measurements. Our study did not have a control group. Proper patient selection for the success of volume ICE guidance for LAAC needs to be investigated. Cost due to the one-time usage of the catheter is a primary concern. A recent study comparing procedural and cost considerations between 2D ICE and TEE showed that the total hospital charges for ICE with local anesthesia were similar to TEE with GETA but with significantly lower professional fees for ICE by avoiding high technical fees associated with TEE, anesthesia and recovery rooms [28]. Studies evaluating both the clinical impact, including knowledge gain and workflow efficiency, and the financial impact of volume ICE substitution for TEE would be highly relevant.
This study was the first to evaluate the clinical feasibility of wide-angled (90° x 50°) 4D volume ICE for intraprocedural guidance of LAAC. TEE is the current gold standard but requires GETA whereas ICE can be performed under conscious sedation and presents an alternative for patients with contraindications to GETA or TEE. This study demonstrated the feasibility of right sided ICE guidance for LAAC, without the need for a transseptal access and with measurements comparable to TEE. Larger prospective studies with proper patient selection, optimized preprocedural guidance, and standardized workflow should be performed to determine the clinical efficacy and outcome of volume ICE guidance for LAAC in comparison to TEE.
4D volume ICE imaging from the right heart circumvents the need for a transseptal access for providing intraprocedural imaging guidance during LAAC; multiple MPR echo views and anatomical landmarks help optimize the LAAC procedural guidance but suffer from non-diagnostic image quality in the presence of challenging patient characteristics. Standardized workflow based on proper patient selection and optimal preprocedural preparation, including adequate training to reduce the learning curve, may improve the imaging success rate of volume ICE guidance from the right heart for transcatheter LAAC procedure. This is promising for patients who have contraindications for TEE or intolerance to anesthesia necessitating a TEE alternative for intraprocedural LAAC guidance.