A Cost-Utility Analysis of Cryoballoon Ablation versus Radiofrequency Ablation for Paroxysmal Atrial Fibrillation
Marie-Isabel Murray1,2*, Mireira Jofre- Bonet3, Huseyin Naci2, Andreas M. Zeiher1
1
Department of Cardiology, University Hospital Frankfurt, Frankfurt am Main, Germany.2
Department of Health Policy, London School of Economics and Political Science, London, UK.3
Department of Economics, University of London, London, UK.
The objective of this study was to evaluate the cost-effectiveness of the treatment with cryoballoon
(CB) compared to the standard treatment with traditional irrigated radiofrequency (RF) ablation
for pulmonary vein isolation in patients with paroxysmal atrial fibrillation (pAF) refractory to
antiarrhythmic drug therapy.
A decision tree model was developed to graphically depict the probabilities, utilities and costs of
CB compared to RF therapy. Data from a conducted systematic literature review and meta-analysis
of only RCTs were used to evaluate clinical outcomes of CB and RF treatments, including success
rates after one year, complications and recurrence of atrial fibrillation.
The cost-utility analysis estimated that, CB therapy had £1,747 higher cost, and 0.0114 more
quality-adjusted life years (QALYs) compared to standard RF treatment over a one-year time
horizon. The incremental cost per QALY of CB ablation compared to RF ablation was estimated
to be £152,836/QALY.
Based on current evidence, CB ablation for pulmonary vein isolation in patients with pAF is costeffective
compared to RF if decision makers are willing to pay £152,836 or higher for a QALY.
Key Words : Cost-Utility Analysis, Cryoballoon Ablation, Radiofrequency Ablation, ICER/ICUR.
Correspondence to: Dr. Marie-Isabel Murray, Theodor-Stern-Kai 7, 60590 Frankfurt am
Main, Germany
Paroxysmal atrial fibrillation (pAF) is a common type of arrhythmia that is defined by an irregular
and often rapid heartbeat. This arrhythmia is associated with a reduced quality of life, high cost
and increased mortality [1,2]. Multiple randomized and non-randomized studies demonstrated
that pulmonary vein isolation (PVI) is an effective treatment for drug-refractory pAF when
compared to anti-arrhythmic pharmacotherapy (AAD) alone [3-5]. The traditional method is a
point-by-point ablation of the circumference of the pulmonary veins using irrigated radiofrequency
(RF) energy. A newer technology uses a cryoballoon (CB) which is placed in the pulmonary vein
ostia, and then delivers freezing energy to isolate the pulmonary veins circumferentially in a single
shot. Multiple studies have proven that both technologies are similarly effective in treating pAF
and have low complication rates [6-9]. Furthermore, previous trials based on ablation outcomes
have suggested that AF ablation with RF and CB catheters is cost-effective for patients with pAF
compared to ADD therapy [5,10-12].
However, there has not been a study comparing the cost-effectiveness of CB versus RF therapy
using outcome data from only randomized controlled trials (RCTs). The objective of this study
was to use data from a published systemic review and meta-analysis to perform a cost-utility
analysis in order to estimate the incremental cost-utility ratio (ICUR) gained for CB ablation
compared to RF therapy over a one-year time horizon.
Modeling Strategy and Basic Assumption
A decision-analytic model was developed to estimate costs, health outcomes and incremental costeffectiveness
of RF ablation compared to CB treatment for pAF. We chose to use a short-term
decision tree model instead of a long-term Markov model since most published RCTs comparing
CB or RF ablation are limited to a 1-year follow-up. Patients with pAF were chosen because
consensus guidelines have recommended ablation in these patients and ablation appears to result
in better outcomes in patients with paroxysmal compared to persistent AF [13].
The probability of being in normal sinus rhythm at one year, as well as specific procedure
complications, were derived from data presented in a meta-analysis conducted by Murray at el.
[14]. In this systematic review, four RCTs were identified which compared CB and RF therapies
in pAF patients regarding different primary outcomes, including success rates one year after
ablation, complications and recurrence of AF [6-9]. Success rate was defined as freedom from
documented AF one year after ablation. Each documented episode over 30 seconds following a
three-months blanking period was considered a failure, as per current guidelines [15].
Complications were defined as adverse events that occurred during or immediately after the
procedure [Table 1].
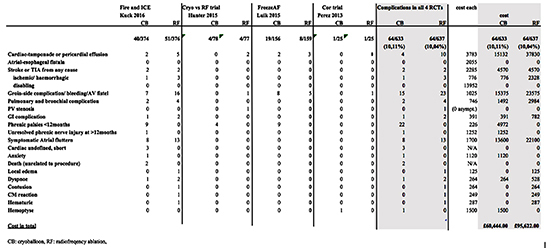
Table 1. Estimates of key costs for the complications
Figures 1 and 2 graphically present the decision tree model with health status, costs and
probabilities used in our analyses. Two decision tree processes were constructed: one for patients
receiving CB therapy [Figure 1], and another for standard RF therapy [Figure 2]. Both procedures
follow the same pathway with different probabilities: after ablation some patients complete an
uncomplicated, successful ablation (1); a proportion of patients are at risk of complications (all
relevant complications are listed in [Table 1]) [Table 2]; and others have AF recurrence (3). With the
exception of a procedure-related stroke, ablation patients experiencing a procedural complication
incurred an immediate cost and short-term disutility. Immediately after that, they followed the
same path as patients without a procedural complication. We assume that a procedure-related
stroke would impact both quality-adjusted life expectancy and costs in the long-term, and these
effects were estimated from previous studies [16].
Figure 1. Decision Tree Cryoballoon Ablation
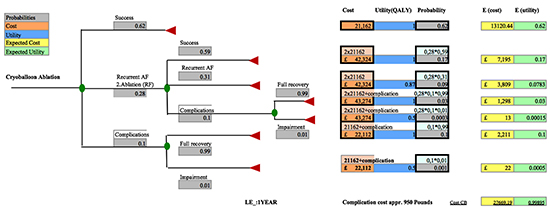
Figure 2. Decision Tree Radiofrequency Ablation
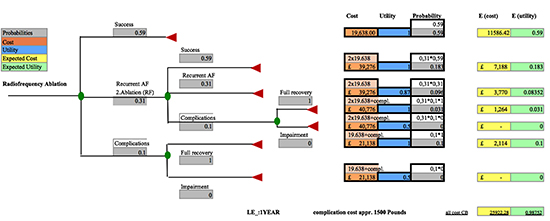
Patients with recurrent AF despite one ablation proceed to repeat ablation. However, this time all patients receive the RF standard ablation. The path of these patients is equal to the path of the first ablation with RF. After the second ablation we assume that there will not be a third ablation performed, because the changes of clinical success are strikingly limited and electrophysiologists do not typically recommend a third ablation.
Since the mortality rate during and immediately after the procedure was zero and the two patients who died in the CB group had deaths completely unrelated to the procedure, we did not include the possibility of mortality in our decision tree model.
Data from a conducted systematic literature review and meta-analysis were used to estimate the clinical probabilities of CB and RF treatments [14]. These include the probability of achieving asuccessful ablation after one year, the probability of re-ablation procedures and the probability of complications with CB and RF treatment. Targeted reviews were performed to identify studies addressing the other clinical model variables. The details of the probabilities used are shown in[Table 2].
Table 2. Summary of important numeric values and parameters
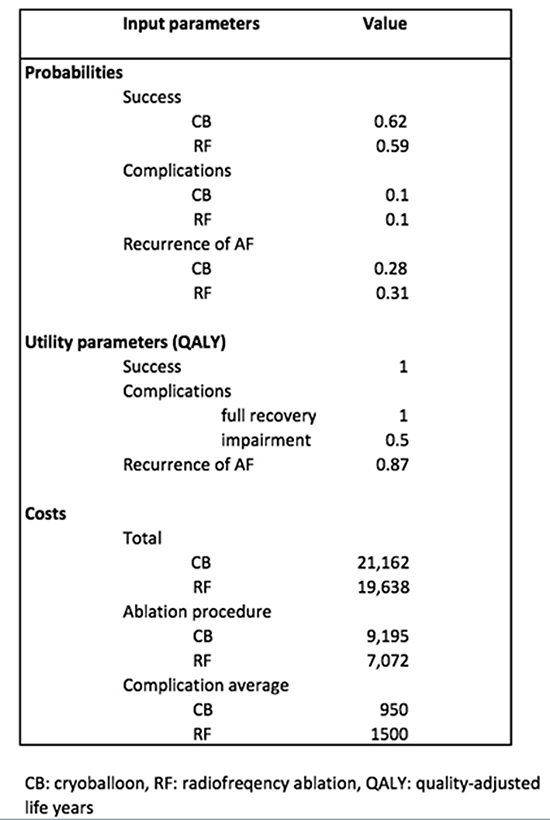
We assessed a single procedure success rate of 0.62 for CB ablation and 0.59 for RF ablation. The complication rate was 0.1 in both groups. After AF recurrence, RF therapy was performed and therefore we assumed a second procedure efficacy rate of 0.59, equally to the first RF procedure.
All health care costs are presented in Pounds. The primary outcomes of interest for this study included variable hospital costs for the ablation visits (procedure costs, supplies and medication) and complication events. Fixed costs, like capital costs or overheads, were not included in our cost evaluation, as they would only be minimally impacted by differences in treatment. We also did not estimate indirect costs, because we assumed that the costs would be similar for both treatments. The majority of cost parameters were taken from the NHS Payment by Results (PbR) tariffs. Further cost estimates were based on existing economic analysis, personal and social care costs and resource use estimates from large databases [17].
The cost for CB ablation were estimated using data from a previous published study [12].
Additionally, it has been demonstrated in multiple studies that the procedure with RF therapy is
less expensive than CB [18-19].
The cost of complications is depicted in [Table 1]. Procedural complications were valued based on
national tariffs. Phrenic nerve palsy was assumed to require CT scan and cardiology outpatient
visit. Costs for additional drug therapy was not included in the calculation, since this would likely
affect both groups equally. The average cost for procedural complications were £950 in the CB
group and £1500 in the RF group. The main reasons for the cost difference were the higher rate of
cardiac tamponade and groin-side complications caused by RF ablation.
The quality-adjusted life years (QALYs) for individual health status were obtained from published studies after a comprehensive literature review [12,20]. Despite consideration of a large number of studies, no single source was identified which could provide all of the baseline information necessary to apply incremental changes in utility according to health status. Patients with successful pAF ablation were assumed to revert to having the same QALY as the general population. For the other main health conditions, specific decrements were estimated. The quality of life and utility decrements used in the model are presented in [Table 2].
The cost-utility analysis followed the standard guidelines of economic evaluations [21]. The expected costs and outcomes of CB and RF treatments were calculated and ICUR was determined. An ICUR was calculated by dividing differential costs with differential QALYs between existing practice and the new health technology (ICUR= C2-C1/U2-U1). It is worth noting that, in multiple studies, incremental cost-effective ratio (ICER) and ICUR are used interchangeably. Furthermore, we did not apply discount rates, because effectiveness and costs were taken as unique values at the end of one year.
The robustness of model predictions was explored using one-way sensitivity analyses by varying input parameters in plausible limits. These parameters included the cost of CB treatment, cost of CB complications and the probability of AF recurrence with the CB approach.
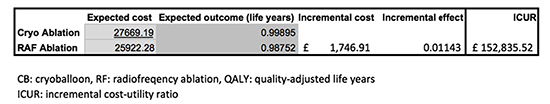
The results of the cost-utility analysis are shown in [Table 3]. They are based on a one-year time horizon including both costs and QALYs. CB ablation, compared with RF ablation, results in greater costs (£27,669 vs. £25,922) and greater QALY (0.998 vs. 0.987). These results yield an
ICUR of £152,836/QALY gained. Therefore, using this analysis, ablation with CB would be considered cost-effective if societies’ willingness to pay for a QALY is £152,836 or higher.
Table 3. ICUR of CB vs. RF treatment

One-Way Sensitivity analysis
A sensitivity analysis was performed to study the uncertainty of some important model parameters
[Table 4]. We performed one-way sensitivity analyses to assess the degree of change in results with variation of one model input parameter value at a time. We chose the following parameters
for our sensitivity analysis: cost of CB treatment, cost of complications with CB and the probability
of AF recurrence after CB ablation. [Table 4] presents the incremental cost per QALY for the
different parameters. Changes in the cost of CB treatment and the AF recurrence rate have a
substantial impact on the model’s conclusion. If the CB cost is reduced to £15,000, the incremental
cost per QALY ablation compared to RF ablation would be £-158,005. Whereas if the CB cost is
£25,000, the incremental cost per QALY would increase to £429,832 per QALY. Furthermore, if
the probability of AF recurrence is assumed to be 0.15 or 0.35, the cost per QALY becomes
£57,881 and £429,832, respectively.
Table 4. One-Way Sensitivity Analysis
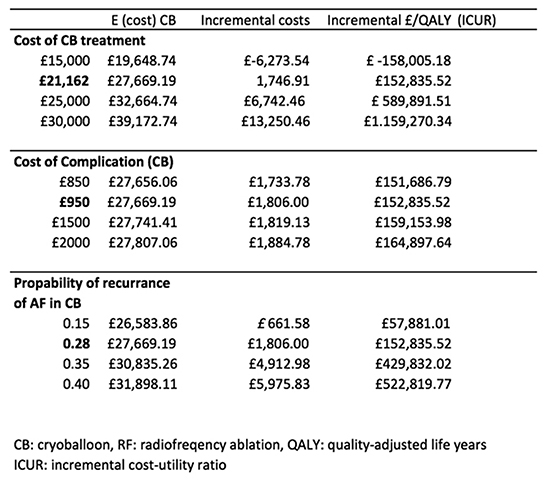
On the other hand, the average cost of CB complications had a relatively small impact on results.
When the cost of CB complications is £850, the incremental cost per QALY becomes £151,687
and it increases to £164,898 per QALY, when the cost of CB complications is £2000.
CB ablation has been used as an alternative treatment to RF catheter ablation for pAF in the past
years. Many studies showed comparable clinical results [6-9]. However, limited evidence exists
about the cost-effectiveness of this relatively new technology compared to the standard RF
treatment. In this health economic analysis, we demonstrated that CB ablation increases medical
care costs and QALY compared to RF with an estimate of 152,836/QALY. Based on common
cost-effectiveness thresholds, which are currently £20-30,000 per QALY gained in the UK, AF
ablation with CB may not be regarded as a more cost-effective strategy than RF. The cost of the
ablation procedure was a relevant proportion of the total cost, which was significantly higher in
the CB ablation procedure (£9,195.64 v. £7,072.64). Furthermore, the sensitivity analyses revealed
that the most important impact on ICUR was the total cost of CB and the recurrence rate of AF. If
in the future the ablation cost for the new technology decreases, CB ablation might become more
cost-effective compared to RF therapy.
This study shares the general limitations of economic modelling. Complex medical practice is
difficult to convert into a decision tree model and details may be missed. This applies to our model
as well. We used clinical probabilities from a meta-analysis which included four RCTs. The RCTs
had an average time-frame of one year and therefore, our cost-utility analysis had only a oneyear
time horizon. Studies about long-term outcomes of different ablation procedures are still
limited and long-term effects should continue to be investigated in the future. In addition, new
technologies of both ablation catheters are evolving constantly. This may result in an
improvement in efficacy and may change the outcome of our analysis. For example, the Fire and
ICE trial demonstrated a significant difference in freedom from cardiovascular rehospitalization between catheter types [22]. Patients treated with the second-generation CB experienced a
higher rate of freedom from cardiovascular rehospitalization than those treated with the firstgeneration
CB. It also should be noted that RCTs may represent an overly optimistic view of care
delivery compared to routine practice in the broader patient population [23]. RCTs usually
conduct research on highly selective populations in tightly controlled settings. Participants may
fail to sufficiently reflect the actual clinical site required to represent the entire patients
population. Furthermore, QALY data were not presented in the RCT trials, thus we had to assume
that all patients with recurrence of AF had a similar QALY. However, many patients with
recurrence of AF have no symptom or less symptoms after catheter ablation [24-25]. Those
patients may be suitable for rate-control and anticoagulation strategy rather than repeat
catheter ablation. Particularly, patients with recurrent, symptomatic AF more than 3 months
after initial ablation should be considered for repeat ablation.
We used cost parameters from NHS PbR tariffs for our analysis which have been used for costeffectiveness
studies in many previous analyses [12,26,27]. The advantage of using these tariffs
is that they represent the national average costs for hospital procedures in England, and the price
for a particular procedure is standardised. Because our model used PbR tariffs to approximate
costs of the ablation procedure and complications instead of adding all individual costs together,
there may be scenarios in which tariffs do not reflect the true costs of the treatment. Some
patients with atrial fibrillation are elderly and frail, with multiple comorbidities such as diabetes,
renal dysfunction and other chronic conditions, and may need additional care with an increased
length of stay. Our model does not include cost adjustment for other comorbidities and PbR
tariffs may not reveal the true complexity and cost of a patient episode. In addition, we assumed that indirect costs would be the same for both treatments. It is possible, however, that the two
therapies could differ in non-medical costs such as loss of work force or reduced productivity.
Lastly, a Markov model might be superior to our model, since a Markov model is especially useful
when events occur repeatedly, such as the repeated occurrence of atrial fibrillation [28]. However,
the published RCTs comparing the proportion of patients achieving normal sinus rhythm
including complication rates after CB and RT ablation are limited to a one-year follow-up,
and therefore we decided to use a decision tree model.
Several previous studies have assessed the potential cost-effectiveness of pAF ablation with RF
and CB compared to AAD therapy in different countries [5,10,11]. For instance, Reynolds et al.
(2014) compared the cost-effectiveness of CB ablation with ADD therapy from the UK perspective
[12]. These studies support the claim that both procedures improve QALYs compared with AAD
therapy in a similar magnitude. Thus, it was stated that RF and CB ablation should be offered
similarly from a health policy perspective [12]. Hunter et al. (2016) is the only author, who
published a cost analysis of AF ablation comparing CB and RF therapy from a US perspective [6].
Similar to our study, they revealed that inpatient costs were 30.0% higher for CB ($27,954) than
for RF ablation ($21,563). Furthermore, the adjusted outpatient costs were 19.5% higher for CB
than for RF therapy. However, in this study neither incremental cost per QALY gained nor ICER
were evaluated and consequently no conclusion about cost-effectiveness could be drawn. Our costutility
analysis is the first study comparing cost-effectiveness of CB with the standard RF ablation.
In our current analysis, we demonstrated that CB ablation is not more cost-effective than RF
therapy. However, some other aspects of this newer intervention should be considered before making a decision. For example, CB ablation is less painful than RF ablation and thus some
patients might prefer this treatment to RF therapy [29]. Additionally, some publications
demonstrated that CB ablation of PVs is a simple and straightforward procedure with a faster
learning curve than RF ablation [29,30]. Consequently, some electrophysiologists in training might
have a higher success rate after PVI with this new technology. Lastly, CB ablation was designed
to prevent the need for a mapping system and creation of multiple ablation lesions to achieve
shorter procedure time [31,32]. Further cost-effectiveness studies must be conducted to evaluate
if this might be beneficial for hospitals.
Our cost-utility analysis concluded that currently, the treatment of pAF with CB might not be more
cost-effective than RF ablation, with an estimated ICUR of 152,836/QALY. However, a shorter
procedure time, a less painful procedure and a faster learning curve are features of the new
technology that could be beneficial for many patients, physicians and hospitals. Furthermore, if
the cost for the new CB technology diminishes in the future, it might become more cost-effective
than RF, since ablation costs had the biggest impact in our sensitivity analysis.