Electrical Isolation Following Thoracoscopic Left Atrial Appendage Exclusion During Hybrid Ablation for Longstanding Persistent Atrial Fibrillation
Ali Hassan Syed M.1, Sarah Paleczny1, Bobby Yanagawa2, Benedict Glover3, Gianluigi Bisleri2
1Division of Cardiac Surgery, Queen’s University, Kingston, ON, Canada.2Division of Cardiac Surgery, University of Toronto, Toronto, ON, Canada.3Division of Cardiology, University of Toronto, Toronto, ON, Canada.
Left atrial appendage (LAA) exclusion with the use of the AtriClip (AtriCure, Inc., OH, USA) device has been shown to be a safe, effective, and durable strategy predominantly to reduce the lifelong risk of thromboembolism and stroke in patients with atrial fibrillation (AF). We present a case showing electrical isolation of the LAA after its exclusion with the AtriClip device during hybrid ablation for the treatment of longstanding persistent AF. Our case demonstrates the effectiveness of the AtriClip device in not only mechanically occluding the LAA but also electrically isolating it, thereby addressing an electrical driver of AF in addition to reducing its thromboembolic sequelae.
Key Words : .
Gianluigi Bisleri, MD, FRCSC
Division of Cardiac Surgery
St. Michael's Hospital- Bond 8
30 Bond Street
Toronto, ON, Canada, M5B1W8
The left atrial appendage (LAA) is a known risk of ischemic stroke in atrial fibrillation (AF); however, it is also responsible for ectopic foci in 27% of AF patients presenting for repeat ablation procedures and LAA electrical isolation can reduce AF recurrence rates 1. LAA exclusion with the use of the AtriClip (AtriCure, Inc., OH, USA) device has already been proven to be a safe, effective, and durable strategy predominantly to reduce the lifelong risk of thromboembolism and stroke 2-5. We present a case demonstrating a secondary benefit of LAA exclusion with the AtriClip device in achieving electrical isolation of the LAA, thereby treating a potential trigger and driver of long standing persistent atrial fibrillation (LsPAF) as well.
A 59-year-old man presented with 10 years of LsPAF refractory to anti-arrhythmic drugs and 2 unsuccessful cardioversions. He was in NYHA III with severe limitations to his daily activities. A pre-operative transthoracic echocardiogram (TTE) showed left atrial volume index of 33 ml/m2, left atrial antero-posterior diameter of 4.7 cm, left ventricular ejection fraction of 56%, and no evidence of valvular disease.
Hybrid ablation for LsPAF and epicardial left atrial appendage exclusion was performed by right and left thoracoscopy, respectively 6, 7. Briefly, the patient was placed in a 30-degree left lateral decubitus position and following right lung deflation, three 10 mm trocars were placed in the 3rd, 4th and 5th right intercostal spaces. Pericardiotomy was performed 3 cm anterior and parallel to the phrenic nerve at the level of the SVC to the junction of the IVC and the transverse and oblique sinuses were accessed with blunt dissection. During surgical dissection, simultaneous endovascular access was obtained for insertion of endocardial mapping catheters.
A baseline endocardial map was created using the EnSite Precision mapping system (Abbott) after removal of all surgical instruments to avoid the risk of electrical interference. The baseline voltage map provided an initial assessment of the atrial substrate indicating the voltage conductance at each anatomical location in the left atrium including the left atrial appendage (LAA). The threshold for high voltage was set at >0.5 mV and a color-coded voltage map was generated.
After endocardial mapping, a baseline epicardial voltage map was generated via a 15mm Advisor circular loop mapping catheter (Abbott) inserted through the thoracoscopic surgical port and applied to the posterior epicardial surfaces. Following this, epicardial box ablation was performed via the Fusion 150 device (Fusion, AtriCure, OH, under Health Canada Special Access Program) positioned around the pulmonary veins for a total of 18 mins. Endocardial mapping did not show any surgical gaps, and so there was no need for left-sided endocardial ablation. Entrance and exit block were successfully achieved. The rhythm spontaneously converted from atrial fibrillation to typical atrial flutter, and ablation was performed in the right atrium endocardially at the level of the cavotricuspid isthmus and conversion to normal sinus rhythm was achieved.
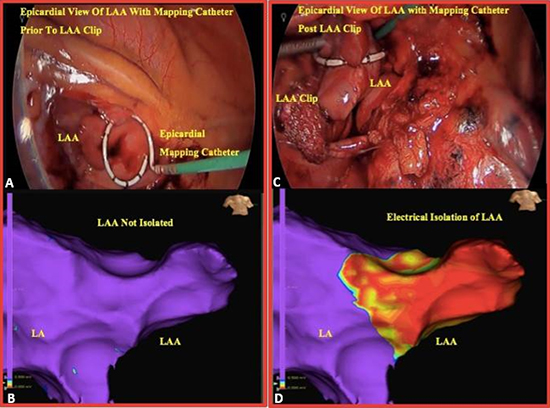
After completion of the ablation and right sided closure, epicardial mapping of the LAA was performed via a left thoracoscopic approach showing electrical activity (Video 1; [Figure 1] A, B). LAA exclusion was then performed with the AtriClip device as we have described before 7. In this case, a size 50 AtriClip was successfully deployed. Left sided closure was then meticulously performed to avoid complications such as lung hernia 8. Post-exclusion epicardial mapping via a loop catheter showed complete electrical isolation of the LAA (Video 1; [Figure 1] C, D). There were no post-operative complications, and the patient had an uneventful stay at the hospital and was discharged on post-operative day 2 in sinus rhythm. At 1-year follow-up the patient was doing well and in sinus rhythm on antiarrhythmic drugs.
Figure 1. A) Baseline epicardial mapping of the LAA showing B) electrical activity (purple; voltage > 0.5mV). C) Epicardial mapping after AtriClip LAA exclusion D) showing complete electrical isolation (red).
Atrial fibrillation is independently associated with a 1.5- to 4-fold increased risk of mortality 9. The addition of LAA exclusion to catheter ablation has been shown to improve freedom from AF at 1 year compared to no LAA exclusion 10. While the more commonly reported extra pulmonary vein sites of AF initiation and maintenance are the superior vena cava, ligament of Marshall, coronary sinus, crista terminalis, and left atrial posterior wall, the LAA is an underreported but important site of AF drivers that can potentially sustain LsPAF 1. Electrical isolation of the LAA has been demonstrated to occur immediately following LAA ligation and is postulated to be due to ligation induced ischemic necrosis 11 The AtriClip device has been shown to be successful in achieving LAA occlusion in 97.8% of patients 4 and thus represents a readily available and safe treatment strategy for effective LAA exclusion. Our case demonstrates the effectiveness of the AtriClip device in not only mechanically occluding the LAA but also electrically isolating it, thereby addressing both a driver of AF as well its thromboembolic sequelae.