Use of Intraprocedural Ibutilide During Stepwise Ablation of Long-Standing Persistent Atrial Fibrillation
Andres Enriquez1, Javad Hashemi2, Kevin Michael2, Hoshiar Abdollah2, Christopher Simpson2, Adrian Baranchuk2, Damian Redfearn2
1Section of Cardiac Electrophysiology, Hospital of the University of Pennsylvania, Philadelphia, Pennsylvania..2Division of Cardiology, Queen’s University, Kingston, Ontario, Canada..
Catheter ablation is an effective therapy for symptomatic atrial fibrillation (AF). The aim of this study was to assess the effect of ibutilide administration in patients with long standing persistent AF undergoing catheter ablation.
We included 25 patients undergoing stepwise catheter ablation with ibutilide 1.0 mg infused prior to mapping and ablation as first step. Procedural and long-term outcomes were compared to a matched cohort of 25 patients in which ibutilide was not used but all other steps remained the same.
Mean age of the cohort was 65.6±8.2 years, and duration of persistent AF 71.7±96.8 months. Termination to sinus rhythm (SR) directly or through an atrial tachycardia (AT) was achieved in 88% of patients administered ibutilide (32% SR/68% AT) vs. 64% in the control group. Ibutilide was associated with increased AF mean cycle-length (mCL) (208.3±31.6 vs. 156.0±23.7 ms; p<0.001) and decreased CFE mean surface area (29.2±20.2% vs. 47.3±13.7%; p=0.002). Procedure and radiofrequency (RF) times were less in the ibutilide group (288.8±49.6 vs. 335.3±47.4 min and 66.0±16.0 vs. 78.0±18.2 min; p=0.002 and 0.029 respectively). The 1-year recurrence was 44% in the ibutilide group and 60% in the control groups (p=0.29). Ibutilide patients had significantly reduced ShEn (6.1±0.14 vs. 7.09±0.14; p<0.001) and ShEn was higher in patients that recurred (6.47±0.24 vs. 5.73±0.15; p<0.001).
In long-standing persistent AF the use of ibutilide in the context of a stepwise ablation results in increased AF mCL, reduction of fractionation and ShEn and higher rates of AF termination, more often through an intermediate AT. Procedure and RF times are also decreased, without compromising long-term outcomes.
Key Words : Atrial Fibrillation, Catheter Ablation, Stepwise Approach, Ibutilide.
Correspondence to: Damian P Redfearn, MD
Heart Rhythm Service
Kingston General Hospital K7L 2V7
Queen's University.
Catheter ablation is an effective therapy for symptomatic, drug-refractory atrial fibrillation (AF)[1-3]. Pulmonary vein isolation (PVI), the standard ablative strategy for paroxysmal AF is insufficient in patients with persistent AF and long-standing persistent AF. Often, additional atrial substrate modification techniques are employed to improve success[4], however this increases procedure time and the optimal strategy is unknown[6].
Complex fractionated atrial electrograms (CFAE), defined as electrograms of short cycle length or continuous activity, are believed to associate with sources of AF perpetuation and CFAE ablation, as an adjuvant therapy to PVI, has been shown to improve maintenance of sinus rhythm (SR)[5,7-10] in some studies but not in others[6]. Contemporary electroanatomic mapping systems can generate automated maps to localize and quantify complexity of left atrial (LA) electrical activity using a number of signal processing techniques but chiefly the mean cycle length at any single point measured over a period of time[11]. The main limitation of this approach is that the majority of CFAE represent passive collision of wavefronts rather than critical drivers of AF[12] and differentiation of perpetuating from passive sites using current sequential mapping methods is speculative. Thus, currently all CFAE sites are targeted, potentially increasing procedure and ablation time without gain in efficacy.
Class III antiarrhythmic drugs (AAD) prolong the atrial refractory period[13], promote the fusion of fibrillatory wavefronts and decrease atrial fractionation[14]. It has been hypothesized that intraprocedural ibutilide may organize areas of passive atrial activation and help to identify CFAE sites critical for maintaining AF, thus reducing the amount of ablation required for success[15]. We investigated this potential in a cohort of long-standing persistent AF patients described herein.
In this descriptive, single-center cohort study we consecutively included adult patients (18 years of age or older) with long-standing persistent AF (sustained for more than 1 year) undergoing catheter ablation between April 2013 and June 2015. All patients had been referred due to symptomatic, drug-refractory AF. Patients with prior ablation procedures, patients who were in SR on the day of the procedure, and patients on amiodarone were excluded. Anti-arrhythmic medications other than amiodarone were discontinued 5 half-lives prior to the study. Therapeutic anticoagulation with warfarin or non-vitamin K oral anticoagulants (NOACs) was maintained for at least 4 weeks before the ablation procedure and a pre-procedural trans-esophageal echocardiogram was performed in all patients to exclude LA thrombus. The study group consisted of consecutive patients where the drug ibutilide was administered following trans-septal puncture, prior to mapping and ablation. The control group was matched for age, sex, and duration of AF and selected from consecutive patients prior to study commencement. There were no other interventions in that time frame and no change in operators. Only patients with a minimum follow-up of 12 months were considered. The study protocol was approved by the institutional ethics committee of Kingston General Hospital and all patients provided written informed consent.
The procedure was conducted in the fasting state under conscious sedation with intravenous fentanyl and midazolam. Warfarin was continued through the procedure whereas NOACs were stopped 48 h before the procedure and restarted 8 h after sheath removal. Venous access was gained from the right femoral and left subclavian veins or both femoral veins. A decapolar catheter (St. Jude Medical, St. Paul, MN, USA) was placed via the subclavian or left femoral vein into the coronary sinus, and a quadripolar catheter (St. Jude Medical, St. Paul, MN, USA) was placed at the right ventricular (RV) apex and moved to the right atrial (RA) appendage after trans-septal puncture to monitor RA mean cycle length. After establishing LA access, intravenous heparin was administered with a target activated clotting time of 300-350 s. Following this, a circular mapping catheter with 5 mm electrode diameter and 2-7-2 mm spacing (Reflexion, St. Jude Medical, St. Paul, MN, USA) and an open irrigated ablation catheter (Therapy Coolflex, St. Jude Medical, St. Paul, MN, USA) were advanced into the LA. The EnSite NavX system (St. Jude Medical, St. Paul, MN, USA) was employed to construct a three-dimensional LA geometry and create a subsequent map based on mean local cycle length over 5 seconds (CFE mean). Isoproterenol to disclose non-pulmonary vein (PV) triggers was not used and the administration of adenosine to unmask latent PV connection was left to discretion of the operator.
The test cohort was composed of patients with long-standing persistent AF deemed unlikely to cardiovert with medication alone. Therefore, an empiric dose of 1.0 mg of ibutilide was chosen to perturb atrial electrophysiology and allow subsequent data collection during continued AF before ablation. Based on our previous experience, this dose rarely results in AF termination in patients with long-standing persistent AF. In addition, some authors have suggested that a therapeutic dose of ibutilide may help discriminate patients in which PVI-alone may be enough from those requiring further substrate modification[16]. Intravenous ibutilide was administered over 10 minutes at the time of trans-septal puncture and before creation of the LA CFE mean map using commercial software (SJM Medical, MN).
CFE Mean Mapping and LA mCL
Before any ablation, a baseline mean cycle length (mCL) CFE mean map was created using the EnSite NavX automated algorithm. Mapping was started 5 minutes after ibutilide bolus completion. Bipolar electrograms were acquired with the 20-pole mapping catheter during a 5-second recording period at each sampled location (30-300 Hz). Color coding of the geometry guided sampling to ensure complete endocardial and pulmonary vein coverage. Areas with CFE mean < 120 ms were identified as CFAE based on previously published data[5,17]. Additional settings included: refractory period of 30 ms, width 5 ms, sensitivity between 0.05-0.08 mV and interior projection of 5 mm. Percentage of fractionation was calculated by summation of all areas with CFE mean <120 ms divided by the total mapped surface area using custom software.
The mCL of AF was measured manually from the mid-coronary sinus bipole after ibutilide administration and before ablation. In the control group measurement was made at the time of CFAE mapping.
Shannon entropy (ShEn) measures the distribution of signal values within the signal histogram and represents a measure of information uncertainty[8]. To investigate the effect of ibutilide we exported all 5-second bipolar electrograms recorded for creation of CFE mean map to the MATLAB environment and calculated a mean ShEn (bits) for each patient.
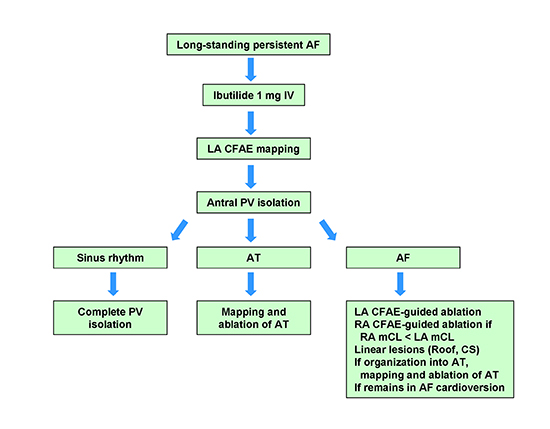
Radiofrequency (RF) ablation was performed using a 4-mm irrigated-tip ablation catheter (Therapy Coolflex, St. Jude Medical, St. Paul, MN, USA) at a power of 30W on the anterior wall and 25W on the posterior wall to minimize the risk of esophageal injury. A stepwise approach was used, starting with ibutilide (in the test cohort) and followed by circumferential antral ablation and isolation of all pulmonary veins, ablation of CFAE (areas of CFE mean <120 msec remaining after antral isolation) and linear lesions (roof, coronary sinus)[Figure 1] until AF terminated. Mapping and ablation was performed in the RA when the RA mCL exceeded the LA mCL measured periodically in the LAA. Linear lesions were performed at the roof and then coronary sinus if AF persisted after CFAE ablation and LA mCL was greater than RA mCL. The endpoint was local electrogram attenuation during AF (loss of fractionated components and reduction of mean amplitude) and bidirectional block at the roof after restoring SR. When AF terminated to an atrial tachycardia (AT) or flutter, subsequent ablation was guided by entrainment and/or activation mapping of the AT. If SR was achieved during ablation, no additional ablation was pursued, with the exception of additional lesions at the PV antrum in case of PV reconnection or additional lesions at the sites of existing linear lesions to obtain bidirectional block. If AF persisted despite extensive CFAE ablation and linear lesions, external cardioversion was performed
Figure 1 Stepwise approach for AF ablation in the ibutilide and control groups. AF = atrial fibrillation; AT = atrial tachycardia; CFAE = complex fractionated atrial electrograms; CS = coronary sinus; LA = left atrium; mCL = mean cycle length; PV = pulmonary vein; RA = right atrium.
Patients were discharged home on the day after the procedure. Antiarrhythmic medications were restarted post procedure and stopped at 3 months in the absence of symptoms. Patients were followed in the outpatient clinic at 3, 6 and 12 months post-ablation. Follow-ups included clinical assessment, 12-lead ECG and a 24-hour Holter; further monitoring was performed if patients reported symptoms. Recurrence was defined as any documented atrial arrhythmia lasting longer than 30 seconds and classified as AF or AT based upon ECG appearance.
Data were expressed as means and standard deviations for continuous variables and percentages for categorical variables. Independent samples t-tests and Fisher’s exact tests were used for comparison between the study and control groups. P values < 0.05 were considered statistically significant
Twenty-five consecutive patients with long-standing persistent AF were included in the study and compared with a matched cohort of consecutive patients treated prior to study commencement where ibutilide was not used. The clinical characteristics of the patients are summarized in [Table 1]. Both groups were comparable. The mean duration of persistent AF was 71.7±96.8 months and was not significantly different between the 2 groups. Most patients had severe LA dilatation, with a mean LA volume index by echocardiography of 50.7±25.4 ml (normal ≤41 ml). Five patients in the ibutilide group (20.0%) and 4 in the control group (16.0%) had a diagnosis of ischemic heart disease by coronary angiography.
Table 1. Baseline characteristics.
| Clinical variable |
Ibutilide |
Control |
p-value |
|
(n = 25) |
(n = 25) |
|
| Age, years ± SD |
66.8±8.9 |
64.4±7.8 |
0.32 |
| Male sex, % |
76.0 (19/25) |
72.0 (18/25) |
0.75 |
| Duration of AF, months |
63.2±102.5 |
78.9±93.8 |
0.63 |
| LA dimension, mm |
48.2±6.7 |
46.4±7.0 |
0.46 |
| LA volume, ml |
95.5±27.7 |
91.1±19.0 |
0.68 |
| LA volume index |
53.5±22.3 |
47.9±28.4 |
0.44 |
| Hypertension, % |
60.0 (15/25) |
56.0 (14/25) |
0.77 |
| Diabetes, % |
16.0 (4/25) |
16.0 (4/25) |
1.0 |
| Ischemic heart disease, % |
20.0 (5/25) |
16.0 (4/25) |
0.71 |
| OSA, % |
24.0 (6/25) |
28.0 (7/25) |
0.75 |
| CHADS VASc |
2.16±1.35 |
1.84±1.51 |
0.17 |
AF = atrial fibrillation; LA = left atrium; LVEF = left ventricular ejection fraction; IAB = interatrial block; OSA = obstructive sleep apnea.
Procedural Characteristics
The average procedure time in the ibutilide group was 288.8±49.6 min vs. 335.3±47.4 in the control group (p=0.002). The RF time was also lower in the ibutilide group (66.0±16.0 min vs. 78.0±18.2 min; p=0.029), while the fluoroscopy time did not differ significantly (25.3±9.7 min vs. 27.1±9.1 min; p=0.57). There was one cardiac tamponade requiring pericardiocentesis and one femoral pseudoaneurysm in the ibutilide group. There was also 1 episode of traumatic hematuria in the control group. No other major procedural complications were observed and no ventricular arrhythmias were associated with ibutilide use.
Table 2. Procedure characteristics and follow-up.
| Clinical variable |
Ibutilide |
Control |
p-value |
|
(n = 25) |
(n = 25) |
|
| Procedure time, min |
288.8±49.6 |
335.3±47.4 |
0.002 |
| Fluoroscopy, min |
25.3±9.7 |
27.1±9.1 |
0.57 |
| AF mCL, ms |
208.3±31.6 |
156.0±23.7 |
< 0.001 |
| CFAE, % |
29.2±20.2% |
47.3±13.7%; |
0.002 |
| AF termination, % |
88 (22/25) |
64 (16/25) |
0.047 |
| Conversion to AT, % |
68 (15/22) |
50 (8/16) |
0.26 |
| Recurrence (AF/AT): |
|
|
0.24 |
| - 6 m, % |
20.7% |
30.3% |
|
| - 12 m, % |
44% |
60% |
|
AF = atrial fibrillation; mCL = mean cycle-length; AT = atrial tachycardia.
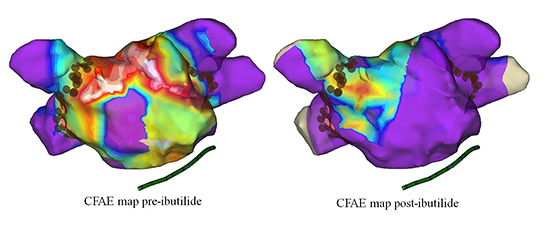
When compared with the control group, ibutilide was associated with a significant prolongation in AF mCL (208.3±31.6 ms vs. 156.0±23.7 ms; p<0.001) and decrease in the total CFAE surface area (29.2±20.2% versus 47.3±13.7%; p=0.002). To illustrate the effect of ibutilide, a CFE mean map was performed both before and after ibutilide administration and prior to ablation in one patient shown in [Figure 2 ].
Figure 2 CFAE mean maps of the LA before and after ibutilide administration in one of the study patients. A significant decrease in the CFAE surface area is noted. CFAE = complex fractionated atrial electrograms.
Patients administered Ibutilide had significantly reduced ShEn compared with control subjects (6.1±0.14 vs. 7.09±0.14; p<0.001). When we examined the ibutilide group for recurrence, ShEn was significantly higher in patient that recurred versus those that did not (6.47±0.24 vs 5.73±0.15; p<0.001). This was not observed in the control group (7.02±0.18 for recurrence vs 7.16±0.21 for no recurrence; p=0.14). A weak correlation was observed between CFAE surface area and mean ShEn (0.35; p=0.03).
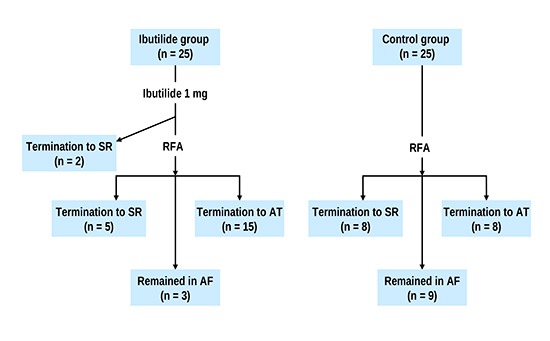
PVI was achieved in all the patients. In the ibutilide group conversion to SR directly or via organization into an AT was achieved in 88% of patients during ablation (n=22) (32% SR and 68% AT) [Figure 3]. In patients with an intermediate AT (n=15) the mechanism was perimitral in 4 cases, CTI-dependent in 4, roof-dependent in 1, focal in 1 (LA septum), both perimitral and roof-dependent circuits in 1, both perimitral and CTI-dependent in 1, both CTI-dependent and focal (LA anterior wall) in 1 and undetermined in 2 patients. In the control group AF termination during ablation was achieved in 64% of patients (n=16) (p=0.047 compared to the ibutilide group; 50% SR and 50% AT). The remaining patients (3 in the ibutilide group and 9 patients in the control group) remained in AF despite extensive ablation and were electrically cardioverted back to SR. Interestingly, conversion to SR before radiofrequency ablation occurred in 2 of the 25 patients in the ibutilide group (8.0%) and in these patients only PVI was performed. Both patients (age 83 and 69 years; AF duration 48 and 24 months) have remained arrhythmia-free after 12 and 14-month follow-up, respectively.
Figure 3 . Flowing chart showing the acute procedural outcomes in the ibutilide and control groups. AF = atrial fibrillation; AT = atrial tachycardia; RFA = radiofrequency ablation; SR = sinus rhythm
The mean follow-up in the whole cohort was 15.9±5.5 months (range 12 to 29 months), longer in the controls than in the study group (18.3±6.4 vs. 13.5±2.9 months; p <0.001) and the recurrence rate over this period was 44% (26/50). No significant difference was observed (p=0.24). The 6-month recurrence of atrial arrhythmias was 20.7% in the ibutilide group and 30.3% in the control groups and 1-year recurrence was 44% and 60%, respectively. In the ibutilide group 85% (6/7) of patients recurred with AF and 15% (1/7) with AT, whereas in the control group 66.5% (10/15) recurred with AF and 40% (5/15) with AT (p=0.27).
In the total group ablation failed to restore SR in 12 patients (24%). In these patients the likelihood of AF/AT recurrence was significantly higher than in those where SR was achieved (75.0 vs. 34.2%; p=0.013). Eleven of the 50 patients underwent a repeat ablation procedure.
In our study of patients with very long-standing persistent AF the use of ibutilide as initial part of a stepwise ablation approach resulted in higher rates of termination to SR and significantly shorter procedure times. In addition, there was an increase of AF mCL, reduction of LA fractionation and mean ShEn with ibutilide. Despite the less extensive ablation, the long-term outcomes were not impaired, with similar recurrence rates at 6 and 12 months, with a trend toward better outcomes in the ibutilide group.
Ibutilide fumarate is a class III intravenous antiarrhythmic agent that acts by induction of a late inward sodium current and blockage of the rapid component of the cardiac delayed rectifier potassium current[19],[20]. This ionic mechanism results in prolongation of the action potential duration and the effective refractory period of the cardiac myocytes. The dose of ibutilide used in our study, 1.0 mg, is equivalent to the therapeutic dose recommended for AF cardioversion[21]. In our patients, however, termination to SR by ibutilide before RF delivery was infrequent, occurring only in 2 cases (8%). This can be explained by the characteristics of our study group, with an average AF duration >6 years and severe LA dilatation (mean LA volume index 50.7 ml). In the 2 patients that converted to SR before commencement of RF, PVI alone was performed and both have remained free of AF/AT at 12 and 14-month follow-up. Ibutilide proved to be safe and was not associated with ventricular arrhythmias.
A recent randomized trial, the MAGIC-AF study, assessed the effect of a sub-therapeutic dose of ibutilide during ablation of persistent AF[22]. Consistent with our results, the study showed a reduction in LA surface area with CFAE sites and greater AF termination during ablation with ibutilide compared with placebo, while the 1-year freedom from AF did not differ significantly in both groups. The dose tested in MAGIC-AF, 0.25 mg IV, was selected to minimize the likelihood of AF termination. Other differences with our design can be acknowledged; in MAGIC-AF ibutilide infusion and CFAE mapping was carried out after PVI in patients who remained in AF, in our study the map was acquired prior to antral ablation. This is highly significant as mapping following ablation is compromised by atrial oedema and signal quality is usually poor. Finally, all persistent AF patients were included in MAGIC-AF, of which only 19% were long-standing[22]. As consequence, the duration of AF was much longer in our study (63.2 ± 102.5 months versus 9 ± 21 months).
CFAE mean index maps have important limitations in their ability to accurately identify the rotor pivot zones due to noise, misleading phase and activation times that distort these maps[23]. Other measures of signal complexity might be used instead. There is data in the literature to suggest that ShEn is a more reproducible feature[23], and Ganesan et al. showed the potential for ShEn to locate pivot points[18]. Ibutilide clearly reduced signal complexity as reflected by mean ShEn and a more marked effect was associated with better outcomes. We might infer this was due to a reduction in pivot points and thus signal complexity not associated with sources of AF. However we did not examine regional ShEn and the observation requires further study.
Optimal Ablation Approach for Long-Standing Persistent AF
Several studies indicate that long-term outcomes after catheter ablation of persistent AF are rather modest. The ablation endpoints in these patients are ill-defined and there is no consensus on the optimal ablation strategy. Current guidelines suggest that substrate modification (linear lesions, CFAE ablation or a combination of these strategies) in addition to PVI is mandatory to improve outcomes[24],[25]. A stepwise approach, involving PVI followed by CFAE-guided ablation and lines, may achieve acute termination in up to 87% of patients[26], but long-term results remain relatively poor and repeated ablation procedures are often necessary[27],[28]. In addition, this technique involves extensive substrate ablation, with long procedure times, increased complications and potential for arrhythmogenic circuits, with risk of recurrent ATs in the future.
In our study the acute benefits of ibutilide use as part of a stepwise ablation, included termination of AF in a great majority of patients (88%) and significantly less RF ablation, decreasing the need for electrical cardioversion from 36 to 12%. This may have 2 alternative interpretations: either ibutilide terminates AF prematurely and conceals substrate targets that should be otherwise eliminated; or ibutilide is able to eliminate “spurious” CFAEs and thus unmask critical drivers responsible for AF perpetuation. The fact that the outcomes in the ibutilide group were not worse despite the less extensive ablation supports the second hypothesis.
In the ibutilide group the most common mode of termination was via an intermediate AT. Of 18 ATs occurring in 15 patients, 78% were macroreentrant, with the most common mechanisms involving reentry around the tricuspid and mitral valves (6 each). The clinical importance of the ATs induced by ibutilide and the prognostic impact of ablating these circuits is unknown. However, some data suggest that, in general, ATs generated during substrate ablation may have a role in subsequent arrhythmia recurrence and their elimination has a positive impact on arrhythmia-free survival[29].
Survival free of AF/AT was 58% at 12-months and, despite higher rates of AF termination when ibutilide was used, the long-term outcomes were not significantly different in the 2 groups. However, this study was not powered or designed to detect a difference, merely examine the effect on a cohort with very long-standing AF. Regarding the mode of recurrence, patients in the control group tended to recur more often as macroreentrant rhythms (AT or flutter) than ibutilide patients in proportion. This did not reach statistical significance, but the tendency might reflect less proarrhythmic effect via reduction in ablation burden delivered in the ibutilide group.
Finally, when both groups were considered together, failure to terminate AF was a predictor of arrhythmia recurrence. This is compatible with a study by Scherr et al., which showed that termination of persistent AF by ablation was the strongest predictor of freedom of recurrence during follow-up[28].
Several limitations can be noted. First, there was no randomization and the comparison group consisted of a similar number of patients ablated without the use of ibutilide as an initial step. However, the primary operators did not change and both groups were consecutive and well balanced in term of clinical characteristics. The sample size was small and the study is underpowered to detect differences in long-term clinical endpoints. Finally, non-PV triggers were not pursued and adenosine not used routinely as the role of these agents in this group of very long lasting AF is unclear, with most studies in paroxysmal patients. The RA was not routinely mapped and guided by the mCL at the appendage. In the absence of more sophisticated tools, ablation of CFAEs in the RA adds little or no benefit versus cardioversion[30]. Finally, several technological advancements have occurred in the time since this study was performed, including improved stability of electroanatomic mapping systems and the availability of force sensing catheters (unavailable at the time of this study). It is possible that the addition of these may have altered the results, however the role of contact force remains debated[31].
In patients with very long-standing persistent AF, stepwise catheter ablation results in good success rates. Ibutilide administration as part of a stepwise approach results in higher rates of termination to SR, more often through an intermediate AT. Procedure and RF times are significantly decreased with a trend toward better long-term outcomes.