Right Ventricular Pacing for Assessment of Cavo-Tricuspid Isthmus Block
Ganesh Venkataraman, MD, Marc Wish, MD, Ted Friehling, MD, S. Adam Strickberger, MD
INOVA Heart and Vascular Institute, Electrophysiology, INOVA Fairfax Hospital, Fairfax, VA.
Cavo-tricuspid isthmus (CTI) dependent atrial flutter is typically treated with cardiac ablation. Standard techniques to assess CTI block after ablation can be technically challenging. Right ventricular (RV) pacing may allow for another technique to assess CTI block after ablation.
The purpose of this study was to evaluate RV pacing as a method to assess CTI block after ablation of CTI dependent atrial flutter, and define endpoints of ablation using this technique.
28 patients undergoing ablation of CTI dependent atrial flutter with intact ventriculoatrial (VA) conduction were prospectively enrolled in this study and underwent the RV pacing protocol, as well as standard coronary sinus (CS) pacing techniques to assess CTI block.
The mean trans-isthmus conduction interval during CS pacing (TICICS) at 600 and 400ms after CTI ablation was 168 +/- 9ms and 175 +/- 18ms, respectively. The mean trans-isthmus conduction interval during RV pacing (TICIRV) at 600ms and 400ms after CTI ablation was 109 +/- 5ms and 111 +/- 5ms, respectively. A TICIRV >100ms was associated with a successful outcome after CTI ablation.
RV pacing may add incremental value in the assessment of CTI block in patients undergoing ablation of CTI dependent atrial flutter.
Key Words : Atrial Flutter Ablation, Cavo-Tricuspid Isthmus, Right Ventricular Pacing, Bidirectional Block.
Correspondence to: Ganesh Venkataraman, 3020 Hamaker Court, Suite 101, Fairfax, VA 22031.
Typical atrial flutter dependent on the cavo-tricuspid isthmus (CTI) is a common arrhythmia frequently treated with radiofrequency (RF) ablation.1,2 Bidirectional CTI block is the standard endpoint for ablation of atrial flutter.3 Methods to assess bidirectional CTI block, including changes in electrogram (EGM) polarity, measurement of trans-isthmus conduction interval (TICI), and an interval between double potentials (DPs) > 110ms along the ablation line can be difficult to assess.4-6 Right ventricular (RV) pacing has been shown to be helpful in assessing CTI block, but this technique has not been validated and specific endpoints to determine CTI block have not been defined.7 The purpose of this study was to evaluate the utility of RV pacing in patients undergoing ablation for CTI-dependent atrial flutter and to define specific endpoints associated with bidirectional CTI block.
A total of 33 consecutive patients who underwent radiofrequency (RF) catheter ablation of CTI-dependent atrial flutter were prospectively enrolled in this study. Patients were excluded from the study if they were under 18 years of age, pregnant, or had undergone a previous CTI ablation. Patients without ventriculoatrial (VA) conduction, identified during the ablation procedure, were subsequently excluded. The protocol was approved by the Medstar Institutional Review Board. Patients provided written informed consent for all procedures.
Atrial Flutter Ablation: Study Protocol
Sedation was provided by electrophysiology (EP) laboratory nursing staff or an anesthesiologist. Access was obtained via the right femoral vein. A 7F deflectable duo-decapolar catheter (Boston Scientific, San Jose, CA; M004 20SL22025 with 2/20/2/2/2/2/2/2/2/2/2/2/2/25/2/25/2/25/22/2/2mm spacing) was positioned around the tricuspid annulus (TA) in the right atrium (RA) with the distal electrode pair (RA 1-2) placed in the coronary sinus (CS) ostium. Electrode pair RA 3-4 was located lateral to the planned CTI ablation line (Figure 1). Through an 8F 60cm sheath (St. Jude Medical, St. Paul, MN; RAMP, 406898), a 10mm RF ablation catheter (Boston Scientific, San Jose, CA; Blazer II XP, M004 4790THMK20) was positioned on the CTI. A 5F quadripolar catheter (St. Jude Medical, St. Paul, MN; M0045404S0) was positioned in the RV apex (Figure 1).
Figure 1. Anteroposterior (left) and left anterior oblique (right) fluoroscopic views of intra-cardiac catheter placement during atrial flutter ablation. The radiofrequency ablation catheter is placed along the cavo-tricuspid isthmus (CTI). The distal tip of the duo-decapolar catheter is placed in the coronary sinus ostium (CSO). The quadripolar catheter tip is placed in the right ventricular apex (RVA)
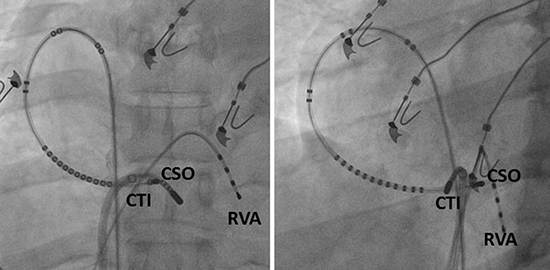
Patients presented to the EP laboratory in either sinus rhythm or atrial flutter. Patients in atrial flutter underwent pacing with concealed entrainment to confirm CTI dependence of the atrial flutter.1 Patients in atrial flutter were cardioverted to sinus rhythm with a 200J synchronized shock. RV pacing was performed to ensure intact retrograde VA conduction.
Once in sinus rhythm, pacing at two different cycle lengths (600ms and 400ms) from the CS ostium and RV apex was performed. When pacing from the CS ostium, the trans-isthmus conduction interval (TICICS) was measured from the pacing stimulus to the local EGM on the pair of electrodes of the duo-decapolar catheter (RA 3-4) located immediately lateral to the planned ablation line on the CTI. When pacing from the RV apex, the trans-isthmus conduction interval (TICIRV) was measured from the local EGM on the distal electrode pair (RA 1-2) of the duo-decapolar catheter located at the CS ostium to the pair of electrodes (RA 3-4) located immediately lateral to the planned ablation line on the CTI.
The TICIRV after CTI ablation was the primary endpoint. Secondary endpoints included the TICICS, differences in TICICS and differences in TICIRV pre- and post CTI ablation, as well as differences in TICICS and differences in TICIRV when pacing at two different cycle lengths.
All patients were followed until hospital discharge. At one month, patients were evaluated for symptoms at an office visit, and an ECG was obtained. A Holter or event monitor was performed if symptoms suggested recurrent atrial flutter.
28 patients undergoing atrial flutter ablation were included in the analysis. Five patients were excluded due to the absence of retrograde VA conduction during RV pacing, which is required for this diagnostic maneuver. Continuous data were expressed as the mean +/- standard deviation. Univariate comparisons were performed on all continuous variables with either unpaired T test or analysis of variance, as appropriate. Categorical variables were compared with Chi-square analysis. All statistical analyses were performed using SAS version 9.1 (SAS Institute, NC). A p value < 0.05 was considered statistically significant.
Twenty-eight of 33 (84.9%) patients undergoing ablation of CTI dependent atrial flutter had intact retrograde VA conduction and were included in this analysis. The mean age was 60.7 +/- 15.0 years. The mean left ventricular ejection fraction was 0.50 +/- 0.16. Of 28 patients, 17 (60.7%) presented to the EP laboratory in atrial flutter and underwent cardioversion at the time of the procedure. Among these 17 patients, the atrial flutter cycle length was 255 +/- 33ms (Table 1).
Table 1. Baseline clinical characteristics of patients undergoing atrial flutter ablation
| Variable |
Mean +/- STD |
| Age (years) |
60.7 +/- 15.0 |
| Male sex (%) |
78.6 |
| BMI (kg/m2) |
31.2 +/-7.6 |
| Diabetes (%) |
39.3 |
| Hypertension (%) |
89.3 |
| Coronary disease (%) |
25.0 |
| Prior CVA (%) |
17.9 |
| Ejection Fraction (%) |
49.7 +/- 15.8 |
| Medications (%) |
|
| Aspirin |
53.6 |
| Beta-blocker |
67.9 |
| ACE-I/ARB |
57.1 |
| Warfarin |
17.9 |
| Anti-arrhythmic |
10.7 |
ACE-I = angiotensin converting inhibitor, ARB = angiotensin receptor blocker, BMI = body mass index, CVA = cerebral vascular accident
Electrophysiology Findings During CS Pacing Before And After CTI Ablation
The mean TICICS with a paced cycle length of 600ms pre- and post-ablation was 42 +/- 5ms (range 20-50ms) and 169 +/- 9ms (range 150-220ms; p < 0.01), respectively. The mean TICICS with a paced cycle length of 400ms pre- and post-ablation was 47 +/- 9ms (range 25-65ms) and 175 +/- 18ms (range 150-225ms; p = 0.01), respectively. The difference between TICICS pre- and post- ablation was 126 +/- 9ms with a paced cycle length of 600ms, and 139 +/- 25ms with a paced cycle length of 400ms (p = 0.08). A change in the pattern of activation across the lateral RA wall during CS pacing was noted post CTI ablation and was consistent with CTI block in all patients.
Electrophysiology Findings With RV Pacing Before And After CTI Ablation
The mean TICIRV with a paced cycle length of 600ms pre- and post-ablation was 31 +/- 4ms (range 20-50ms) and 109 +/- 5ms (range 100-140ms; p < 0.01), respectively (Figures 2 and 3). The mean TICIRV with a paced cycle length of 400ms pre- and post-ablation was 34 +/- 9ms (range 20-60ms) and 111 +/- 5ms (range 100-125ms; p < 0.01), respectively. The difference between TICIRV pre- and post- ablation was 79 +/- 8ms with a paced cycle length of 600ms, and 79 +/- 12ms with a paced cycle length of 400ms (p = 0.8). A change in the pattern of activation across the lateral RA wall during RV pacing was noted post CTI ablation and was consistent with CTI block in all patients.
Figure 2. The trans-isthmus conduction interval during right ventricular pacing (TICIRV) was measured pre-ablation of the cavo-tricuspid isthmus (CTI). Surface ECG leads I, II, and V1 and intra-cardiac electrograms from an ablation catheter placed on the CTI (ABLd-ABL p), a duodecapolar catheter placed on the right atrium (RA) septum, to the cristae, and around the tricuspid annulus with the distal tip in the coronary sinus ostium (RA 19-20 to RA 1-2), and a quadripolar catheter placed in the RV apex (RVp-RVd) are shown. RV pacing pre-ablation of the CTI with an atrial activation sequence consistent with isthmus conduction and a TICIRV interval of 30ms, as measured between paired electrodes RA 1-2 and RA 3-4, is shown
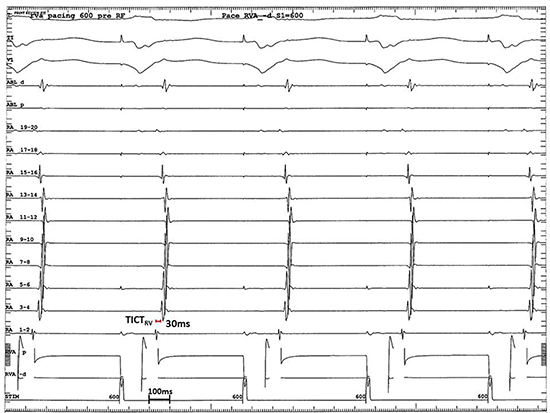
Figure 3. The trans-isthmus conduction interval during right ventricular pacing (TICIRV) was measured post-ablation of the cavo-tricuspid isthmus (CTI). The tracings are arranged as in Figure 2. RV pacing post-ablation of the CTI with an atrial activation sequence consistent with complete isthmus block and a TICIRV interval of 115ms is shown
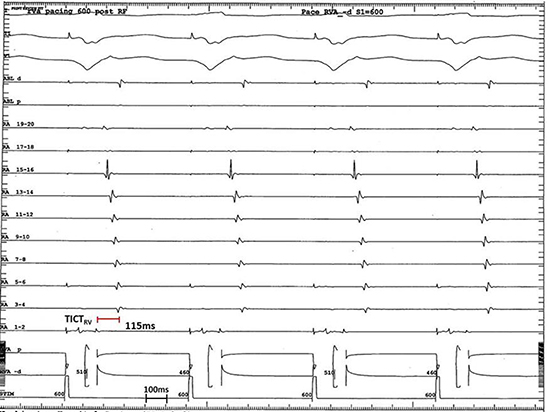
Short And Mid-Term Outcomes Post CTI Ablation
Bidirectional CTI block was achieved in all 28 patients. No complications were observed. The mean follow up was 8.1 +/- 6.6 months. There were no recurrences of atrial flutter.
The major finding of this study is that RV pacing during ablation of CTI dependent atrial flutter is an important adjunctive tool in the assessment of CTI block. More specifically, a TICTRV > 100ms is associated with successful CTI ablation.
Ablation of CTI Dependent Atrial Flutter: Previous Studies
CTI dependent atrial flutter is a common arrhythmia, and RF ablation is first line therapy. In early studies, CTI dependent atrial flutter ablation was performed with a 4mm tip RF ablation catheter.1-3 However, subsequent studies observed improved outcomes with CTI ablation with 8mm and 10mm tip RF ablation catheters.8-9
Methods to assess CTI block after ablation include measurement of the TICICS, and presence of DPs along the ablation line.4-6 DPs represent the measurement of local activation on both the medial and lateral sides of the CTI ablation line, and are likely the most accurate near-field assessment of CTI conduction. The current method to assess DPs relies on pacing from the proximal CS while recording DPs with an ablation catheter along the length of the CTI ablation line. An interval between DPs > 110ms has been associated with bidirectional CTI block.6 Challenges with this technique include poor stability of a catheter in the coronary sinus, unreliable capture of the atrial tissue, and inaccurate measurement of the first component of the split potential due to pacing artifact. Data regarding the utility of DPs have come from studies using a 4mm tip RF ablation catheter.6,10-11 Larger 8mm and 10mm tip RF ablation catheters, functionally, have a larger “antenna” and lead to greater destruction of local tissue; both of which can prevent visualization of one or both components of the DPs along the ablation line.
The TICICS is defined as the interval between the stimulus artifact and the local atrial activation recorded from the pair of electrodes positioned on the CTI just lateral to the ablation line. This method relies on pacing from the proximal CS. An increase in TICICS >50% has been associated with complete CTI block).12 Although an absolute measurement of TICICS has not been found to be associated with complete CTI block, a TICICS 150-180ms or greater is generally an acceptable target after CTI ablation.12 TICICS may overestimate the frequency of CTI block due to latency between CS pacing and atrial capture, and may be unable to discriminate complete block from incomplete block with very slow conduction. As with the measurement of DPs, TICICS also requires stable capture of the atrium from the distal tip of the duo-decapolar catheter positioned in the CS ostium. Hence, methods to assess CTI block with CS pacing have limitations.
Comparison of TICIRV with Previous Endpoints
Right ventricular (RV) pacing overcomes these challenges of coronary sinus pacing, allows for stable and reliable pacing, eliminates the issue of latency with atrial capture, and provides an accurate measurement of TICIRV; hence, it is helpful in assessing CTI block. Previous studies have shown that RV pacing can aid in the assessment of CTI block, but have not provided specific endpoints for ablation.7
In the current study, we defined TICIRV as the interval between the distal pair of electrodes on the duo-decapolar catheter located at the CS ostium and the pair of electrodes positioned on the CTI just lateral to the planned ablation line. Once CTI block is achieved, the distance between the medial and lateral electrodes is slightly shorter with the TICIRV as opposed to that of DPs, where the medial and lateral potentials are recorded on the CTI ablation line. Therefore, it is expected that with CTI block, less time is required to inscribe the medial and lateral electrodes with TICTRV than when recording DPs. In the current study, a TICIRV >100ms after ablation of CTI dependent atrial flutter is shorter than the duration expected with DPs, i.e., > 110ms,6 and was associated with excellent outcomes.
RV pacing to assess CTI block has at least three limitations. First, patients without intact retrograde VA conduction cannot utilize RV pacing in the assessment of CTI block. In this study, this occurred 15% of the time and the use of RV pacing was precluded. Isoproterenol may have improved VA conduction and allowed for the use of RV pacing in the assessment of CTI block, but was not administered to patients in this study. Second, DPs were not measured during RV pacing. Electrophysiologically, this is likely the gold standard to assess bidirectional block. However, DPs are difficult to assess after CTI ablation with a 10mm tip RF ablation catheter. Third, data regarding partial but not complete CTI block was not collected. However, a comparison of the TICIRV before and after the achievement of complete CTI block was performed, and as expected, was slightly less than DPs. Finally, lateral RA pacing was not performed pre- and post-CTI ablation to confirm true bidirectional block. However, after CTI ablation, unidirectional block is not common.
Data evaluating the use of RV pacing as a method to assess CTI block during ablation of CTI dependent atrial flutter have been limited. RV pacing allows for accurate assessment of TICIRV along the CTI ablation line. These results demonstrate that a TICIRV >100ms is associated with excellent outcomes after ablation of CTI dependent atrial flutter, and should be considered for verification of bidirectional CTI block.