S. Serge Barold MD, FHRS1, Bengt Herweg MD, MD, FHRS2
1Clinical Professor of Medicine Emeritus, Department of Medicine, University of Rochester School of Medicine and Dentistry, Rochester, New York.2Professor of Medicine and Director of the Arrhythmia Service, University of South Florida College of Medicine and Tampa General Hospital, Tampa, Florida.
Atrial fibrillation (AF) occurs in one of four patients undergoing cardiac resynchronization therapy (CRT).-Without special therapy, the prognosis of AF patients with CRT has been generally worse than those in sinus rhythm. The importance of a high percentage of biventricular pacing (BIV%) was confirmed in a large study where the mortality was inversely associated with BIV% both in the presence of normal sinus and atrial paced rhythm and with AF. The greatest reduction in mortality was observed with BIV% >98%. Patients with BIV% >99.6% experienced a 24% reduction in mortality (p < 0.001) while those with BIV% <94.8% had a 19% increase in mortality. The optimal BIV% cut-point was 98.7%. This cutoff would appear mandatory but it would be best to approach 100%. Careful evaluation of device interrogation data upon which the BiV% is based is essential because the memorized data can vastly overestimate the percentage of truly resynchronized beats since it does not account for fusion and pseudofusion between intrinsic (not paced) and paced beats. The recently published randomized CERTIFY trial provides unequivocal proof of the value of AV junctional (AVJ) ablation in CRT patients with AF. This trial confirmed the favorable results of AVJ ablation by many other studies and two important meta-analyses and therefore established the firm recommendation that the procedure should be performed in most, if not all, patients with permanent AF as well as those with frequent and prolonged episodes of paroxysmal AF. Patients after AVJ have improved mortality with a mortality similar to those in sinus rhythm. The AVJ ablation procedure carries the theoretical risk of device failure and death in pacemaker dependent patients. An inappropriate first ICD shock for AF seems to increase mortality. Increased long-term mortality after an inappropriate shock may be due to the underlying atrial arrhythmia substrate as opposed to the effect of the shock itself.
Key Words : Atrial Fibrillation, Cardiac Resynchronization, B Iventricular Pacing, Ablation Of Atrioventricular Junction, Implantable Cardioverter Defibrillator.
Correspondence to: Dr. S. Serge Barold, MD, FHRS.
Rochester, New York.
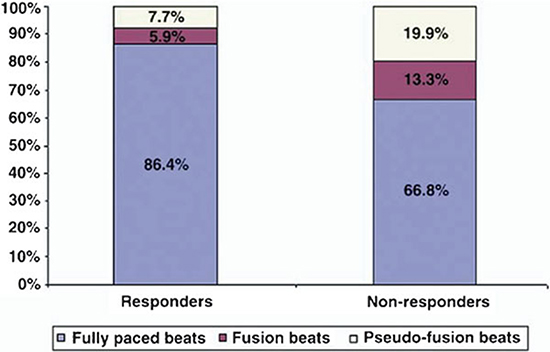
The major randomized controlled trials that demonstrated the efficacy of cardiac resynchronization therapy (CRT) excluded patients with atrial fibrillation (AF). Yet, AF occurs in one of four recipients of CRT.1-2 The prognosis of AF patients with CRT is generally worse than that of patients in sinus rhythm.3-4 because they are at a major disadvantage.5 They exhibit loss of atrioventricular synchronicity, a higher risk for insufficient CRT delivery because of uncontrolled ventricular rates, more ICD shocks for ventricular arrhythmia, inappropriate ICD shocks, inadequate symptomatic improvement, repeated hospitalization and increased mortality.6-17 Furthermore AF may be associated with fusion and pseudofusion beats that represent inefficient biventricular capture fig 1.18-19 Such beats render the pacing counters inaccurate for assessing true biventricular capture beats. AF represents an important cause of poor long-term CRT benefit and prognosis unless aggressive efforts are made to slow the ventricular rate. The new developments in rate control can now promote the delivery of a high percentage of biventricular paced beats to the AF patient (which was challenging in the past) so as to produce an overall response virtually similar to that seen in patients with sinus rhythm despite the persistence of atrial arrhythmia.
Figure 1 24-hour Holter data for cardiac resynchronization therapy (CRT) responders and non-responders with permanent AF. CRT responders had a higher percentage of fully paced beats than non-responders. Non-responders to CRT had a significantly higher percentage of ineffective pacing because of a combination of fusion and pseudo-fusion beats (Reproduced with permission from reference.18)
Contemporary CRT devices are equipped with reliable and extensive diagnostic and memory features yielding full disclosure of the number, duration, and overall burden of atrial tachyarrhythmias. These advanced diagnostic features have demonstrated the high frequency of symptomatic and asymptomatic AF and atrial arrhythmias in CRT patients with heart failure (HF). Because the overwhelming majority of atrial tachyarrhythmias consist of AF, we shall refer, as do many workers, to atrial tachyarrhythmias simply as AF.15-17,20 Some arrhythmias stored in an implanted device may not be true AF but rather atrial tachycardias or atrial flutters with rates that exceed the programmable recording threshold. In AF the loss of atrial transport function and associated tachycardia frequently result in deterioration of cardiac function and clinical outcome. AF compromises CRT delivery due to RR interval variability and competing tachycardia, and may even result in excessive rapid ventricular pacing during atrial tracking. Arrhythmia occurrence must be confirmed by examining stored electrograms to rule out problems such as intermittent undersensing, far-field R wave sensing by the atrial channel, and electromagnetic interference. Because of intermittent atrial undersensing, a single prolonged episode may be recorded as multiple shorter episodes so that the overall arrhythmia burden may be more reliable than the number of episodes.
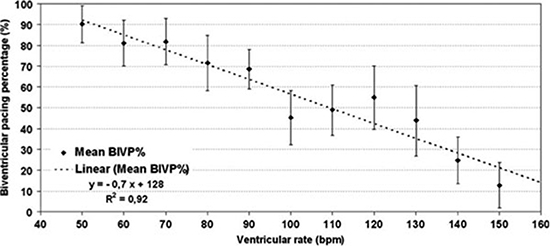
Figure 2 The percentage of effective biventricular pacing (BiVP%) during atrial fibrillation decreases linearly as a function of the ventricular rate. The faster the ventricular rate, or the shorter the R-R interval, the less biventricular pacing was present. (Reproduced with permission from reference.21 )
Device interrogation also provides estimates of the percentage of biventricular (BIV%) pacing in CRT patients, a measurement of the utmost importance in achieving a satisfactory clinical response.18-19 Other important data from implanted devices include the ventricular rate during atrial tachyarrhythmias and stored electrograms that permit the precise diagnosis of the atrial tachyarrhythmia (e.g. AF versus atrial flutter versus atrial tachycardia) and characterize the initiation/termination of arrhythmias. The AF burden calculated from the recordings in terms of total time in AF during a specific period is sometimes called the “electrocardiographic” AF burden. This burden can be further subdivided into total time in AF, the number of AF (re)occurrences in a specific period or duration of the AF-free period until the recurrence of AF, or a combination of these. AF burden is a more accurate assessment of AF than the time to the first recurrence of AF.
Incidence and Prognosis of Atrial Fibrillation During Cardiac Resynchronization Therapy
Device based continuous monitoring of AF in CRT patients has improved the diagnosis and therapy of AF in this group of patients.7 The bulk of our knowledge regarding the role of CRT in patients with permanent AF is based on non-randomized, observational data. AF and heart failure have much in common and frequently coexist. AF is independently associated with a worse outcome in heart failure. Marijon et al16 analyzed the incidence of AF in CRT patients in a prospective study and found that 34 out of 173 (27.5%) patients developed paroxysmal AF during a follow-up of 9.9 ± 3.6 months. About half of the AF patients had a past history of AF. Boriani et al21 evaluated 1404 CRT patients for a median follow-up of 18 months. All were in sinus rhythm at the time of entry into the study. AF was documented in 443 out of 1404 patients (32%). The duration of AF ranged from > 10 min to weeks. AF developed in 222 CRT patients without a previous history of AF (22%) and 221 CRT patients with a previous history of AF (16%). The observations of Leclercq et al17 involving 120 CRT patients followed for a mean of 183 ± 23 days showed an AF incidence of 21%. A previous history of AF was present in 29% of patients and those with new-onset AF after CRT constituted 17% of all the patients. Thus, the incidence of AF in patients with heart failure treated with CRT ranges from 30 – 35% for paroxysmal AF and around 20–25% for permanent AF. This should not be surprising given the association of AF with the severity of HF heart failure. This association carries a worse prognosis than HF with sinus rhythm.
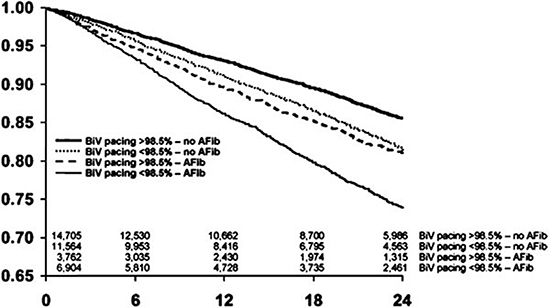
Figure 3 In a large cohort of 36,935 patients followed up in a remote-monitoring network (LATITUDE Patient Management system) a high percentage of biventricular (BiV) pacing achieved, specifically >98.5%, was associated with a reduction in mortality. As expected, patients with atrial fibrillation (AF) had a worse outcome than those without AF. However, this was lessened if the high percentage of BiV pacing could be achieved in the AF population, usually after an atrioventricular junction ablation (Reproduced with permission from reference.24)
Boriani et al21 found in their AF population that age (p = 0.046), and uncontrolled VR (p = 0.028) were the only independent predictors of clinical outcome assessed by the combined end-point of HF hospitalizations or death. In a study involving 1193 CRT patients (initially all in sinus rhythm) Santini et al18 found AF in 361 patients (30%) over a mean follow-up of 13 month (The study overlapped that of Boriani et al21). Among 882 patients with no previous history of AF, 20% developed new-onset AF. The end point of deaths or hospitalizations occurred in 174 patients (14.6%). AF (especially persistent AF) was significantly correlated with the composite end point of death and HF hospitalization (p = 0.005).
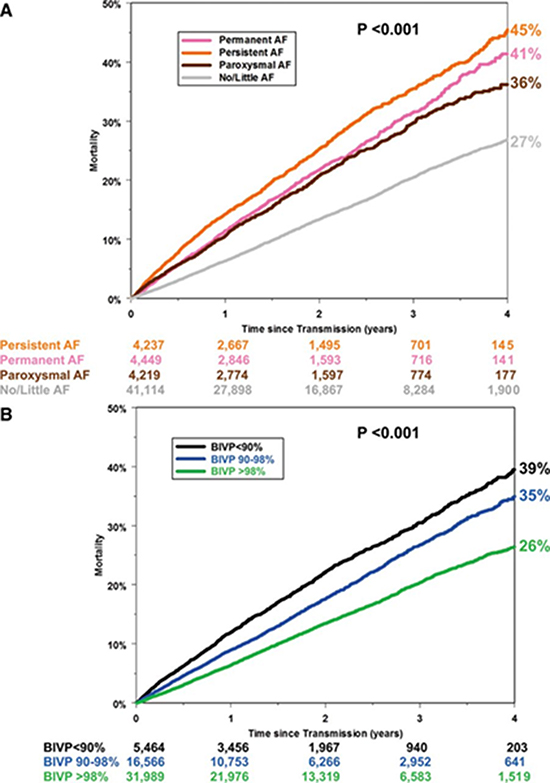
Figure 4 The epidemic of inadequate biventricular pacing in patients with persistent or permanent atrial fibrillation. Unadjusted mortality. A, Atrial fibrillation (AF) classification groups. B, Biventricular pacing (BIVP%) groups. See text for details. (Reproduced with permission from reference.26)
Prognostic data was also obtained in a recent subanalysis of the MADIT-CRT trial where the cumulative probability of both the combined end point of HF or all-cause mortality was higher among patients who developed atrial tachyarrhythmia during the first year.22
Importance of The Percentage of Biventricular Pacing: More is Always Better
In the study of Boriani et al22 the percentage of biventricular pacing (BIV%) in the AF group was 95% vs. 98% in the entire patient population. When patients with AF were in sinus rhythm the BIV% was 98% vs. 71% during AF, p < 0.01). Suboptimal CRT was defined as BIV% < 95% which was predicted by the occurrence of persistent or permanent AF (P < 0.001), and uncontrolled ventricular rate (P = 0.002). BIV% was inversely correlated to the ventricular rate (VR) in AF decreasing by 7% for each 10 bpm increase in VR fig 2.
Koplan et al23 conducted a retrospective analysis in 1800 of CRT patients to evaluate the significance of BIV% and its relationship to a combined clinical end point of death and heart failure hospitalization. Patients that showed a BIV% >92% had a 44% reduction in clinical end points compared with subjects with BIV% 0–92% (p < 0.00001). Subjects with BIV% 98% to 99% had similar outcomes as the subjects with BIV% 93–97% and also similar outcomes as subjects paced 100% of the time. Subjects with a history of atrial arrhythmias were more likely to pace ≤ 92% (p < 0.001).
The importance of a high BIV% has recently been confirmed in a large cohort of 36,935 patients who participated in the US LATITUDE patient Management System in which the patients were followed in a remote monitoring network.24 The mortality was inversely associated with BIV% both in the presence of normal sinus and atrial paced rhythm and with AF fig 3. The greatest reduction in mortality was observed with BIV% >98%. Patients with BIV% >99.6% experienced a 24% reduction in mortality (p < 0.001) while those with BIV% <94.8% had a 19% increase in mortality. The optimal BIV% cut-point was 98.7%.
It is important to remember that the delivery of a stimulus does not guarantee effective CRT. The percentage of BiV pacing based on device interrogation data vastly overestimates the percentage of truly resynchronized beats since it does not account for fusion and pseudofusion between intrinsic (not paced) and paced beats. Kamath et al18 utilized 12 lead Holter monitoring to assess the incidence of ineffective capture in19 AF patients undergoing CRT fig 1. The study clearly demonstrated that although device interrogation showed >90% BiV pacing only 9 patients (47%) received effective BiV pacing. It is imperative to examine rhythm strips and electrocardiograms of non-responders to verify that the beats are truly resynchronized. Importantly, certain device algorithms aimed at maximizing biventricular pacing in AF patients with a relatively fast ventricular rate may also lead to a false sense of reassurance about the percentage of BiV pacing.
Importance of the Percentage of Biventricular Pacing in Patients in Sinus Rhythm
Ruwald et al25 estimated the threshold of BIV pacing percentage percentage needed for CRT-D (D = implantable cardioverter-defibrillator, 699 patients) to be superior to ICD (no D, 520 patients) on the end-point of HF or death in patients from the Multicenter Automatic Defibrillator study. The study was comprised of individuals with depressed LV function, prolonged QRS durations, and New York Heart Association class I or II HF symptoms in sinus rhythm. No difference was seen in the risk of heart failure/death between ICD and CRT-D patients with BIV pacing ≤90%, and BIV pacing exceeding 90% was associated with a benefit of CRT-D in HF/death when compared with ICD patients. Furthermore, BIV pacing ≥97% was associated with an even further reduction in HF/death, a significant 52% reduction in death alone, and increased reverse remodeling. CRT-D with BIV ≥97% was associated with a significant 52% reduced risk of death alone, when compared with ICD patients, and a 63% risk reduction when compared with CRT-D patients with BIV pacing <97%. Within the CRTD group, for every 1 percentage point increase in BIV pacing, the risk of HF/death and death alone significantly decreased by 6 and 10%, respectively. Increasing BIV pacing percentage was associated with significant reductions in LV end-systolic volume. Interestingly a past history of supraventricular tachyarrhythmias did not influence the results.
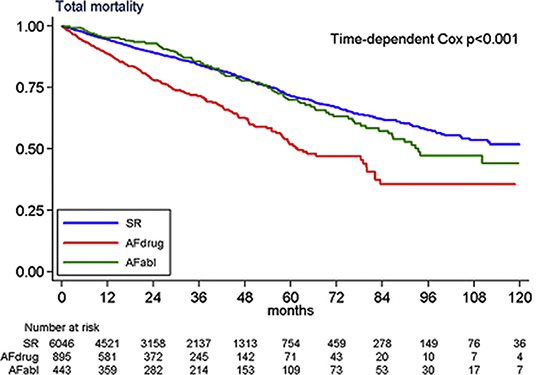
Figure 5 CERTIFY trial. Kaplan-Meier survival after cardiac resynchronization therapy (CRT) from total mortality for the 3 patient groups: sinus rhythm (SR) (blue lines); atrial fibrillation (AF) plus drugs (red lines); and AF plus ablation (green lines). (Reproduced with permission from reference.14)
Uncontrolled Ventricular Rates
A ventricular rate (VR) in AF controlled at rest may not be associated with rate control during exercise. Furthermore, pronounced RR interval variability in AF may decrease the number of resynchronized beats. In a study in 2011 when the benefit of AVJ ablation was already being appreciated, Boriani et al21 calculated the average VR of each patient at 115 ± 15 bpm In an AF group of 443 patients. An uncontrolled VR occurred in 150 of 443 (34%) of the patients. In the AF patients with new-onset AF after CRT, 93 of 222 patients (42%) were found to have uncontrolled VR while in those with a known history of AF before CRT, 43 of 221 patients (26%) exhibited uncontrolled VR (p = 0.001). An uncontrolled VR which occurred in about one-third of CRT patients was associated with a worse clinical outcome of combined heart failure, hospitalization or death (p = 0.046).
The Epidemic of Inadequate Biventricular Pacing
In a study evaluating inadequate biventricular pacing, CRT defibrillator patients were classified as permanent (daily mean AF burden ≥23 hours), persistent (≥7 consecutive days of AF ≥23 hours/d), paroxysmal (≥1 day with AF ≥6 hours), or no/little AF (all others) using device-detected AF during the 6 months postimplant fig 4.26
Subsequent all-cause mortality was evaluated using a multivariable Cox proportional hazard regression. Among 54 019 patients, 8% of patients each had permanent (N=4449), persistent (N=4237), and paroxysmal AF (N=4219). A high proportion of patients with permanent (69%) and persistent (62%) AF did not achieve high BIV% (>98%).25 Relative to patients with BIV % >98%, patients with reduced BIVP had increased mortality after adjusting for age, sex, AF, and shocks (90%–98%: hazard ratio=1.20 [1.15–1.26]; P<0.001; <90%: hazard ratio=1.32 [1.23–1.41]; P<0.001). High BIVP% was associated with the greatest mortality improvement in permanent AF among the AF classifications. Nearly half (47%) of the patients with persistent AF had <90% BIV% during AF. High BIV% (> 98%) was not achieved in two thirds of 8686 patients with persistent or permanent AF, and these patients had an increased risk of death independent of each other and age, sex, or ICD shocks.25
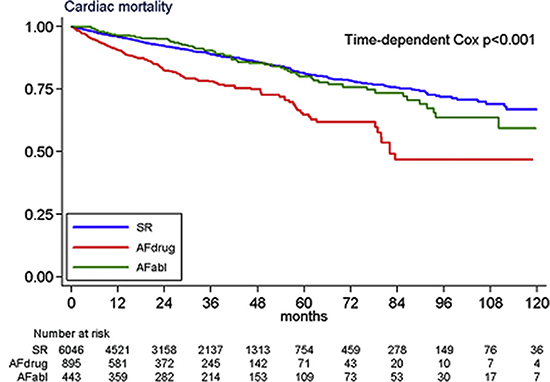
Figure 6 CERTIFY trial. Kaplan-Meier survival after cardiac resynchronization therapy (CRT) from total mortality for the 3 patient groups: sinus rhythm (SR) (blue lines); atrial fibrillation (AF) plus drugs (red lines); and AF plus ablation (green lines). (Reproduced with permission from reference.14)
Analysis of the RAFT Study in Patients with Permanent Atrial Fibrillation: Suboptimal Dose of Cardiac Resynchronization?
The results of the Resynchronization for Ambulatory Heart Failure Trial (RAFT AF) study were published in 2012 and constitutes to date the largest, randomized report examining the role of CRT in patients with permanent AF27 The findings were disappointing, contrary to prevailing belief that AF patients improve with CRT though somewhat less than in patients in sinus rhythm. The RAFT AF study illustrates the importance of BIV%. The RAFT study enrolled 1788 patients with a follow-up of 40 ± 18 months. Healy et al randomized all the 229 patients with permanent AF (12.7%) and compared 115 patients who received only an ICD vs. 114 patients who received a CRT device and an ICD (CRT-D device). Patients with permanent AF were required to have a resting heart rate of ≤60 beats per minute and ≤90 beats per minute after a 6-minute walk test to be eligible for the study. All patients received optimal medical therapy. Only 1 patient had an AV junction ablation before or within 6 months after randomization. During the first 6 months after randomization, there were 34.3% of CRT-treated patients with ≥95% biventricular pacing and 47.1% with biventricular pacing ≥90% of the time. There was no statistically significant difference in the risk of or those receiving <95% ventricular pacing versus ≥95% (P=0.65) reaching a composite endpoint of all-cause deaths or hospitalization for heart failure receiving <90% ventricular pacing versus ≥90% or those receiving <95% ventricular vs. ≥95% . The study demonstrated a strong trend toward a 42% decrease in heart failure hospitalizations with CRT, closely missing statistical significance with a P value of 0.052.
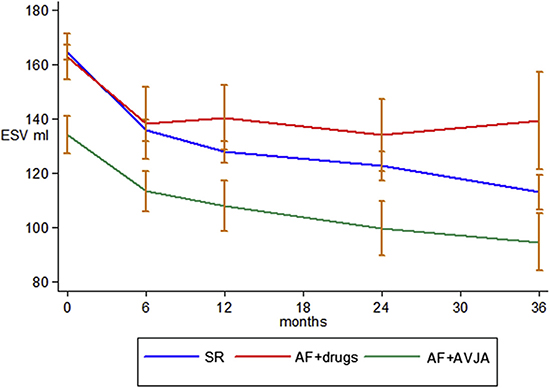
Figure 7 CERTIFY trial. Left Ventricular Reverse Remodeling after cardiac resynchronization (CRT). Progression in left ventricular end-systolic volume (ESV) after therapy CRT throughout the 3-year follow-up for the 3 groups: sinus rhythm (SR) (blue line); atrial fibrillation (AF) plus drugs (red line); and AF plus atrioventricular junction ablation (AVJA) (green lines). (Reproduced with permission from reference.14)
Only one third of CRT patients in the RAFT trial received ≥95% ventricular pacing during the first 6 months. Even this may bean overestimate, because Holter monitoring studies have shown that, when device logs indicate ≥90% ventricular pacing inpatients with permanent AF but without AV junction ablation, 53% of these paced beats are actually fusion or pseudofusion. Furthermore, the CRT-ICD arm had the conducted AF response algorithm (Medtronic) enabled. This feature regularizes the pacing rate by adjusting the pacemaker escape interval after each ventricular beat. In this way the delivery of biventricular pacing was enhanced at a rate that closely matches the relatively fast spontaneous ventricular rate. Therefore the BiV% may have been overestimated in the CRT-D patients. The investigators of the RAFT AF study indicated that their data suggests that the standard medical rate control of permanent AF in RAFT was not sufficient to allow effective delivery of CRT therapy. The potentially misleading conclusions of the RAFT trial were forcefully and correctly challenged by Gasparini and Boriani.28
Control of The Ventricular Rate and Need For Ablation of The AV Junction
Many reports have emphasized that the control of the ventricular rate with AV blocking drugs is difficult and often yield suboptimal results. During AF one must not rely solely on the pacemaker counters to determine the percentage of biventricular pacing because of prevailing fusion and pseudofusion beats liable to produce an inaccurate count of true bipolar capture beats. It seems reasonable to start with pharmacologic therapy to optimize rate control in AF patients requiring CRT. When after careful clinical evaluation including device interrogation, repeated Holter monitoring, and exercise testing, the amount of “true” biventricular pacing is suboptimal, atrioventricular node ablation should be considered. The limiting value of suboptimal pacing has gradually increased so that ≥ 95% may no longer be acceptable.24
AV junctional (AVJ) ablation should be considered in all CRT patients when AF engenders a fast ventricular rate despite adequate doses of AV nodal active drugs or when such drugs are not tolerated or when antiarrhythmic medications are ineffective or call contraindicated.
The importance of achieving 100% BIV pacing by AVJ ablation was first highlighted by Gasparini et al in 2006.7 They demonstrated that permanent AF patients (48 subjects) treated with negative dromotropic drugs and receiving biventricular (BIV) pacing as high as 88% (considered at that time ‘adequate’) fared poorly compared to AF patients (114 subjects) treated with CRT and AVJ ablation in whom the global effective CRT dose approached 100% effective BIV pacing. This study showed that only those AF patients who had undergone AVJ ablation developed significant improvements in left ventricular (LV) ejection fraction, LV end-systolic volume, and exercise capacity. Furthermore, a significantly higher proportion of responders (response defined as a ≥10% reduction in LV end-systolic volume relative to baseline) were observed in the AVJ ablation group (68%) compared with the non-ablated group (18%) at 12 months.
Gasparini et al.8 in 2008 presented more extensive data on 1285 consecutive CRT patients (1042 in sinus rhythm, 243 (19%) in AF). Of the 243 AF patients, 125 underwent rate control with drug therapy. Those with > 85% BIV pacing were continued with rate control (BIV > 85% pacing was considered as “sufficient” CRT delivery at the time but is no longer considered as satisfactory as discussed later). The other 118 AF patients underwent AVJ ablation for inadequate BIV capture during follow--up defined arbitrarily as < 85% BIV capture. At a median follow-up of 34 months, all-cause mortality and cardiac mortality was similar in the sinus rhythm group and the AF group.
In the above study, the long-term total mortality was statistically lower in the AVJ-ablation group with11 deaths out of 118 patients during pacing 98.7 ± 1.8% of the time, compared to the AF group in the drug-treated group with28 deaths out of 125 patients The difference was mostly due to a reduction of deaths from progressive HF which was 4.3 in the ablated AF group vs. 15.2 per 100 person-year in the drug-treated AF group (p < 0.001).
The beneficial role of AVJ ablation in AF patients has been confirmed by others.29-32 However, a few small studies claim that conservative therapy without AVJ ablation produces results similar to those seen after AVJ ablation.32-38 Finally, the recently published randomized CERTIFY trial provided unequivocal proof of the value of AVJ ablation in CRT patients with AF.14
The study was conducted because no randomized controlled trial of CRT had addressed whether CRT confers similar benefits on AF patients (25% of CRT patients) with or without AVJ ablation (A despite the high prevalence of AF in the patient population undergoing CRT. The trial compared clinical outcomes of patients with permanent AF undergoing CRT combined with either AVJ ablation (A) (n = 443) or rate-slowing drugs [(AF+drugs = 895] to outcomes in patients who were in sinus rhythm (n = 6,046).14 The study found that after median follow-up of 37 months: all-cause mortality (6.8 vs 6.1 per 100 person year) and cardiac-related mortality (4.2 vs 4.0) were similar in patients with AF+AVJA and in patients who were in sinus rhythm (both p = not significant). In contrast, the AF+ drugs drugs group had a higher rate of total and cardiac-related mortality than both the sinus rhythm and the AF+AVJA groups (11.3 and 8.1, respectively; p<0.001) fig 5 and 6. The authors also reported that on multivariable analysis the AF plus AVJA group had a total mortality (Hazard ratio [HR]: 0.93, 95% confidence interval CI 0.74-1.67) and cardiac mortality (HR: 0.88, 95% CI 0.66-1.17) similar to the sinus rhythm group, independent of known confounders. The AF+ drugs group, however, had a higher total mortality (HR: 1.52, 95% C.I. 1.26-1.82) and cardiac mortality (HR: 1.57, 95% C.I. 1.27-1.94) mortality than both the sinus rhythm and AF+AVJA groups (both p<0.001). The AF+AVJA group was associated with 52% lower mortality than the AF+drug group, independent of age, sex, etiology of heart failure, New York Heart Association class, device type, LV ejection fraction (LVEF), and QRS duration. The investigators concluded that long-term survival after CRT in patients with AF+AVJA is similar to that observed in patients in sinus rhythm. Mortality is higher in AF patients treated with rate-slowing drugs.
All 3 patient groups namely, the AF+AVJA, AF +drugs, and sinus rhythm groups showed improvements in LVEF at 6 months. The increase in LVEF observed in the AF+AVJA and sinus rhythm groups was higher than that observed in the AF+drugs group (p < 0.001 and p ¼ 0.003, respectively). Similarly, the 3 groups showed a reduction in LV end-systolic volume (LVESV) at 6 months (all p < 0.001). Although there was no further reduction in LVESV after 6 months in the AF+drugs group, the reduction in LVESV for the sinus rhythm group and AF+AVJA group was sustained over the 3-year follow-up. The difference in LVESV between the AF+AVJA group and AF+drugs group increased from 25 ml at 6 months to 50 ml at 3 years (p < 0.001) fig 7.
The mean biventricular pacing percentage was significantly higher in the AF+AVJA group (96±6%) than in the AF+drugs group (87±14%; p < 0.001); this difference in all likelihood played an important +role in the different mortality observed in these 2 groups
The results of the CERTIFY trial confirmed the findings of 2 meta-analyses39-40 that had suggested that in CRT patients with AF, AV junctional ablation is associated with a reduction in all cause-mortality, compared with rate-slowing drugs. One of the meta-analyses ablation showed a substantial reduction in all-cause mortality (risk ratio 0.42) and cardiovascular mortality (risk ratio 0.44) and improvements in New York Heart Association functional class (risk ratio 0.52), compared with CRT without AV junctional ablation. Based on these results, organizational guidelines now emphasize the importance of AV junctional ablation for the control of ventricular rate in CRT patients with AF(Class IIa, Level of evidence: B). According to the ESC, a lower level of evidence (Class IIb, Level of Evidence C belongs to CRT for patients with atrial fibrillation. treated with rate-slowing drugs.
The impressive results following AVJ ablation suggests that the procedure should be performed in most, if not all, patients with permanent AF as well as those with frequent and prolonged episodes of paroxysmal AF. With regard to timing, some cardiologists have suggested the use of routine AVJ ablation at the time of CRT implantation and others prefer to do it 1 month later after verification of proper device function or even later if reverse LV remodeling has occurred.
There are no reports of increased mortality associated with AVJ ablation. The procedure carries the theoretical risk of device failure and death in pacemaker dependent patients. Following ablation, attempts at restoring sinus rhythm in selected patients should not be abandoned because restoration of AV synchrony in HF is superior to AF with a controlled biventricular paced rate.
Organizational Guidelines for Cardiac Resynchronization
The 2010 European Society of Cardiology (ESC) guidelines state that “there is consensus that essentially complete ventricular capture is mandatory in order to maximize clinical benefit and improve the prognosis of patients with permanent AF. This often requires creation of complete heart block by ablation of the AV junction given the frequently inadequate efficacy of pharmacological treatment of ventricular rate control at rest and during exercise.”41 Frequent pacing was defined as BIV% ≥95% in 2010, but it is now defined as 98%. The 2012 ESC state that the routine use of AV junction ablation ensures adequate biventricular pacing in patients with AF.42 Such patients are considered as eligible to receive CRT with a Class II a indication with the added specification of AV nodal ablation.” AF patients with LVEF≤35%, heart failure with an intrinsic QRS ≥120ms and who remain in NYHA functional class III and ambulatory IV despite adequate medical treatment are classified as a class IIa provided BiV pacing is achieved as close to 100% as possible.
The 2012 American College of Cardiology/American Heart Assocation/ Heart Rhythm Society (ACC/AHA/HRS) guidelines state that the prospective experience among patients with permanent AF and with decreased LV systolic function suggests that benefit may result from biventricular pacing when the QRS duration is ≥120 ms, although it may be most evident in patients in whom atrioventricular nodal ablation has been performed such that right ventricular pacing is obligate.43 Thus, the 2012 ACC/AHA/HRS guidelines indicate that CRT can be useful in patients with AF and LVEF less than or equal to 35% on guideline-directed medical therapy if a) the patient requires ventricular pacing or otherwise meets CRT criteria and b) AV nodal ablation or pharmacologic rate control will allow near 100% ventricular pacing with CRT. (Level of Evidence: B).
The 2012 guidelines certainly did not consider AVJ ablation as controversial. The class IIa indication for CRT in the guidelines is probably based on the incorporation of relatively few AF patients in the major CRT trials and the lack of large randomized trials guideline-directed medical therapy comparing patients in sinus rhythm with those in AF. We believe that AF should now be a class Ia indication for CRT based on the favorable impact of AVJ ablation and our better understanding of rate control and the importance of aiming for the highest percentage of biventricular pacing.
Implantable Cardioverter-Defibrillators
AF is the most common cause of inappropriate shocks in CRT patients and is related to a baseline history of AF. AF is associated with an increased risk of appropriate and inappropriate defibrillator therapy and is an independent risk factor for mortality.44-46 AF also causes an increased risk of heart failure deterioration. Appropriate shocks are related to AF may be an expression of a poor cardiac function, but this relation could also be due to a reduced amount of biventricular pacing during periods of paroxysmal or persistent AF with subsequent less electrical remodeling. This could not only lead to mortality, but also result in a higher frequency of ventricular arrhythmias and consequently of appropriate shocks. Powell et al44 found that no mortality risk was associated with an inappropriate first shock such as “benign rhythms” (sinus tachycardia or supraventricular tachycardia) or nonarrhythmia events (noise, artifact, and oversensing). This group had similar survival to those who did not receive a shock. Although some workers have claimed that inappropriate shocks were not associated with increased mortality, Powell et al found that an inappropriate first shock for AF/A flutter increased mortality. These data suggest that increased long-term mortality after a shock is due to the underlying arrhythmia as opposed to the shock itself.
Fisher et al47 found that the most powerful programmable variable associated with shocks was the detection rate threshold. A detection threshold of 167 bpm was associated with an increase in shocks, independent of other variables. This is consistent with previous reports demonstrating that lower 1-year inappropriate shock rates occur when utilizing detection thresholds of 181 to 188 bpm as compared with detection thresholds of 150 to 170 bpm. More complex algorithms have been recently developed to produce a marked reduction of inappropriate shocks due to AF.48
Impact of Structural Changes on the Development of Atrial Tachyarrhythmias During Cardiac Resynchronization
The change in the left atrial volume and incidence of atrial tachyarrhythmias was evaluated in a substudy of the MADIT-CRT trial.22 In the total population of 1820 patients there were 139 patients with atrial tachyarrhythmis (AF 47%). A low left atrial volume (LAV) reduction was defined as a <20% and a high LAV reduction as ≥20%. Based on the 1 year follow- up echocardiographic data, the mean percent reduction of LAV was 3-fold higher in patients treated with a CRT-D (D = ICD) device compared to the ICD-only group. The median reduction in LAV was 29% (20 – 30%) in the CRT-D group versus 10% (5 – 14%) in the ICD-only group (p < 0.001). As expected, reduction in LAV was highly correlated with reduction in the LV end-systolic volume.
The cumulative probability of atrial tachyarrhythmias (at 2.5 years) in MADIT-CRT was lowest among high LAV responders to CRT-D (3%) and significantly higher among both low LAV responders to CRT-D (9%) and ICD-only patients (7%; p = 0.03 for the difference among the 3 groups). Multivariate analysis showed that high LAV responders experienced a 53% reduction in the risk of subsequent atrial tachyarrhythmias compared to low LAV responders in the CRT-D group and patients in the ICD-only group (p = 0.01).
The potential influence of CRT on the risk of new-onset AF or a beneficial effect of CRT on the burden of paroxysmal AF remains unknown but CRT is associated with conversion of persistent or permanent AF to sinus rhythm in a minority of patients.
Atrial High Rate Episodes
Shanmugam et al49 conducted a trial of 560 patients with CRT prospectively followed for a mean of 370 days, using remote monitoring technology. The study defined atrial high rate episode (AHRE) as an atrial rate >180 pulses/minute and included patients with and without a prior history of AF. The investigators did not adjudicate individual AHRE, but defined them as significant if they were documented for at least 1% of any day or 14 minutes. Thromboembolic complications developed in 2% of patients and were nine times more likely to develop among patients who had ≥3.8 hours of AHRE detected during any day.
However, patients with AHRE < 3.8 hours/day still had a trend toward an increased risk of thromboembolism, with a hazard ratio of 4.3, P= 0.11. The ASSERT study did not demonstrate a strong temporal relationship between AHRE and thromboembolic events. The median interval between the most recent prior AHRE and the thromboembolic complication was 47 days and only 27% of patients with AHRE who suffered a thromboembolic complication were in AF at the time of that event. This is in keeping with the TRENDS trial50 (Is There a Critical Value of Daily Atrial Tachyarrhythmia Burden From Device Diagnostics That Raises Stroke Risk?) which found that in patients with AHRE and a thromboembolic event, only 30% were in AF at the time of the event, and in the remaining patients, the most recent AHRE was an average of 168 ± 199 days earlier.50 This challenges our traditional understanding of the relationship between AF and stroke.
Witt et al51 recently reported an observational study of patients who received CRT and no history of AF. They were screened for early detected AHREs longer than 6 minutes occurring before 6-month follow-up, and the longest duration of AHREs was recorded.51 Of 394 eligible patients, 79 patients (20%) had early AHRE detected. During a median follow-up of 4.6 years, patients with early detected AHREs had an increased risk of clinical AF (HR 2.35; 95% CI 1.47-3.74; P < .001) and thromboembolic events (HR 2.30; 95% CI 1.09-4.83; P = .028). For patients with AHREs longer than 24 hours, these associations were stronger. The risk of mortality was not higher with early detected AHREs (HR 0.97; 95% CI 0.64-1.45; P = .87). Of the 27 patients with thromboembolic events, only 10 patients (37%) had AHREs detected within a 2-month period before the thromboembolic event. Therefore detection of early AHREs after CRT is associated with a significantly increased risk of clinical AF and thromboembolic events.
At this time, the critical duration, rate, and definable burden of AHRE or AF associated with a significant risk of a stroke that would warrant anticoagulation remain unknown though patients with a CHADS 2 or CHA2DS2-VASc score should be strongly considered.52 AHRE monitoring may help us understand more about the natural history of AF by revealing the circumstances predictive of progression from asymptomatic to symptomatic AF and the transition from paroxysmal to sustained AF. Such data may become useful in the future. Although there appears to be a strong association between AHRE and stroke, more data are needed before routine oral anticoagulation. Can be recommended. Randomized trials of anticoagulation with respect to AF burden and frequency of AHRE are needed.
Return Of Sinus Rhythm. Implantation Of An Atrial Lead
Gasparini et al53 indicated that about 10% of CRT patients with permanent AF revert to sinus rhythm spontaneously mostly in the first year but late reversion even at 5 years is possible. These workers identified 4 predictors of reversion: 1. Smaller LV end-diastolic diameter, shorter QRS duration after CRT, smaller left atrial diameter, and AVJ ablation. Patients with 3 predictors had a 60% likelihood of spontaneous reversion and those with 3 predictors had a 25% chance of reversion. Patients with the spontaneous return of sinus rhythm showed an 87% reduction in mortality after 1 year. Gasparini et al49 suggested that implantation of an atrial lead should be considered at the time of CRT implantation. The parameters suggesting a favorable atrial response might be useful in determining which patients are likely to respond to various therapies aimed at restoring sinus rhythm.53,54
Conversion to Sinus Rhythm
Rhythm control should be considered in selected patients with persistent symptoms attributable to AF. The parameters defined by Gasparani et al53 to predict the spontaneous return of sinus rhythm after CRT could also be used to predict a favorable response to therapies used to restore sinus rhythm. Cardioversion of permanent AF should be considered in the first 3 – 6 months particularly in patients demonstrating significant LV remodeling.55 There are no official guidelines about drug therapy, cardioversion or AF ablation (excluding the AV junction) in patients with CRT devices. There are no data about the role of pulmonary vein isolation in in CRT patients with AF.56 Ongoing trials may provide data about this potentially important procedure.56
AF in CRT patients is associated with an increase in heart failure hospitalizations and death mainly because uncontrolled ventricular rates reduce the delivery of an optimal “dose” of BiV pacing. ICD shocks in AF may be contributory. Although the ventricular rate in AF can be controlled with drugs in some patients, AV junctional ablation is now the preferred choice especially on the basis of the recent CERTIFY trial. AV junctional ablation permits CRT delivery close to 100% of the time with regularization of the RR intervals, elimination of fusion and pseudofusion beats and discontinuation of some AV nodal blocking drugs. Patients who have undergone AV junctional ablation derive as much benefit from CRT as patients in sinus rhythm provided the ventricular rate is controlled by AV junctional ablation. It is incumbent on the physician to achieve the highest possible BiV% pacing because prognosis depends on it. The greatest mortality reduction in CRT patients with AF occurs with BIV% pacing ≥ 97-98%. One should always aim for a BIV% pacing of 100%. More is better and small gains in BIV% pacing are important. The latest organizational guidelines recommend a class IIa indication for CRT in patients with AF and a controlled ventricular rate that may require AV junctional ablation. The guidelines should now show CRT in AF as a class 1a indication for CRT in patients with a controlled ventricular rate that virtually always requires AV junctional ablation.