Atrial Fibrillation In Athletes: Pathophysiology, Clinical Presentation, Evaluation and Management
Mohit K, Turagam MD, Greg C, Flaker MD, Poonam Velagapudi MD, Sirisha Vadali MD, Martin A, Alpert MD
From the Division of Cardiovascular Medicine University of Missouri- School of Medicine, Columbia, Missouri, USA.
Atrial fibrillation (AF) is the most common cardiac arrhythmia in athletes, especially in middle-aged athletes. Studies have demonstrated that athletes who engage in endurance sports such as runners, cyclists and skiers are more prone to AF than other athletes. The effects of exercise on the onset and progression of AF is complex. Triggers of AF in athletes may include atrial ectopy and sports supplements. Substrates for AF in athletes include atrial remodeling, fibrosis, and inflammation. Modulators of AF in athletes include autonomic activation, electrolyte abnormalities, and possibly, gastroesophageal reflux. Management of AF in athletes with rate-controlling agents and antiarrhythmic drugs remains a challenge and can be associated with impaired athletic performance. The value of catheter ablation is emerging and should be considered in suitable athletes with AF.
Key Words : Atrial Fibrillation, Athletes, Exercise, Pathophysiology, Evaluation, Management.
Correspondence to: Dr. Martin A. Alpert,
Room CE-338
University of Missouri
Health Sciences Center
5 Hospital Drive
Columbia, MO 65212.
Atrial fibrillation (AF) is the most common cardiac arrhythmia in athletes, especially in middle-aged athletes.1 Participation in regular physical exercise has been shown to be beneficial to cardiovascular health and overall well-being.2-5 However, recent studies have demonstrated that long-term endurance exercise increases the risk of AF, both in athletes training at a competitive level and in individuals who participate in vigorous exercise at a non-competitive level6-24, Table 1. The effects of exercise on the onset and progression of AF is complex and remain unclear with some studies also demonstrating no increased risk of AF with exercise.25-31 This review focuses on the pathogenesis, clinical presentation, evaluation and management of AF in athletes.
Type of Sport and Atrial Fibrillation
Studies have demonstrated that athletes who engage in endurance sports such as runners, cyclists and skiers are more prone to AF than other athletes.15-18,22,23,32 The exact mechanism involved remains unclear as other athletes who participate in boxing, wrestling, weight-lifting also practice strenuous sport practices, but AF does not appear to be as prevalent in those groups. The question remains – is this related to the type of sport? Unfortunately, little information exists relating to AF risk and sport specificity. Further research is warranted in this area.
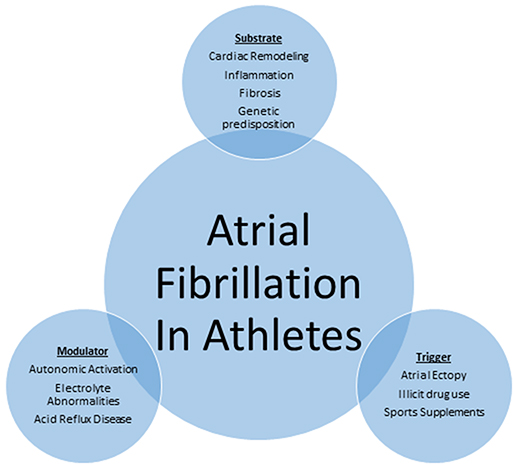
The mechanisms by which exercise contributes to AF are not well understood and are presumed to be multifactorial Figure 1. It is accepted that the initiation and perpetuation of AF requires a trigger, a modulator and a substrate. The mechanism of AF in athletes may be attributable to the interaction among these three factors. A specific trigger (atrial ectopy, sports supplements and illicit drug use) in the presence of a suitable substrate (genetic predisposition, inflammation, fibrosis and cardiac remodeling) and a modulator (autonomic activation, electrolyte abnormalities, acid reflux disease) remains the foundation in onset and maintenance of AF in athletes.
AF is commonly-triggered by focal ectopic discharges within the four pulmonary veins at the left atrial junction.33 It has been postulated that increased sympathetic activity when participating in vigorous exercise can trigger atrial ectopy. However, this concept lacks convincing evidence.13,17,34
Figure 1 Schematic representation of mechanism of atrial fibrillation in athletes
A study of 134 professional Swiss athletes and non-athlete controls reported no significant increase in the frequency of isolated atrial ectopic beats (18/62 versus 17/62, p=0.35), despite a significant increase in the frequency AF or atrial flutter (p=0.028) on a 24 hour electrocardiographic monitor.17
Sports supplements are commonly-consumed by individuals who exercise regularly and indulge in athletic activities, even at a non-competitive level.
Professional athletes occasionally use illicit or performance enhancing drugs, which are not approved by the World Anti-Doping Agency (WADA), to improve performance Table 2.35 Anabolic steroids, when associated with competitive sports, has garnered the most attention from media and the public. Increased risk of AF associated with anabolic steroids has been reported in young athletes in isolated case reports.36,37 There are no systematic data regarding risk of anabolic steroids in the initiation of AF.
Energy drinks have recently gained popularity with young adults participating in competitive and non-competitive sports.38 Energy drinks contain high levels of caffeine (50 mg to 500mg),38 stimulants such as taurine, guarana, ginseng, and vitamins such as riboflavin, pantothenic acid and thiamine.39 Isolated cases of cardiac arrhythmias, including AF with heavy consumption of energy drinks have been recently reported.38,40 The potential explanation being genetic susceptibility exaggerated by autonomic modulation from high dose caffeine or other ingredients which may trigger AF.
We currently lack objective data on the electrocardiographic effects of energy drinks. One study reported that heavy consumption of energy drinks in healthy individuals can contribute to a transient increase in both blood pressure of 10 mmHg and heart rate of 5-7 beats/minute.41 However, long-term data concerning the risk of chronic consumption of energy drinks, especially in middle aged individuals who also have other medical comorbidities in triggering AF are lacking.
There is ample evidence that endurance exercise is associated with both bi-atrial and ventricular enlargement which can occur independent of each other.8 Left atrial size of >4.0 cm was noted in 20% of athletes who participated in competitive sports.42 Mont and colleagues reported increased left atrial longitudinal, anteroposterior and transverse diameters and volumes [46.5 ± 17.2 vs 34.6 ± 10.0, p<0.001] with exercise.19 Atrial enlargement is reported to be related to the lifetime hours of exercise.43
Several population studies have demonstrated increased risk of new-onset AF with increased left atrial enlargement.44,45 However, the role of left atrial remodeling in athletes as a predictor of AF is speculative with no clear evidence. A study of 492-marathon runners with a mean age 42±7 years reported that total higher lifetime hours of training was associated with left atrial enlargement and subsequently higher risk of AF (24% in < 1500 hours, 40% 1500-4500 hours and 83% in > 4500 hours).13
Despite increased left atrial size in athletes, one study reported lower left atrial stiffness compared to controls (0.13 ± 0.04 vs. 0.16 ± 0.06, p≤0.01).46 Another study stratified subjects based on lifetime training as low (<1500 hours), intermediate (1500-4500 hours) and high (>4500 hours). This study reported an increase in left atrial volume (30±5, 33±5 vs. 37±6 ml/m,2 p<0.001), but no effect on atrial mechanical function (pump strain -15.0±2.8, -14.7±2.7 vs. -14.9±2.6%, p=0.92 and conduit strain 23.3±3.9, 22.1±5.3 vs. 23.7±5.7%, p=0.455) measured by two-dimensional echocardiographic speckle track imaging.47
The role of fibrosis in exercise induced-AF mostly from animal models. Sixteen weeks of exercise in Wistar rats substantially increased fibrosis marker expression including fibronectin-1, transforming growth factor-β1, matrix metalloproteinase-2, tissue inhibitor of metalloproteinase-1, procollagen-I, and procollagen-III in the atria and ventricles when compared to controls. Furthermore, exercise cessation reversed fibrosis eight weeks after exercise cessation.48
Another study in a similar rat model confirmed the above findings concerning the role of cardiac fibrosis with endurance training by noting an increase in protein major profibrotic markers and messenger RNA synthesis. The study also reported that pretreatment with losartan 50 mg/kg/day reduced all markers of fibrosis.49
The role of TNFα-dependent activation of both NFκB and p38MAPK with exercise was recently described in rat models as an underlying mechanism of exercise induced atrial remodeling and AF.50 However, further research is necessary to examine this mechanism.
Table 1. Selected Controlled Studies of the Prevalence of AF in Athletes
| Study Type |
Number of subjects |
Age/Gender |
Type of exercise |
Prevalence of AF in athletes/controls (%) |
| Karjalainen et al15 |
795 |
35-39 years/ Male |
Cross country Running |
5.3/0.9 |
| Baldesberger et al17 |
196 |
~66 years/ Male |
Cyclists vs. golfers |
10/0 |
| Mont et al8 |
216 |
<65 years/ Male + Female |
Endurance athletes |
63/15 |
| Elosua et al16 |
109 |
41-55 years/ Male |
Endurance athletes |
32/14 |
| Heidbuchel et al22 |
|
60 years/83% Male, 17% Female |
Cycling, running, or swimming |
|
| Molina et al18 |
557 |
48 years |
Marathon runners vs. sedentary |
5/0.7 |
| Grimsmo et al11 |
78 |
54-62 years- Group I 72-80 years- Group II 87-92 years- Group III |
Cross-country runners, skiers |
12.8 |
Another study including 45 veteran elite athletes and controls demonstrated biochemical evidence of myocardial fibrosis. Markers of collagen turnover including tissue inhibitor of matrix metalloproteinase type I (350 vs. 253 ng/ml, p=0.01); plasma carboxyterminal propeptide of collagen type I (PICP 259 vs. 166 microg/l, p<0.001) and carboxyterminal telopeptide of collagen type I (CITP 5.4 vs. 2.9 microg/l, p<0.001) was demonstrated in veteran athletes when compared to sedentary controls.51
In another study including twelve veteran male endurance athletes with a mean age 56±6 years reported that 50% (6/12 athletes) demonstrated evidence of myocardial fibrosis by late gadolinium enhancement (LGE) on cardiac magnetic resonance imaging (CMR). No LGE was demonstrated in sedentary controls. Number of years spent in training (p<0.001) and participation in number of competitive marathons (p<0.001) predicted prevalence of LGE on CMR.52 Further research is necessary to evaluate the role of cardiac fibrosis with exercise.
The role of inflammation as a substrate in AF is speculative and controversial. Several studies have shown an association between AF and elevated CRP (C-reactive protein).53,54 Swanson et al hypothesized that excessive training can induce chronic systemic inflammation which may induce high CRP levels that may lead to atrial electrical remodeling and development of AF. Atrial remodeling can be treated with anti-inflammatory drugs.55 Limited research has demonstrated increased activation of interleukin-6, TNF-α and interleukin beta-1 in induction and maintenance of AF.56
Several studies have investigated the role of autonomic activation on AF.12,13,57 AF in athletes is predominantly vagal-mediated.2 Increased vagal tone initiates AF by creating macro-reentry pathway by increase in the dispersion of the atrial refractory period.58 Most athletes have a lower resting heart rates which was also a predictor of AF in a study of long-term endurance cross country skiers.11
Vagal mediated AF is different from adrenergically-mediated AF which is more commonly seen in the elderly with diseased hearts. Vagal-mediated AF is typically associated with macro-reentry circuits, whereas adrenergically-mediated AF is associated with micro-reentry circuits.59
Higher vagal tone was reported in non-elite athletes who participate in regular exercise. A study reported significantly higher vagal tone in non-elite athletes with higher lifetime training hours (>4500 hours versus <1500 hours, 47±16ms vs 34±13ms, p=0.002)].13
Mechanistic insight concerning the pathogenesis of AF with exercise comes from animal models. Gausch et al reported that AF duration increased significantly (AF >304 seconds in 64% vs 15%; p < 0.01) in rats who underwent programmed exercise regimen with one hour treadmill training daily for 16 weeks when compared to sedentary controls. Increased vagal tone, atrial dilatation and atrial fibrosis were also reported at 16 weeks in the exercise group. Increased vagal tone was attributed due to messenger ribonucleic acid downregulation of IKACh-inhibiting RGS proteins, was present at 16 weeks in exercising rats. Detraining for 4 weeks normalized vagal tone.14 The role of IKACh in mediating cardiac response to vagal stimulation was previously described in the genesis of AF from rat models.60
Electrolyte Abnormalities
Athletes who are involved in vigorous exercise can have dynamic fluid shifts in the body which can lead to dehydration and alteration in pH and depletion of electrolytes including sodium, potassium and magnesium which may also contribute to AF.
Table 2. World Anti-doping Agency (WADA) List of Prohibited Drugs
| Anabolic Agents |
1.Anabolic Steroids
2.Other Anabolic Agents (Clenbuterol, selective androgen receptor modulators (SARMs), tibolone, zeranol, zilpaterol)
3.Peptide Hormones, Growth Factors, and related substances.
|
| Beta-2 Agonists |
|
| Hormone and Metabolic Modulators |
1.Aromatase inhibitors
2.Selective estrogen receptor modulators (SERMs)
3.Myostatin inhibitors
4.Metabolic Modulators: Insulin, (PPARδ) agonists
|
| Diuretics and other masking agents |
1.Diuretics, desmopressin
2.Plasma expanders (e.g. glycerol; intravenous administration of albumin, dextran, hydroxyethyl starch and mannitol)
|
| Stimulants |
1.Adrafinil; amfepramone; amfetamine; amfetaminil; amiphenazole; benfluorex; benzylpiperazine; bromantan; clobenzorex; cocaine; cropropamide; crotetamide; fencamine; fenetylline; fenfluramine; fenproporex; fonturacetam [4-phenylpiracetam (carphedon)]; furfenorex; mefenorex; mephentermine; mesocarb; metamfetamine(d-); p-methylamphetamine; modafinil; norfenfluramine; phendimetrazine; phenmetrazine; phentermine; prenylamine; prolintane. |
| Narcotics |
1.Buprenorphine, dextromoramide, diamorphine (heroin), fentanyl and its derivatives, hydromorphone, methadone, morphine, oxycodone, oxymorphone, pentazocine, pethidine. |
| Cannabanoids |
|
| Glucocorticosteroids |
|
| Alcohol |
1.Ethanol |
| Beta Blockers |
1.Acebutolol, alprenolol, atenolol, betaxolol, bisoprolol, bunolol, carteolol, carvedilol, celiprolol, esmolol, labetalol, levobunolol, metipranolol, metoprolol, nadolol, oxprenolol, pindolol, propranolol, sotalol, timolol. |
Swanson et al postulated that regular exercise can induce gastroesophageal reflux which may induce AF.57 The association between acid reflux disease, AF and athletes from high vagal tone remains a subject of conjecture.
A study investigated esophageal acidity in healthy athletes and controls after 80 minutes of moderate to hard sprinting. All subjects reported symptoms of acid reflux. Intra-esophageal acidity monitoring was done which showed that in controls pH< 4.0 was noted 4.9% of the time vs. 17.2% of the time for runners fed a light breakfast one hour before the run.61 Another study reported similar findings of intraesophageal acidity and acid reflux symptoms in 5/11 fasted runners and in 8/9 fed runners during or just after exercise.62
Soffer et al, reported a direct correlation between exercise (cycling at a VO2 max of 75% and 90%) and decrease in intra-esophageal pH to below 4.0. In trained cyclists exercising at VO2 max of 75% and 90%, the number of episodes when the pH decreased below 4.0 were 1.2 and 3.7 episodes/hour. In untrained cyclists the number of episodes when the pH decreased was substantially higher at 4.5 and 17.5 episodes/hour respectively.63,64
Marathon runners after a 20K race demonstrated evidence of esopghagitis on endoscopy.65 A large population study including 163,627 patients reported that acid reflux disease increased the risk of AF by 39% [95% confidence interval 1.33-1.45].66
Clinical Features and Evaluation
Symptoms such as syncope, palpitations, and dyspnea on exertion reported by athletes should be thoroughly evaluated. A detailed history and a thorough physical examination are warranted. Onset of symptoms with relation to exercise needs to be established. A history of the use of alcohol, sports supplements and energy drinks is important. AF associated in young athletes is usually paroxysmal.
Persistent AF may occur in middle-aged athletes with comorbid cardiovascular conditions. When an athlete reports palpitations it is important to exclude underlying structural heart disease such as arrhythmogenic right ventricular dysplasia, hypertrophic cardiomyopathy, or underlying conduction abnormalities such as the Brugada Syndrome, the Wolff-Parkinson-White syndrome or concealed atrioventricular bypass tracts.
The natural history of vagal-mediated AF in athletes remains unknown. A study of 30 well-trained athletes with a mean age of 48±7 years followed for nine years reported that paroxysmal AF remained stable in half of the athletes and progressed to persistent or permanent AF in relatively few athletes.21
For competitive athletes with recurrent episodes of AF, especially if rates are not controlled, symptoms are present, or exercise tolerance is reduced, activity restrictions must be considered. The need to restrict asymptomatic athletes whose ventricular rates are well-controlled is less compelling, but this may depend on the sport.
All athletes with a diagnosis of AF should undergo standard testing such as basic metabolic panel to access for underlying electrolyte abnormalities, a thyroid panel and a transthoracic echocardiography. Cardiac monitoring devices such as a Holter monitor, a cardiac event monitor or rarely, an implantable loop recorder may be used to determine if symptoms correlate with AF episodes.
Treatment of AF in athletes with either rate or rhythm control medications can be challenging. Identification of overtraining in athletes is important as reduction or temporary cessation of exercise may decrease or even prevent AF recurrence. The initial approach should be to recommend reduction of physical activity.
A study of 1772 athletes with a mean follow up of 62 months reported disappearance of AF with detraining.9 Similarly, Hoogsteen et al21 reported that sports abstinence improved symptoms of AF in athletes.
Rate control agents such as beta-blockers or calcium channel blockers may decrease performance and should be avoided, if possible, in professional athletes.
Antiarrhythmic drugs represent a reasonable choice in some athletes with AF. Flecainide may be used regularly or as a “pill in the pocket” for athletes with vagal-mediated paroxysmal AF in the absence of structural heart disease. Caution is recommended with flecainide because of the risk of proarrhythmia due to intense adrenergic hypertonia during professional sports.
Disopyramide, a class IA antiarrhythmic drug, was shown to be effective in vagal-mediated and bradycardia-dependent AF. Early small studies with disopyramide in post-cardioversion patients reported maintenance of sinus rhythm in 67% patients at 6 months and 54% at 1 year.67,68 Disopyramide is poorly-tolerated due to antimuscarinic properties and proarrhtyhmic effects.
Amiodarone a class III antiarrhythmic agent, is a potent rhythm control medication. Caution is required due to long-term toxic effects. There are no studies on the efficacy of angiotensin converting enzyme inhibitors, aldosterone antagonists and statins in vagal-mediated AF related to endurance sports.
The 36th Bethesda Conference69 recommended that athletes with asymptomatic AF can safely participate in any competitive sports in the absence of structural heart disease with maintenance of appropriate ventricular rate with no decrease in functional capacity when they were in sinus rhythm.
Risk of stroke from AF is calculated by the CHA2DS2-VASc score which assigns 2 points for age >75 years (A2), 1 point for vascular disease (V), 1 point for age 65-74 years (A), and 1 point for female gender in addition to the standard risk factors.70
In low risk athletes such as those with a CHA2DS2-VASc score of 0-1, no antithrombotic therapy is recommended. For CHA2DS2-VASc scores of ≥2, oral anticoagulation is recommended with warfarin or one of the novel oral anticoagulants. There are no data regarding the safety of novel oral anticoagulants in athletes with AF. Any form of oral anticoagulation can be a challenge due to increased risk of bleeding with sports activates.
Direct current cardioversion can be considered in athletes with AF lasting <48 hours or under TEE guidance when the duration remains unknown. Athletes returning to exercise participation after cardioversion have a high likelihood of AF recurrence due to increased autonomic hyper-activation.
The value of catheter ablation in vagal AF is emerging, with recent data supporting its role in management of AF in athletes. A study of 20 athletes (mean age 44.4±13.0 years) reported freedom from AF and antiarrhythmic therapy at 36.1 ± 12.7 months with pulmonary vein isolation. This study also reported a significant increase in exercise capacity (from 183 ± 32 to 218 ± 20 W, p < 0.02) and substantial improvement in several quality of life indicators on a self-reported questionnaire.71 All of the athletes became eligible for competitive sports >6 months after therapy. Another study including 182 subjects undergoing pulmonary vein isolation for AF reported similar arrhythmia-free survival at one year in the lone AF sport group versus controls (59% vs 48%, p=0.44), and similar rates of procedure-related complications (7.1% vs. 4.3%; p=0.45). The frequency of redo pulmonary vein isolation procedures was similar between the lone AF sport group and controls (40.5% vs 37.3%, p=0.5).72 Koopman et al studied 94 endurance athletes and reported similar AF recurrence after an initial pulmonary vein isolation procedure. However, the recurrence rate was significantly higher in non-endurance controls compared tp endurance athletes (48% vs 34%, p=0.04) after 3 years of follow-up.73 There was however, similar arrhythmia free survival at 3 years between both groups (87 vs. 85%, p=0.88). The effectiveness of catheter ablation, particularly pulmonary vein isolation, in endurance athletes is partly due to younger age and absence of diseased atria. However, the multifactorial etiology of AF in endurance athletes may be partly responsible for arrhythmia recurrence which may require a repeat procedure. Pulmonary vein isolation should be considered as a first-line therapy in endurance athletes with atrial fibrillation for arrhythmia-free survival, improvement in exercise capacity so that one can resume endurance sports practices. A redo-ablation procedure may be considered with recurrence.
Athletes who are candidates for oral anticoagulation for stroke prevention in AF prior to catheter ablation will likely remain so after the procedure.74 The issue of cessation of oral anticoagulation in athletes who remain free from AF after catheter ablation is uncertain and requires further study.
There is substantial evidence that endurance training results in exaggerated vagal tone, cardiac remodeling, inflammation and fibrosis, all of which may contribute to the onset of AF in athletes. AF is a major cardiovascular disorder which increases the risk of stroke by 5-fold, mortality by 2-fold and also impairs quality of life and exercise capacity.72 This disease should not be trivialized as a mere consequence of overtraining.
It has been recently hypothesized that exercise is associated with a U-shaped effect in terms of cardiovascular benefit. Further studies are necessary to examine the specific effects of endurance exercise on AF risk including sport specificity, duration, type, intensity in specific age groups and gender.
Long-term follow-up data regarding chronic effects of intense endurance exercise investigating training modalities and physiological factors (such as heart rate, blood pressure, VO2 max) may help in better understanding of this condition. Research in animal models examining the specific cardiovascular, cellular and molecular adaptation to intense endurance exercise is necessary.
Genetic studies including identification of specific genomes that may be vulnerable with chronic endurance exercise are required.
Several middle-aged endurance athletes may have brief episodes of atrial arrhythmia which can be triggered both increased resting vagal tone and sympathetic activation during intense physical exertion. The question remains as to whether such athletes can safely continue training. Currently, there are no guidelines on how best to manage such arrhythmias in the aging athlete. Pulmonary vein isolation via catheter ablation may be an effective strategy in these patients.
The decisions by the physician is based on clinical judgment and lack clarity of evidence. Decreasing volume and intensity of exercise is recommended. Further investigation with remote cardiac monitoring device may be warranted.
Prior completed study grants from NIH,Squbb,CPI,Geigy,Wyeth-Ayerst,Smith-Kline-Beacchum,Sanofi-Aventis,Astra-Zeneca,St. Jude, Boehringer-Ingelheim.