Heart Failure With Reduced Ejection Fraction And A Narrow QRS Complex: Combination Of A Subcutaneous Defibrillator With Cardiac Contractility Modulation
Susanne Röger MD1,2, Martin Borggrefe MD PhD1,2, Jürgen Kuschyk MD1,2
1Medical Faculty Mannheim of the University of Heidelberg, 1st Department of Medicine, Mannheim, Germany.2DZHK (German Centre for Cardiovascular Research) partner site Mannheim, Germany.
Cardiac contractility modulation (CCM) is a relatively new electrical therapy for heart failure patients with reduced ejection fraction. The majority of patients eligible for CCM will also need an implantable cardioverter-defibrillator (ICD). To-date, three pacing electrodes are mandatory for CCM therapy because the current CCM signal delivery algorithm requires sequential intracardiac sensing of a p-wave, followed by appropriately timed ventricular activation by the two ventricular septal leads. As there is no device combining CCM with ICD functions, most CCM patients will need multiple intracardiac electrodes, which increase the cumulative risk for complications such as systemic infections, thrombosis of central venous lines, insulation failures or lead fractures. The long-term complications associated with trans-venous ICD leads have led to the development of a totally subcutaneous implantable cardioverter-defibrillator (S-ICD). In this essay the two technologies CCM and S-ICD are reviewed. Additionally, we present their successful combination on the basis of a case report on the first patient receiving both devices.
Key Words : Subcutaneous Implantable Cardioverter-Defibrillator, Cardiac Contractility Modulation.
Correspondence to: Dr. med Susanne Röger
I. Medical Department
Theodor-Kutzer-Ufer 1-3
D-68167 Mannheim
Germany.
Despite strong advances in diagnostic and treatment, heart failure (HF) remains the single largest cause of mortality in the western world.1,2
Cardiac resynchronization therapy (CRT) reduces hospitalizations and mortality in patients with advanced heart failure and prolonged electrical activation (i.e., increased QRS duration).3-6 However, about 60% of patients with heart failure have a normal QRS duration and up to 30 % of patients receiving CRT do not respond to the therapy.7 In patients with a narrow QRS complex, CRT has failed to reduce the rate of death or hospitalization for heart failure and may even increase mortality.8 Thus, there is a need for alternative device-based treatments for patients with persistent symptoms despite optimal medical therapy (OMT).
Cardiac contractility modulation (CCM) is a relatively new electrical device-based technique proposed for enhancing ventricular contractile strength of the failing myocardium independent of the synchrony of myocardial contraction.9-12 CCM signals are non-excitatory electrical impulses of relatively high voltage that are applied during the absolute refractory period.
One cellular defect that underlies myocardial contractile dysfunction in heart failure is a dysregulation of intracellular calcium homeostasis. Such abnormalities reflect heart failure-associated changes in expression of genes encoding calcium handling proteins and post- lational modification of their associated proteins. These include down-regulation of genes encoding for the sarcoplasmic reticular adenosine triphosphate–dependent calcium pump, changes in expression and hypophosphorylation of phospholamban, altered regulation of the sodium-calcium exchanger, and hyperphosphorylation of the ryanodine release channel. Cardiac contractility modulation signal application is associated with normalization of phosphorylation of key proteins and expression of genes coding for proteins involved in regulation of calcium cycling and contraction. CCM experimental and clinical studies have shown a prolongation of the action potential, an increase of myocardial inotropy (also in remote areas of the myocardium) without an elevation of myocardial oxygen consumption and reverse remodeling.9-12 As the signals influence cell function without any effect on activation sequence, CCM therapy is not dependent on QRS duration and acts alongside CRT.13
Two prospective randomized multicenter studies have demonstrated improvements in NYHA functional classification: quality of life indexed by Minnesota living with heart failure questionnaire (MLWHFQ) and peak oxygen uptake (peak VO2) during cardio-pulmonary exercise testing (CPX).14,15 In a retrospective study, Schau et al. demonstrated that CCM therapy is safe, as it has no adverse effect on long-term survival.16 To date CCM therapy is recommended for patients in sinus rhythm with a left ventricular ejection fraction (LVEF) ≥25-35%, NYHA class III and normal QRS duration, as this subgroup of patients seems to benefit most from the therapy.17,18 According to the guideline-recommended selection criteria, the majority of patients eligible for CCM will also need an implantable cardioverter-defibrillator (ICD).2,19
With the current device, three pacing electrodes are mandatory, because the current CCM signal- delivery algorithm requires sequential intracardiac sensing of a p-wave, followed by appropriately timed ventricular activation by the two ventricular septal leads. Currently there is no device combining CCM with ICD functions, therefore most CCM patients will need multiple electrodes.
There are significant co-morbidities associated with device therapy related to acute and chronic transvenous lead complications. These include systemic infections, acute and chronic displacement, pneumothorax, cardiac perforation, and tamponade as well as inappropriate shocks associated with insulation failure or lead fractures.20 Cumulative data suggest that there may be at least a 20% risk of transvenous lead failure at 8–10 years post-implant.21 Failed leads often require removal, a procedure that is associated with significant morbidity and mortality.22,23 Complications are strongly associated with the number of implanted electrodes.24
The long-term complications associated with transvenous ICD leads have led to the development of a totally subcutaneous implantable cardioverter-defibrillator (S-ICD). The S-ICD System (former Cameron Health/ now Boston Scientific, Natick, Massachusetts, USA) senses, detects, and treats malignant ventricular arrhythmias (ventricular tachycardia /fibrillation) without intracardiac leads. The subcutaneous pulse generator and electrode are placed extrathoracically.25 In this report we describe the first successful combination of CCM therapy with a S-ICD device.
Cardiac Contractility Modulation (CCM)
Cardiac contractility modulation (CCM) involves the application of an electrical impulse to the cardiac muscle during the absolute refractory period of the ventricular action potential.10,11 The utilized waveform is a biphasic square wave pulse. In general, amplitudes between 10 and 20mA and durations of stimuli ranging from 10 to 20msec per phase are used. CCM signals are delivered via an implantable pacing device similar to a pacemaker (duration of therapy being 7-12 hours per day). To date, the OptimizerTM system (Impulse Dynamics Inc., Orangeburg, New Jersey, USA) is the only clinically available system. The new version Optimizer IVs is significantly smaller than its predecessor Optimizer III (29cc vs. 64 cc). The device is implanted into the pectoral region in a minimally invasive procedure and utilizes three pacemaker leads that are introduced into the right side of the heart via the subclavian vein. One of these leads is placed into the right atrium where it detects the right atrial electrical activity, which can be used to time CCM delivery. Cardiac contractility modulation signal delivery occurs through the remaining two leads positioned on the ventricular septum.
The current CCM device contains a built-in algorithm that inhibits delivery of a CCM signal when irregular electrical activity is detected, such as premature atrial or ventricular complexes or sensing defects. This is designed to eliminate the possibility of CCM signal delivery during a T-wave, which has the potential to induce arrhythmias.
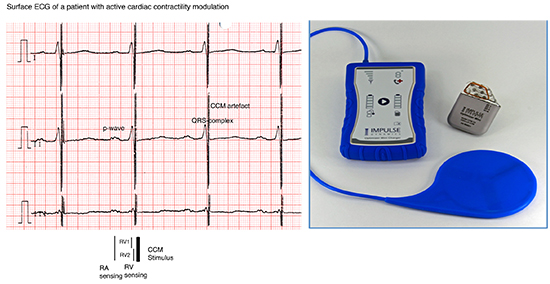
Figure 1 a shows the surface ECG of a patient with active CCM. Figure 1 b shows the current device, Optimizer IVs, and the patient’s charging device. Patients are asked to recharge their device battery once a week (time to recharge a depleted battery is 45-60min).
Figure 1. a) Surface ECG of a patient in sinus rhythm with activated CCM. The corresponding CCM algorithm is pictured at the bottom of the figure. Abbreviations: RA= right atrial, RV= right ventricular. b) Illustration of the CCM device Optimizer IV with the external charging system. (The illustration was provided from Impulse Dynamics).
The Subcutaneous Implantable Cardioverter-Defibrillator (S-ICD)
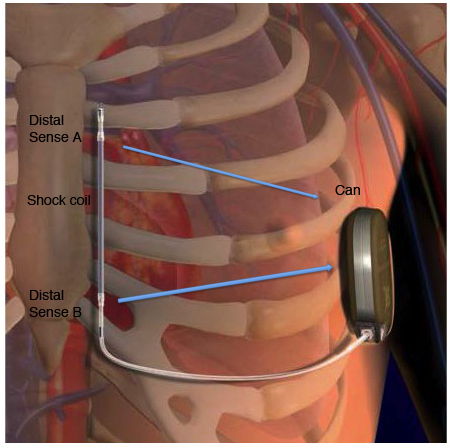
The S-ICD system25,26 consists of a 3-mm tripolar parasternal electrode (polycarbonate urethane 55 D), which is connected to an electrically active defibrillator can (Figure 2). The electrode is positioned parallel to the sternum (1 to 2cm to the left) and the pulse generator is positioned over the sixth rib at the mid-axillary line. The electrode has an 8-cm shocking coil, flanked by two sensing electrodes. The distal sensing electrode is positioned adjacent to the manubriosternal junction, and the proximal sensing electrode is positioned adjacent to the xiphoid process. Cardiac rhythm is detected by the two sensing electrodes or by either of the sensing electrodes and the active can. Three sensing configurations are available. The S-ICD automatically selects an optimal vector for rhythm detection and for avoiding double QRS counting and T-wave over-sensing. Once signals have been validated as free of noise and double detection, feature analysis and rate detection are used to discern rhythm type and determine the need for therapy. A conditional discrimination zone incorporating a feature-extraction technique can be programmed between rates of 170 and 250 beats per minute to distinguish supraventricular tachycardia from ventricular tachycardia and avoid inappropriate discharge. Testing of the device during implantation is done with the use of 65-J shocks to ensure a margin of safety. The fully deployed device delivers 80-J shocks. Patients requiring ventricular pacing are not eligible for the S-ICD as continuous pacing therapy is not possible. The device does provide 50 beat per minute post- shock pacing for 30 seconds, with the use of a 200-mA biphasic transthoracic pulse.
Figure 2. Pictoral representation of electrode and can of an S-ICD implanted at the typical operative site. Three sensing vectors are analyzed automatically to detect the optimal parameter. A-Can-Secondary vector; B-Can-Primary vector; AB-Alternate vector. Figure modified from.27
The First Patient Receiving Combined S-ICD And CCM Therapy
A 44 year-old male Caucasian patient was first diagnosed with three-vessel coronary artery disease and heart failure with reduced left ventricular ejection fraction (LVEF 25%) in 1998. He underwent three-vessel saphenous vein coronary artery bypass surgery in the same year. The patient’s coronary risk factors were arterial hypertension, hyperlipidemia, obesity grade 1 and an insufficiently controlled diabetes mellitus type 2. His heart failure medications included recommended doses of carvedilol, digitalis, angiotensin-converting-enzyme inhibitor and diuretic. An aldosterone receptor antagonist could not be administered because of stage3 chronic renal failure.
As the left ventricular ejection fraction remained low on OMT, the patient received primary prophylactic with a transvenous single-chamber ICD in 2003. Because of persistent heart failure symptoms despite optimal medical treatment, an Optimizer device (in connection with the Fix-CHF-4 study) was implanted during the same operative procedure. In the following weeks the patient’s NYHA class improved from III to II, while the left ventricular ejection fraction remained at 25%. The patient was seen in the outpatient clinic at regular intervals and in 2006 was diagnosed with AV nodal reentry-tachycardia that was successfully ablated. No further hospitalizations occurred during these years.
In April 2011 the patient was admitted to our hospital emergently with fever and rigors. Transesophageal echocardiography showed mobile densities adjacent to all intracardiac electrodes. The heart valves showed no pathology. Blood cultures were positive for staphylococcus aureus. Coronary arteriography showed open bypass grafts. The patient was transferred to the cardiac surgery unit the same day and both devices and all electrodes were successfully removed. The patient received intravenous antibiotic therapy for six weeks. Repeat transesophageal echocardiography showed no evidence of new masses and CRP levels, which had peaked at 247 mg/l, returned to normal.
In July 2011 a subcutaneous S-ICD was implanted without complications. In the following months the patient requested re-implantation of a CCM device because of recurrent heart failure symptoms resulting in a functional state of NYHA III. A new CCM device (Optimizer III) was implanted in December 2011.
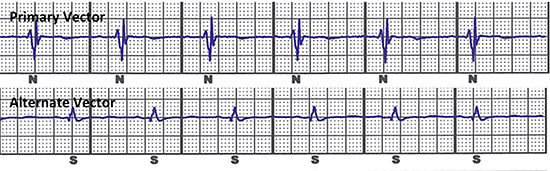
The device was implanted into the right pectoral region, one pacemaker lead was placed at the right atrium and two pacemaker leads were placed at the right ventricular septum via the right subclavian vein. In the course of the operation a cross talk test with the activated CCM device was performed using the three sensing configurations of the S-ICD. The primary vector recognized “noise” during CCM activation. The secondary vector was not eligible because of under-sensing of the ventricular signals. The alternate third vector demonstrated accurate sensing with minimal noise and absence of double detection of ventricular signals, despite active CCM stimulation (Figure 3). This sensing modality was programmed as the permanent sensing configuration. Subsequent ventricular fibrillation threshold testing was successfully performed with the induced arrhythmia terminated by a 65-Joule shock. Figure 4A and 4B show the patient’s chest x-ray.
Figure 3. Crosstalk test between S-ICD and Optimizer: a) Primary vector with an artifact of the CCM signal that is delivered during the QRS complex. The S-ICD detection algorithm observes this pattern and classifies it as “noise” (depicted by “N” in the S-ICD printout). b) Alternate vector with no substantially apparent CCM artifact. Alternate vector was programmed as permanent sensing vector. N= noise, S= sensing
On an outpatient visit in March 2014 the patient’s cardiac condition was stable. There were no further hospitalizations for cardiac reasons. The patient is currently in NYHA class II and the LVEF remains unchanged at 25%.
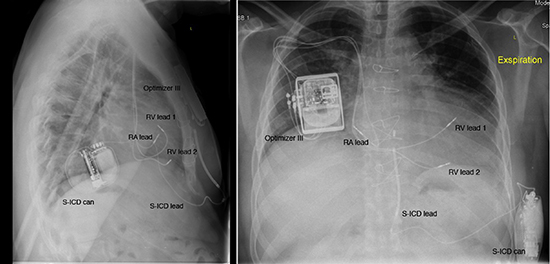
Figure 4. Chest X-ray from the first patient receiving combined S-ICD and CCM therapy. 4a: posterior-anterior view 4b: lateral view.
The two technologies S-ICD and CCM can be combined and administered successfully in patients with advanced heart failure with reduced ejection fraction. A careful intraoperative cross talk test is recommended to exclude interaction between the two devices and to avoid double counting or over-sensing.
Furthermore, a postoperative ergometer testing and provocation maneuvers are recommended (with the CCM device active), with sensing vectors being monitored in real-time. This enables observing phenomena that might appear only during exercise or tachycardia.
The S-ICD might potentially show artifacts of the CCM as noise, and in this case the sensing vector is to be selected manually.
Major requirements for a successful combination of both techniques include relatively stable sinus rhythm and the absence of significant bradycardia or a high number of ventricular premature beats. In principle, CCM is contraindicated in patients with permanent atrial fibrillation as the signal delivery is inhibited. First results of a single center case series recently demonstrated that the application of CCM signals is feasible in selected patients with permanent/persistent atrial fibrillation in case of combined application with CRT therapy.28
The combination of the two techniques S-ICD and CCM might be considered for younger patients with advanced heart failure or for patients that suffered from lead complications in the past. Ultimately, a device combining ICD, pacemaker and CCM functions would be desirable.